 by Stacy Liechti, PhD; Gianna Capodilupo, MA; Douglas J. Opler, MD; Mark Opler, PhD, MPH; and Lawrence H. Yang, PhD
by Stacy Liechti, PhD; Gianna Capodilupo, MA; Douglas J. Opler, MD; Mark Opler, PhD, MPH; and Lawrence H. Yang, PhD
Dr. Liechti is Lead Research Consultant at the PANSS Institute in New York, New York. Ms. Capodilupo is Research Assistant at MedAvante-ProPhase in New York, New York. Dr. D. Opler is Assistant Professor in the Department of Psychiatry at Rutgers New Jersey Medical School in Newark, New Jersey. Dr. Opler is Adjunct Assistant Professor at NYU School of Medicine and Chief Research Officer at MedAvante-ProPhase Inc. in New York, New York. Dr. Yang is Associate Professor of Social and Behavioral Sciences at New York University in New York, New York.
Funding: No funding was provided for this article.
Disclosures: The authors have no financial conflicts relevant to the content of this article.
Abstract: Psychometric instruments are products of their time— Their designs and initial purposes are influenced and shaped by the contemporary treatment regimens, context, and cultural and conceptual biases of their developers. In this review article, the authors explore the history of the most influential schizophrenia research tools that have been created over the past several decades. The authors describe the scientific concepts, cultural influences, and challenges of past and present researchers as they strive to develop better assessment tools for schizophrenia. Starting with Moore’s Scheme for the Quantitative Measurement of Abnormal Emotional Condition, developed in the early 1900s, and concluding with Kay, Fiszbein, and Opler’s Positive and Negative Syndrome Scale, developed in the 80s, the authors describe several scales and illustrate how each scale led to and influenced the development of a later scale. The authors hope that a better understanding of schizophrenia assessment tool evolution and limitations will assist in the development of new instruments that better address the global needs for the evaluation, research, and treatment of psychosis.
Keywords: Positive and Negative Syndrome Scale (PANSS), Brief Psychiatric Rating Scale (BPRS), Inpatient Multidimensional Psychiatric Scale (IMPS), Multidimensional Scale for Rating Psychiatric Patients (MSRPP), psychometrics, symptoms, psychosis
Innov Clin Neurosci. 2017;14(11–12):12–17
Introduction
Our rating scales, diagnostic instruments, and psychometric tools are not created in a vacuum; rather, they are products of their time, with input from culture, biases, and what is considered to be state of the art in psychopathology and psychopharmacology at the time of their development in. The Positive and Negative Syndrome Scale (PANSS) is no exception. It was developed during a time in which negative symptoms were gaining broad acceptance as separate constructs of schizophrenia, and the scale was utilized in the first wave of studies for the earliest second-generation antipsychotics.
The PANSS and other instruments like it affect and are affected by how we conceptualize mental illness. The purpose of this review is twofold: first, to provide a historical narrative of the events that led to the creation of the PANSS, and second, to identify some of the implicit and overt cultural assumptions and statements that have played a role in the development of this psychometric instrument.
The Rise of Mental Disorder Awareness in the United States
By the mid-1940s, there was growing awareness in the United States of the extent and severity of mental disorders. By 1944, nearly half of the individuals dismissed from the armed services were discharged for reasons of mental health, a far greater loss of manpower than that seen due to influenza, battle wounds, malaria, or any other single illness.1 Data from the selective service records echoe this at-the-time profound revelation: mental illness was listed as the sixth most common “defect” among service members, with a prevalence rate of 55.8 per 1,000 men.2 This discovery, for the United States government, was more than simply a health crisis but also a crisis of training and education, economics, and, most importantly, a crisis that posed a threat to national security. If the incidence of mental illness, particularly psychosis, appeared so abundantly among a subgroup of the country’s population, how prevalent might it be across the nation as a whole? Congress signed the National Mental Health Act in 1946, and, on April 15, 1949, the National Institute for Mental Health was formally established. The year 1946 also saw the establishment of the Clinical Psychology Section and the Psychiatry and Neurology Sections in the Veterans Administration (VA) Central Office to oversee and respond specifically to treatment efforts and ongoing research in VA hospitals and regional offices across the country.
The Birth of Psychometrics
As early as in 1951, in an article published on the symptomatology of psychosis, psychologist J. R. Wittenborn stated very clearly that the culture of the researcher might have a strong influence on the science of phenomenology. He cautioned that the clustering of symptoms in his own data might have been due to “patterns of belief and techniques of examination” prevalent among contemporary New England psychiatrists. That is to say, psychiatrists who are different in cultural background might possibly rate patients so differently that the appearance of different symptom patterns would result. It is also possible that the forms of behavior by which mental illness is manifested are in some way culturally determined; this possibility can be examined only by making intercultural comparisons for symptom patterns among the mentally ill.”3
Psychometrics can be referred to as an objective, quantitative evaluation relying substantially on statistical methods. At its inception, the field of psychometrics was intended to describe and classify “abnormal behavior” with the assumption that there was a shared etiology and specific symptom expression for each disease area. Few psychometric instruments existed prior to World War II. Father Thomas Verner Moore’s (1877–1969) “Scheme for the Quantitative Measurement of Abnormal Emotional Conditions” was one of the few statistically derived measures available at the time and the first one constructed via a factor analysis of patient symptomatology.4 Moore sought to evaluate the classification and differentiation of syndromes of psychosis in the light of Kraeplin’s work. He drew heavily on the statistical methods of his former classmate and colleague, Charles Spearman, particularly his idea of factor analysis, to analyze the psychometric data he collected.5 Moore primarily collected his data from interviews and ward observation of 367 male and female patients who were functionally psychotic. His findings supported Kraeplin’s classifications and further concluded that manic-depressive syndrome and dementia praecox were in reality five highly correlated syndromes (catatonic, deluded and hallucinated, paranoid irritability, cognitive defect, and constitutional hereditary depression) that all shared common etiological factors.4
Following Moore’s psychometric advances, no other instruments grounded in factor analysis of data were developed until World War II. Between 1943 and 1953, more than 15 new rating scales and checklists were developed and published to evaluate psychiatric patients on the ward or during clinical interview.6 It was in 1951 that chlorpromazine, the first neuroleptic, was introduced.7 The introduction of tranquilizers as treatment options helped to fuel this demand for the use of statistical measurements in comparing the efficacy of these drugs. The bulk of the investigations of new drug treatments fell to
the VA.2
Maurice Lorr’s Multidimensional Scale for Rating Psychiatric Patients
In the 1950s, VA psychologist Maurice Lorr began a series of studies with the objective of providing a more efficient framework for describing the symptomatology of psychoses, conducting therapeutic evaluation, and measuring patient change.8 For Lorr, this required precise psychometric instruments.9 Though Kraeplin’s system was still in use during the early post-World War II era, Lorr rejected Kraeplin’s typological approach and instead proposed a method in which not all elements of a syndrome needed to be present for a patient to be assessed and diagnosed.
Lorr and fellow VA psychologists Richard Jenkins and James O’Connor conducted a factor analysis of data collected on the “Northport Record.” This early Lorr measure comprised rating scales derived from data on functional psychotic patients at the VA hospital in Northport, New York.10 Lorr and colleagues later revised the “Northport Record” to create a new psychometric instrument, the Multidimensional Scale for Rating Psychiatric Patients (MSRPP). The MSRPP was designed to measure symptom severity and changes in patients with psychoses who had been lobotomized. The instrument and its symptom inventory consisted of two sections: 1) an interview section rated by a psychiatrist or psychologist and 2) a ward section completed by nurses or other staff members following an observation period. The MSRPP also had an alternative form for use with outpatients.6 Lorr was passionate about the use of rating scales for objective recording and evaluation. His review of quantitative measurements suggests he thoroughly understood that having a familiarity with the patient being interviewed was crucial to accurately understanding the patient’s symptomology.7 This measure demonstrated these beliefs and the importance of behavioral observation as part of a symptom rating scale, a feature that was adopted by the PANSS many decades later.
The MSRPP and the other scales created during and directly following World War II had fundamental issues for Lorr, both in the process by which data were collected and in the manner in which those data were classified. Lorr remained uneasy with the use of interviews and observation as the key components in assessing psychopathology and its expression. The problem for Lorr was one of “developing controlled interview patterns … and of objectively recording what the trained clinician can validly or reliably observe or infer.”6 Lorr and his contemporaries reviewed, analyzed, and conducted additional studies to identify salient symptoms and to evaluate available classifications. However, the factors that Lorr had hypothesized and his rating scales had many similarities to those developed by his peers. This might have been due to the influence of authoritative prior work by Moore, the fact that Lorr and his peers all used similar methodologies, and the fact that all worked with similar patient populations.3,10
Lorr tested his hypotheses among veteran psychotic patients from five VA hospitals. He attempted to include a representative cross-section of the patient population in terms of their symptom severity and the duration of their stay at the hospital.6 With the study results, an additional factor analysis of the MSRPP, and results of comparisons with other studies conducted during the 1950s, Lorr condensed his list of factors from the 12 appearing in the MSRPP to the 10 he had identified in all cases.
Maurice Lorr’s Inpatient Multidimensional Psychiatric Scale
The Inpatient Multidimensional Psychiatric Scale (IMPS) was designed to measure the 10 psychotic syndromes, described by Lorr, that were established by repeated factor analyses of the instrument’s authors.12 Lorr also validated the 10 hypothesized syndromes from the prior factor analyses reported by Degan, Wittenborn, and Guetin, but only considered those syndromes that could be evaluated through clinical interviews.10 He asserted that the actual formulation for the syndromes was based primarily on empirical analyses and thus was unhampered by theoretical or diagnostic biases—a premise that was heavily critiqued by others.11,15 With the IMPS, Lorr also sought to classify several syndrome-based patient types, showing that there were six in all. He hoped this finding would spark a reexamination of the 1952 version of the Diagnostic and Statistical Manual of Mental Disorders (DSM). Rather than securing an intellectually derived consensus approved by the members of the American Psychiatric Association, he sought instead to introduce observational and statistically driven approaches to typology.9,10
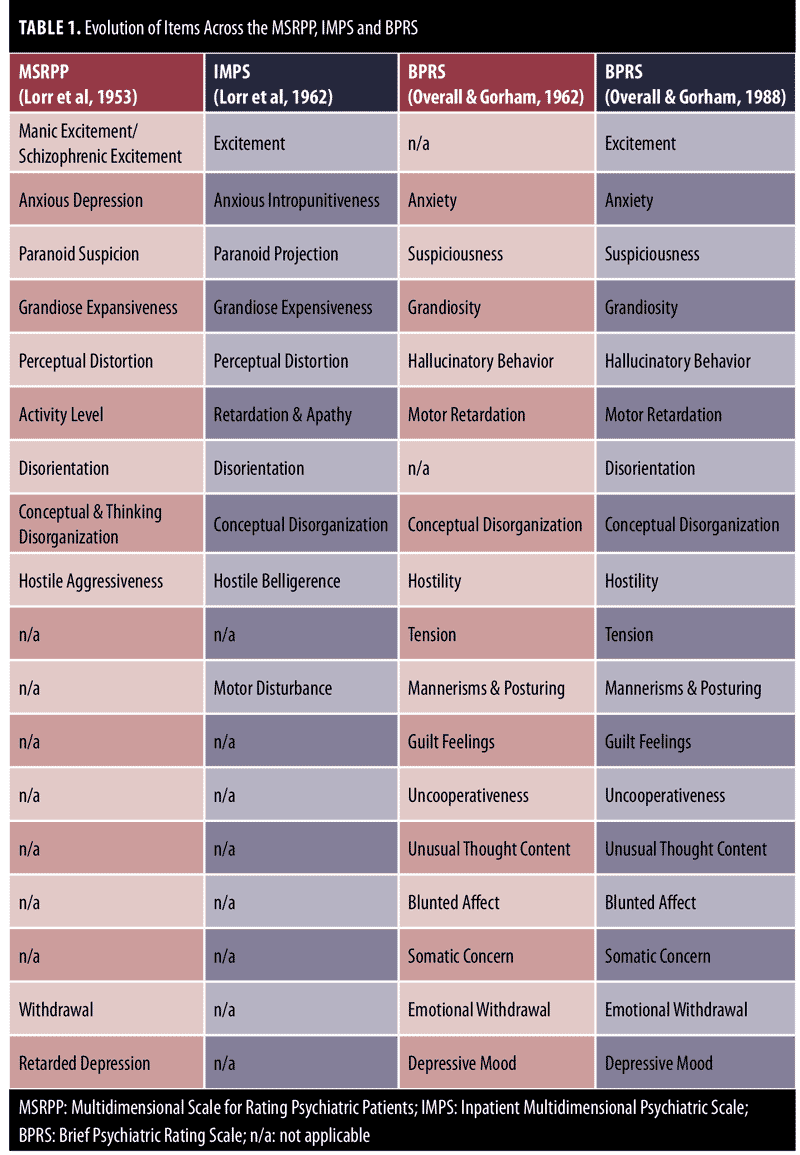
Lorr et al17 evaluated versions of the scale and constructs using data from a national study on the effects of medications. Multiple group factor analysis was conducted based on hypothesized groupings of variables and it yielded the same 10 syndromes as the initial unrevised form, thus providing evidence of the validity of these syndromes to the authors of the IMPS.16 The final instrument comprised 75 items and the MSRPP, with several exceptions. The most obvious was the list of 10 syndromes (Table 1). Lorr also eliminated the “unratable” category, converted the bipolar scales into unipolar continua, and added two sets of descriptors to express intensity and frequency in some of the scales.10 He furthermore emphasized precision, clarity, and utility, with the goal of improving the reliability of the IMPS. At the time, he viewed the processes of diagnosis and assessment to be in disarray and the psychiatric and psychological training programs to still be in their infancy.
Lorr anticipated that the individuals who would likely use the IMPS had experience in interviewing psychiatric patients and were familiar with psychosis. At the time, there was no standardized procedure for conducting a psychiatric interview. For the IMPS, it was recommended that interviewers check their ratings against another rater during their first administrations. To assure reliability, Lorr recommended the routine use of two raters to describe a single patient. Raters were advised to come to consensus when their opinions differed, but Lorr considered it permissible to average ratings. As he himself noted, his scales were equally a test of the presence of severity of a patient’s symptoms as well as a test of the clinician’s ability to detect those symptoms.12
Lorr openly acknowledged the limitations of his instrument. Though it demonstrated good internal consistency and strong inter-rater reliability, the instrument’s overall validity remained in question. As designed, the IMPS was intended for use in research and patient management. While Lorr anticipated that the IMPS would be able to detect change over time, some aspects of the IMPS did not appear to support his assumption that open-ward patients would exhibit less severe symptomatology across the instrument’s domains. Lorr found that scores of the Disorientation, Anxious Intropunitiveness, and Retardation and Apathy categories were not as reduced over time as he had hypothesized.
Lorr next turned his attention to typology with the IMPS.11 Lorr’s approach reveals much about his view of psychopathology and the place of the clinician or researcher in time and context. His overarching goal of freedom from bias was difficult to achieve, as even his multivariate analytic results were shaped by prior data, findings, and conceptualizations.16,17 As a concluding thought in the IMPS manual, he expressed his reservations regarding the possibility of an abbreviated version of the IMPS. Lorr maintained that it was necessary to have redundancy so that each syndrome could be defined by its range of behaviors rather than be limited by a single characteristic.8 He feared that reducing the instrument into a global scale for each syndrome weakened both its reliability and validity. The creation of such an instrument, in Lorr’s opinion, would push psychiatry back a decade toward the time of the first DSM, where subtypes were characterized by a singular and unidimensional feature—the model against which Lorr was working. Despite this criticism, future scales would strike a balance between item reduction and comprehensive evaluation, highly structured interview approaches, and global summaries of symptomatology.
Gorham, Overall, and the Brief Psychiatric Rating Scale
In the late 1950s, John Overall was one of the first researchers to benefit from the new psychiatric training programs established post-World War II. Overall was assigned the task of evaluating existing psychometric instruments and developing new ones for use in the VA’s psychiatric studies, particularly those aimed at examining the efficacy of drug treatment in comparison with other treatment methods. It was during this time that Overall began his lifelong collaboration with clinical psychologist John Gorham. Concurrent with Lorr’s development of the IMPS, Overall and Gorham began a series of studies that resulted eventually in the birth of the Brief Psychiatric Rating Scale (BPRS).
Gorham and Overall perceived a need for an instrument tailored to measure the efficacy of drug treatments but that would not be burdensome for the staff at psychiatric hospitals to administer. Gorham and Overall found the MSRPP, the foundational starting point for the BPRS, to be ineffective in evaluating drug efficacy because it did not possess sufficient specificity to assess changes in symptoms according to a certain type of drug.19 Thus, they developed their own set of drug-change scales from the MSRPP that were sensitive to medication effects. In their minds, the efficiency of a brief scale depended on the inclusion of items that were especially sensitive to drug change, such as Unwarranted Suspicion, Hallucinatory Behavior, Disorientation, Tension-anxiety, Inaccurate Self-concept, Emotional Responsiveness, Conceptual Disorganization, Mannerisms and Posturing, and Guilt and Dread.
The product of these efforts was an experimental version of the BPRS, in which raters were asked to make a global rating of the severity of the pathology for each symptom construct.19 The reliability of these 14 items was tested at the VA. Gorham and Overall recommended that two clinicians jointly interview a patient using the BPRS and then have the raters make independent ratings to ensure reliability.20 A single rating for each scale item was to be determined by consensus in instances in which scores were different. Averaging scores was not permissible, although this convention has been largely disregarded in subsequent decades.21
Prior to publishing the BPRS, Gorham and Overall added two additional scale items to the 14 items from the experimental BPRS: “Unusual Thought Content” and “Blunted Affect.” A small committee of psychologists and psychiatrists determined that these items were crucial to include even if factor analysis had minimized their significance.22 By including a single scale to record the symptomatology of relatively independent symptom areas, Gorham and Overall created a tool for the concise and speedy evaluation of change due to treatment in psychiatric patients and provided a comprehensive description of symptom characteristics. However, the BPRS authors also stated that the Lorr scales, which had more items, should be used in instances where time permits.
In 1965, Gorham and Overall added two additional items, “Excitement” and “Disorientation,” to the BPRS, bringing the item total to 18.23 While Gorham and Overall had outlined the basic structure of the BPRS interview, in 1988, Rhoades and Overall suggested a number of possible lead questions that would ensure each of the content domains would be covered during the BPRS interview process, with the understanding that interviewers would modify the questions and follow-up as each situation demanded.24 The authors felt that this semi-structured interview methodology was consistent with the guiding principle of the BPRS wherein symptom constructs are abstract and the symptoms themselves can be more fluid, as opposed to past scales in which symptomology is rigid.
The same perception of symptom manifestations and symptom constructs deterred Overall and his colleagues from officially including anchoring points for their scales or officially endorsing the anchoring point schemes proposed by others. While introducing anchoring points to the BPRS would allow researchers to predetermine threshold values on items, the arguments against this revision to the instrument stemmed from other concerns. Overall asserted that the BPRS was aimed at capturing global assessments of pathologies that were not the sum of individual ratings of symptoms and behaviors.24
Stanley Kay, Lewis Opler, and the PANSS
By the 1980s, the discourse of psychiatry in the United States began to embrace a different epistemology—a dimensional approach to psychopathology—that steadily replaced the typological framework favored in earlier decades. The early 1980s saw the reinvigoration and elaboration of a two-dimensional model for schizophrenia, largely at the hands of British psychiatrist Timothy Crow.25,26 Crow hypothesized the existence of a phenomenology and neurobiology based on the concepts of positive and negative symptoms that might mark separate syndromes or disease process. This dichotomous explanation of schizophrenic pathology found favor among many circles and fostered the construction of a set of measurements to determine symptom severity, such as Nancy Andreasen’s Scale for Assessing Positive Symptoms (SAPS) and Scale for Assessing Negative Symptoms (SANS). These new instruments did not, however, satisfy all researchers.
While treating patients at the Bronx Psychiatric Center in the late 1970s and early 1980s, Lewis Opler noticed changes in patient symptomatology that did not cohere entirely with the scholarly literature to date. Contrary to findings by Angrist, Rostrosen, and Gershon published in 1980,27 Opler observed a marked improvement in negative symptoms after administering levodopa (L-DOPA) to counteract the motor side effects induced by neuroleptics in patients diagnosed with schizophrenia.26 It had been thought that while negative symptoms were indicative of disorders such as schizophrenia, these symptoms were attributed to structural defect and therefore would not be responsive to drug therapy. Unfortunately, the “gold standard” psychometric instrument at the time, the BPRS, did not adequately cover the range of negative symptoms that Opler and his colleagues were observing and wished to measure. Opler was directed to Stanley Kay, who suggested the use of an experimental instrument, the Psychopathology Rating Schedule (PRS), alongside the BPRS.
The PRS was the work of Kay, a psychologist, and Manmohan Singh, an Indian-born, British-trained psychiatrist. While working in a psychopharmacology unit at the Bronx State Hospital, Singh was asked to create, in partnership with Kay, a scale to assess typical and atypical schizophrenia and the efficacy of drug treatments. Drawing from his training and work in Britain, Singh approached his research with the goal of gaining insight into the disease process and embracing a wide range of foci including psychopathology, psychomotor skills, psychosocial cognition, and etiology. The widely available BPRS was designed around the occurrence of symptom changes due to treatment with first-generation antipsychotics. As such, Singh found that the BPRS lacked the means to gauge other dimensions that might be present beyond those known to change in response to first-generation neuroleptics but, per phone interview, Singh does not claim to attribute any of the so-called “negative symptoms” that have been added to the PANSS to any single or group of predecessor scales. Singh and Kay worked to modify and then append the instrument to suit their specific needs.
Opler and Kay determined that many of the items from the PRS addressed negative symptoms, making it complimentary to the 18-item BPRS. The appeal of the PRS also stemmed from the presence of anchoring points ranging from absent (1) to extreme (9) to account for the severity of the symptoms, which improved reliability by defining criteria for each dimension through careful description. Kay and Opler decided to create a single measure that added 12 items from the PRS to the 18 BPRS items. They asserted a fundamentally different premise in the construction of their measure, in that there should be an equivalent number of positive and negative items. The positive subscale included six BPRS items and one PRS item, the negative subscale contained two BPRS items and five items from the PRS. The additional general pathology subscale contained 10 items from the BPRS and six from the PRS. Later joined by Abraham Fiszbein and others, Opler and Kay conducted preliminary studies to test and validate their instrument.28 The three conceptually derived subscales—positive, negative, and general psychopathology—were determined to have high alpha coefficients, indicating that a new instrument with three internally consistent subscales had been born.29
During the era in which the PANSS was developed, the DSM also experienced a transformation. For example, there were debates regarding “mood-congruent” versus “mood-incongruent” delusions and bizarre versus non-bizarre delusions and their relevance for treatment, prognosis, and possible subtyping. As a result, instead of using the “Unusual Thought Content” item from the BPRS for the anchoring point for delusions, Kay and Opler used the “Delusions” item from the PRS so that they could use “Unusual Thought Content” as a separate item to measure bizarreness. These debated subtleties led the way for researchers and clinicians to better interpret and rate psychotic symptoms among inpatient and outpatient populations around the world. To date, the PANSS has become the gold-standard for assessing psychotic symptoms through a semi-structured interview and has been translated into more than 40 different languages.30 While this is currently a widely used and respected assessment, as previously mentioned, it too is a product of its time and context.
Opler’s interest in measuring negative symptoms in the 1980s preceded larger efforts in psychiatry to evaluate new treatments for schizophrenia. Clozapine was recognized to be an “atypical” antipsychotic agent not only for its improved motor side-effect profile but also for its increased efficacy in treating negative symptoms. The success of clozapine as an antipsychotic agent for otherwise treatment-refractory patients spurred a race to develop the next atypical agent. This necessitated a metric to monitor such efforts, thereby cementing the role of the PANSS in psychopharmacological and clinical assessment. Aided by the PANSS, the search for treatments that ameliorate negative symptoms, cognition, and functional impairments of schizophrenia continues as the focus of drug development efforts shifts away from the dopaminergic and toward glutamatergic and other neurotransmitter systems.
Conclusion
Since Moore’s initial efforts and discovery of five highly correlated syndromes, there have been different assessments created to evaluate symptom profiles, target populations, and drug efficacy. All of the scales discussed here strive to appropriately assess an individual’s symptoms and functioning. The advancements in assessments made by the discussed scientists, doctors, clinicians, and researchers discussed above paved the way for the future of understanding symptoms, treatment, and the overall state of knowledge for psychosis. Lorr contributed by stressing the importance of interrater reliability, and acknowledged that the use of scales could both assess the rater’s ability to identify symptoms and assess the patient’s symptoms themselves. Overall and Gorham developed a new scale to better assess the effects of medications on patients. Moore contributed factor analysis to assessing symptoms. These fathers of modern day measurement in psychiatry, like Kraeplin, contributed to our knowledge of the classification of symptoms. Each one of these individuals helped to establish building blocks to the gold-standard assessments used today, and the next generation of assessments will likely build upon these as well. As in the past, future generations of assessment tools will continue to be affected by the predominating philosophies and controversies of their day.
References
- Engel J. American Therapy: The Rise of Psychotherapy in the United States. New York, NY: Penguin Group (USA) Inc.; 2008:43–75.
- Felix RH, Kramer M. Extent of the problem of mental disorders. Ann Am Acad Pol Soc Sci. 1953;286(1):5–14.
- Wittenborn JR, Holzber JD. The generality of psychiatric syndromes. J Consult Psychol. 1951;15(5):372–380.
- Moore TV. The Essential Psychoses and Their Fundamental Syndromes: Studies in Psychology and Psychiatry from the Catholic University of America. Baltimore, MD: Williams and Wilkins; 1933.
- Noll R, DeYoung CG, Kendler KS. Thomas Verner Moore. Am J Psychiatry. 2017;174(8):729–730.
- Lorr M, Jenkins RL, Holsopple JQ. Factors descriptive of chronic schizophrenics selected for the operation of prefrontal lobotomy. J Consult Physchol. 1954;18(4):293–296.
- Lorr M. Rating scales and check lists for the evaluation of psychopathology. Psychol Bull. 1954;51(2):119–127.
- Ban TA. Fifty years chlorpromazine: a historical perspective. Neuropsychiatr Dis Treat.2007;3(4):495–500.
- Lorr M, Rubinstein EA. Factors descriptive of psychiatric outpatients. J Abnorm Psychol. 1955;51(3):514–522.
- Lorr, M, Klett CL, McNair DM, Lasky JJ. Inpatient Multidimensional Psychiatric Scale. Palo Alto, CA: Consulting Psychologists Press; 1962.
- Lorr M, Klett CJ, McNair DM. Syndromes of Psychosis. New York, NY: MacMillan Co.; 1963.
- Guertin WH. A factor-analytic study of schizophrenic symptoms. J Consult Psychol. 1952;16(4):308–312.
- Lorr M, McNair DM, Klett CJ, Lasky JJ. A confirmation of nine postulated psychotic syndromes. Amer Psychologist. 1960;15(7):495.
- Degan JW. Dimensions of Functional Psychosis. Richmond, VA: William Byrd Press.; 1952.
- Eysenck, HJ. The dynamics of anxiety and hysteria: An experimental application of modern learning theory to psychiatry. Oxford, England: Frederick A. Praeger; 1957.
- Lorr, M. Measurement of the major psychotic syndromes. Ann N Y Acad Sci. 1962;93(1): 851–856.
- Grayson DA. Can categorical and dimensional views of psychiatric illness be distinguished?. Br J Psychiatry. 1987;151:355–361.
- Hariri E. Whose evidence? Lessons from the philosophy of science and the epistemology of medicine. Aust N Z J Psychiatry. 2001;35(6): 724–730.
- Gorham DR, Overall JE. Drug-action profiles based on an abbreviated psychiatric rating scale. J Nerv Ment Dis. 1960;131(6):528–535.
- Gorham DR, Overall JE. Dimensions of change in psychiatric symptomatology. Dis Nerv Syst. 1961;22:576–580.
- Hedlund JL, Vieweg BW. The Brief Psychiatric Rating Scale (BPRS): a comprehensive review. J Oper Psychiatry. 1980;11(1):48–65.
- Overall JE, Gorham DR. The brief psychiatric rating scale. Psychol Rep. 1962;10(3):799–812.
- Overall JE, Gorham DR. The Brief Psychiatric Rating Scale (BPRS): recent developments in ascertainment and scaling. Psychopharmacol Bull. 1988; 24(1):97–99.
- Rhoades HM, Overall JE. The semistructured BPRS interview and rating guide. Psychopharmacol Bull. 1988;24(1):101–104.
- Crow TJ. Regular review: molecular pathology of schizophrenia: more than one disease process?. 1980;280(6207):66–68.
- Crow TJ. Positive and negative schizophrenic symptoms and the role of dopamine. Br J Psychiatry. 1980;137:383–386.
- Angrist B, Rotrosen J, Gershon S. Differential effects of amphetamine and neuroleptics on negative vs. positive symptoms in schizophrenia. 1980;72(1):17–19.
- Opler LA, Kay SR, Rosado V, Lindenmayer JP. Positive and negative syndromes in chronic schizophrenic inpatients. J Nerv Ment Dis. 1984;172(6):317–325.
- Kay SR, Fiszbein A, Opler LA. The positive and negative syndrome scale (PANSS) for schizophrenia. Schizophr Bull. 1987;13(2): 261–276.
- Khan A, Yavorsky C, Liechti S, et al.. A rasch model to test the cross-cultural validity in the positive and negative syndrome scale (PANSS) across six geo-cultural groups. BMC Psychol. 2013;1(1):5.
