Dear Editor:
Pneumocephalus was first described in 1866, and the term was coined in 1914.[1] It is also known as a pneumatocele or intracerebral aerocele and may be classified as simple or tension pneumocephalus. The most common causes are craniofacial trauma, neoplasm, infection, surgical intervention, and barotrauma. Pneumocephalus has been documented most often following lumbar punctures (LPs).[1–5] It also can occur following spinal or epidural anesthesia.
One article reported an instance of pneumocephalus in a 48-year-old man after several diagnostic LPs.[2] A second case was observed in a 72-year-old woman with normal pressure hydrocephalus who developed a pneumocephalus following an LP.[3] A 50-year-old woman with disequilibrium experienced an LP complicated by tension pneumocephalus,[4] and another reported case was in a 35-year-old woman evidencing a pneumocephalus after having an LP performed for spontaneous intracranial hypotension.[5]
Vignette. A 74-year-old, right-handed, Caucasian man with history of alcohol abuse, hypertension, and insulin-dependent diabetes mellitus presented with receptive aphasia, acalculia, and agitation. New-onset atrial flutter was observed. Magnetic resonance imaging (MRI) revealed a left middle cerebral artery stroke with hemorrhagic conversion. During hospitalization, the patient evidenced severe alcohol withdrawal, including delirium tremens. His alcohol withdrawal was treated without much clinical benefit. Fentanyl was then administered to calm agitation and facilitate an LP in order to rule out encephalitis. An 18-gauge needle was utilized, and the procedure completed in the decubitus position. Following some clinical deterioration, a computerized tomography (CT) scan of the head without contrast one hour after the procedure revealed pneumocephaly in the middle cranial fossae, likely induced by the LP (Figure 1).
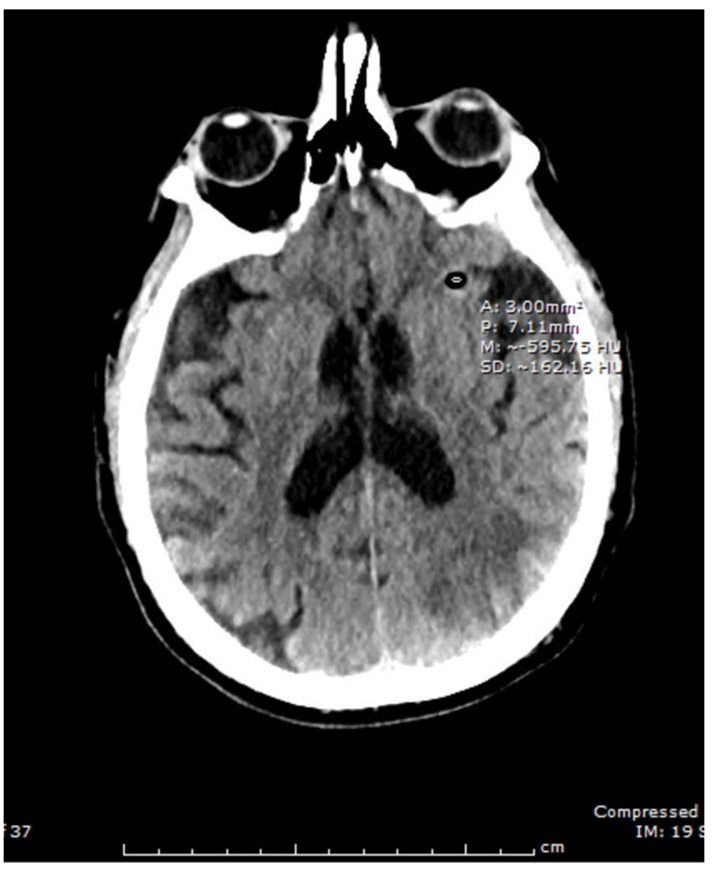
Discussion. Pneumocephalus is defined by two mechanisms: a ball-valve and an inverted bottle concept.1 The ball-valve type implies positive pressure events, such as coughing or valsalva maneuvers, that prevent air escape. Tension pneumocephalus is included in this mechanism, causing a parenchymal mass effect. The inverted bottle theory includes a negative intracranial pressure gradient following cerebrospinal fluid drainage, relieved by air influx. A small pneumocephalus is usually sealed by blood clots or granulation, allowing spontaneous reabsorption and resolution.[1] Otherwise, the lateral positioning of a patient during spinal tap might create a lower intrathecal pressure with air being allowed into the subarachnoid space. Pneumocephalus also can develop when a stylet is reinserted into the needle before needle retraction, usually performed to minimize post-dural-puncture headache.[6]
Pneumocephalus can be avoided by performing the LP in a sitting position, monitoring the amount of fluid drainage, carefully replacing the stylet to make sure the needle does not contain air, and instructing patients to briefly hold their breath and prevent making sudden movements during the procedure.[3]
It is also important to consider needle size during a spinal tap. A smaller gauge makes a smaller dural perforation, causing less damage compared to larger ones; that also prevents cerebrospinal fluid leakage.[7,8] There is an inverse correlation between the needle gauge and post-dural-puncture headache.[8,9] The incidence of headache decreases by 1.4 percent per unit increase in the gauge.[8]
Additionally, it is necessary to consider the longer time required for the procedure while using smaller needles (e.g., 25 gauge). It takes more time because introducers are needed, smaller needles require aspiration of cerebrospinal fluid, and it takes longer to collect the required fluid volume. Research documents that the smaller needles are safe and that adequate amount of fluid can be collected.9 Physicians will require additional training using this method, however.
Comment. Pneumocephalus, though a rare complication of LP, has increased recently in frequency. The occurrence of a pneumocephalus after a diagnostic or therapeutic LP procedure might worsen a presenting condition and might also lead to complications, such as a tension pneumocephalus. Pneumocephalus induced by an LP often resolves without intervention; conservative measures include bed rest, head elevation, avoidance of positive pressure, and pain control. During an LP, consider utilizing a smaller sized spinal needle to minimize this complication.
With regard,
Murali K. Kolikonda, MD; Priyanga Jayakumar, MD; Srividya Sriramula, MD; and Steven Lippmann, MD
Dr. Kolikonda is from the Department of Neurology, Dr. Jayakumar is from the Division of Infectious Diseases, Dr. Sriramula is with Internal Medicine, and Dr. Lippmann is from the Department of Psychiatry, University of Louisville School of Medicine, Louisville, Kentucky.
Funding/disclosures: No funding was provided. The authors have no conflicts of interest relevant to the content of this letter.
References
- Schirmer CM, Heilman CB, Bhardwaj A. Pneumocephalus: case illustrations and review. Neurocrit Care. 2010;13(1):152–158.
- Flora GS, Tuchschmid JA, Sharma OP. Pneumocephalus in association with lumbar punctures. Chest. 1990;98(4):1041.
- Kozikowski GP, Cohen SP. Lumbar puncture associated with pneumocephalus: report of a case. Anesth Analg. 2004;98(2):524–526.
- Nelson AS, Jafari A, Shah P, et al. Pneumoencephaly following lumbar puncture in association with an ethmoidal osteoma and porencephalic cyst. J Neurol Neurosurg Psychiatry. 2007;78(10):1149–1151.
- Girauda P, Chauvet S. Secondary pneumocephalus after lumbar puncture: An unusual complication of spontaneous intracranial hypotension? Clin Neurol Neurosurg. 2013;115(10): 2204–2206.
- Tran P, Reed EJ, Hahn F, et al. Incidence, radiographical features, and proposed mechanism for pneumocephalus from intravenous injection of air. West J Emerg Med. 2010;11(2):180–185.
- O’Connor G, Gingrich R, Moffat M. The effect of spinal needle design, size, and penetration angle on dural puncture cerebral spinal fluid loss. Am Assoc Nurse Anesthetists J. 2007;75(2):111–116.
- Zorrilla?Vaca A, Healy R, Zorrilla?Vaca C. Finer gauge of cutting but not pencil point needles correlate with lower incidence of post dural puncture headache: a meta regression analysis. J Anesth. 2013. Doi: 10.1007/s00540-016-2221-2.
- Bertolotto A, Malentacchi M, Capobianco M, et al. The use of the 25 Sprotte needle markedly reduces post-dural puncture headache in routine neurological practice. Cephalalgia. 2016;36(2):131–138.




