 by Rishikesh V. Behere, MD; Mukund G. Rao, MD; Shree Mishra, MD; Shivarama Varambally, MD; Shivashankar Nagarajarao, PhD; and Bangalore N. Gangadhar, MD
by Rishikesh V. Behere, MD; Mukund G. Rao, MD; Shree Mishra, MD; Shivarama Varambally, MD; Shivashankar Nagarajarao, PhD; and Bangalore N. Gangadhar, MD
Dr. Behere is with the Department of Psychiatry, Kasturba Medical College, Manipal University, Manipal, Karnataka, India; Dr. Rao is Registrar, North West Area Mental Health Service, Coburg, Melbourne, Australia; Drs. Mishra, Varambally, and Gangadhar are with the Department of Psychiatry, National Institute of Mental Health & Neurosciences, Bangalore, Karnataka, India; and Dr. Shivashankar is with the Department of Speech Pathology and Audiology, National Institute of Mental Health and Neurosciences, Bangalore, Karnataka, India.
Innov Clin Neurosci. 2015;12(7–8):31–33.
Funding: No funding was received for the preparation of this manuscript.
Financial disclosures: The authors have no conflicts of interest relevant to the content of this article.
Key words: Primary Auditory Neuropathy, Anxiety Disorder, Social Anxiety, Diagnostic confusion, Audiometry
Abstract: The authors report a case of a 47-year-old man who presented with treatment-resistant anxiety disorder. Behavioral observation raised clinical suspicion of auditory neuropathy spectrum disorder. The presence of auditory neuropathy spectrum disorder was confirmed on audiological investigations. The patient was experiencing extreme symptoms of anxiety, which initially masked the underlying diagnosis of auditory neuropathy spectrum disorder. Challenges in diagnosis and treatment of auditory neuropathy spectrum disorder are discussed.
Introduction
Auditory neuropathy spectrum disorder (ANSD) is the consensually approved terminology[1] in the literature to describe a disorder with wide variations in clinical symptomatology and audiological manifestations. The presumed sites of lesions for this disorder occur within the auditory system and include the inner hair cells (the sensory cells of the cochlea), the synapses between the inner hair cells and the fibers of the VIII nerve (vestibulocochlear nerve), the ganglion neurons, the VIII nerve fibers themselves, or any combination of these sites.[2] Hearing acuity may vary from normal hearing to severe hearing loss and may also demonstrate fluctuations in hearing threshold.[3]
The cardinal feature of ANSD is speech perceptual difficulty that is disproportionate to the hearing acuity of the individual. Patients with ANSD often demonstrate good identification of nonspeech sounds; however, the presence of specific difficulties in understanding speech often leads to significant disability in social interactions and may even impact psychosocial well-being.[4]
We report a case of a man who presented with anxiety disorder that was resistant to conventional treatment with anti-anxiety agents. The diagnosis of ANSD was missed initially as it was overshadowed by the anxiety disorder. Eventually, a diagnosis of ANSD was confirmed via audiological investigations. Consent was obtained from the patient to report this case.
Case Report
Mr. B was a 47-year-old man who was referred to the psychiatry outpatient services of a tertiary referral neurosciences center by his treating psychiatrist for evaluation of anxiety symptoms that were not responding to a conventional anti-anxiety regimen. The patient primarily reported feeling anxious in social situations and during conversations with his superiors at his place of employment over the last 25 years. The anxiety was associated with autonomic arousal, thoughts of being scrutinized by others, and avoidance of social situations. Mr. B’s family members described him as shy and reserved since childhood, with no intellectual disability. His past medical, psychiatric, and developmental history was uneventful. Detailed physical examination and biochemical tests inclusive of renal, liver, thyroid functions, serum electrolytes, and fasting blood glucose were normal. Mr. B was currently taking escitalopram for anxiety.
Mr. B’s clinical presentation fulfilled criteria for social phobia as per the International Statistical Classification of Diseases and Related Health Problems, Tenth Edition (ICD-10).[3] However, during the clinical interview, Mr. B was observed to have difficulty in understanding our questions unless they were repeated two to three times. He attributed his anxiety to difficulty in understanding conversations, a symptom that had been present since childhood. He reported continued difficulty understanding instructions from his superiors at work that affected his work performance and made him feel more anxious. His anxiety was most pronounced during phone conversations. Hence, the specific sound of a mobile ringtone or a ringing land phone would trigger autonomic arousal in him that was characterized by palpitations, sweating, tremors, and dryness of mouth.
Examination by the otorhinolaryngologist ruled out any middle ear pathology. Magnetic resonance imaging (MRI) of the brain and an electroencephalography (ECG) did not reveal any abnormalities. Consultation from the Department of Speech Pathology and Audiology was sought for the assessment of his difficulties in perceiving speech.
The audiological history was ascertained and reconfirmed. A host of audiological tests were administered that included pure tone and speech (speech recognition threshold [SRT], speech identification score [SIS], and speech-in-noise [SPIN] test); audiometry acoustic stapedius reflex test (ASRT); auditory brain stem responses (ABR); distortion product otoacoustic emissions (DPOAE); gap detection threshold (GDT); and dichotic digits test (DDT). These audiological tests were performed using standard clinical test procedures. The audiological test results are presented in Table 1.
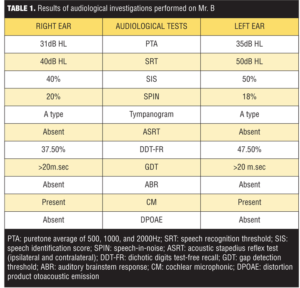
The patient demonstrated the following: mild-to-moderate sensorineural hearing loss (pure tone average [PTA] of 500Hz, 1K.Hz, and 2K.Hz: right ear 31.6dB, left ear 35dB), absence of acoustic stapedius reflex with “A” type tympanograms, and absence of ABR with presence of cochlear microphonics. The speech identification score was poor (right ear 40%, left ear 45%) and was pronounced under speech-in-noise conditions (right ear 20%, left ear 18%). The DDT demonstrated bilateral suppression (right: 37.5%, left: 47.5%). The GDT was greater than 20m.sec in both ears, which suggested impairment in temporal resolution. The audiological findings indicated a diagnosis of ANSD, although the otoacoustic emissions (OAE) were absent in both ears.
Discussion
Mr. B initially presented with social anxiety disorder, and through the course of interviews, he was observed to have difficulties in speech perception, which led to an audiological evaluation with a clinical suspicion of an auditory processing disorder. The diagnosis of ANSD was made based on the audiological findings of absent ABR and acoustic reflex in the presence of bilateral mild-to-moderate degree of hearing loss and the presence of cochlear microphonics on ABR with poor speech identification score disproportionate to the hearing loss. The presence of cochlear microphonics in this patient, which is a pre-neural response, suggested the integrity of outer hair cells. However, this was not evidenced on OAE. Space-occupying lesions at the brainstem level were ruled out through neurological examination and radiological investigations.
Although the OAE is used as a differential diagnostic tool and is often present in patients with auditory nerve dys-synchrony, it was absent in this patient, making our diagnosis challenging. Starr et al[5] report that in 30 percent of patients with ANSD, the OAE is absent. Deltenre et al[6] attribute the loss of OAE in the presence of preserved cochlear microphonics to the dysfunction of the cochlear amplifier, which would add to the initial synchronization deficit in such patients. This could be the possible mechanism for the absence of OAE in our patient too. The patient also demonstrated impaired temporal resolution (gap detection >20m.sec in both ears). Being one of the basic components for speech perception, impaired temporal resolution may significantly alter an individual’s ability to perceive speech. This factor along with poor dichotic perception (inability in binaural separation) may have contributed to the significant impairment in verbal comprehension by Mr. B.
Mr. B also reported erectile dysfunction, which was possibly related to the escitalopram he was taking for anxiety. Medications were reassessed by the clinical team, and Mr. B was started on mirtazapine 30mg/day; the escitalopram was discontinued. In addition, education regarding his disability and incorporation of behavioral modifications that included practicing speechreading (i.e., lip reading) skills, asking his secretary to take down notes for him, and participating in yoga therapy were initiated. After these measures were in place, Mr. B reported a better level of functioning in his day-to-day office work. However, his most distressing symptom, autonomic arousal on hearing telephone ringtones, persisted. This symptom was possibly confounded by Mr. B’s inability, when speaking on the phone, to use visual cues (i.e., speechreading) from the person with whom he was speaking. While Mr. B’s difficulty in comprehending speech made a formal cognitive behavior therapy approach difficult, his autonomic arousal symptom did improve with a technique of thiopentone-assisted systematic desensitization.[7]
Mr. B was seen for follow-up on two occasions over a three-month period after initiation of the desensitization sessions. On his final follow-up visit, he subjectively reported a 75-percent improvement in his anxiety symptoms and phone ringing phobia by utilizing a combination of mirtazapine, behavioral interventions, yoga therapy, and five desensitization sessions. His sexual dysfunction had also resolved.
Conclusion
Presence of psychiatric symptoms that have been long-standing and unresponsive to conventional pharmacotherapy and the presence of defects in perceiving speech should raise clinical suspicion of a possible underlying neuro-developmental condition. Our patient’s severe anxiety symptoms initially masked the presence of ANSD. Once the proper diagnosis was made, the ANSD was effectively managed through an interdisciplinary and multimodal treatment approach, and the patient improved significantly. In cases of ANSD with comorbid psychiatric symptoms, we recommend an individualized treatment plan that incorporates the use of alternative communication strategies and behavioral modifications (e.g., enhancing the patient’s speechreading skills and utilization of face-to-face conversations, reducing competing noices in certain auditory environments, and speaking more slowly while conversing), along with appropriate pharmaco- and psychotherapies.
References
1. Northern J (ed). Guidelines for Identification and Management of Infants and Young Children with Auditory Neuropathy Spectrum Disorder. Aurora, CO: The Children’s Hospital; 2008.
2. Starr A, Picton TW, Sininger Y, et al . Auditory neuropathy. Brain. 1996;119:741–753.
3. World Health Organization. International Statistical Classification of Diseases and Related Health Problems, 10th Revision (ICD-10). Geneva: WHO; 1992.
4. Shivashankar N, Satishchandra P, Shashikala HR, Gore M. Primary auditory neuropathy—an enigma. Acta Neurol Scand. 2003;108(2):130–135.
5. Starr A, Sininger Y, Nguyen T, et al. Cochlear receptor (microphonic and summating potentials, otoacoustic emissions) and auditory pathway (auditory brain stem potentials) activity in auditory neuropathy. Ear Hear. 2001;22:91–99.
6. Deltenre P, Mansbach AL, Bozet C, et al. Auditory neuropathy with preserved cochlear microphonics and secondary loss of otoacoustic emissions. Audiology. 1999;38:187–195.
7. Pearlman T. Behavioral desensitization of phobic anxiety using thiopental sodium. Am J Psychiatry. 1980;137:1580–1582.
