by Cheryl B. McCullumsmith, MD, PhD; David J. Williamson, PhD; Roberta S. May, MA; Emily H. Bruer, M.ed; David V. Sheehan, MD, MBA; and Larry D. Alphs, MD, PhD
by Cheryl B. McCullumsmith, MD, PhD; David J. Williamson, PhD; Roberta S. May, MA; Emily H. Bruer, M.ed; David V. Sheehan, MD, MBA; and Larry D. Alphs, MD, PhD
Dr. McCullumsmith is with the University of Cincinnati Department of Psychiatry and Behavioral Neuroscience, Cincinnati, Ohio; Dr. Williamson is with the University of South Alabama College of Medicine, Departments of Psychiatry and Neurology, Birmingham, Alabama, and Janssen Medical Affairs, LLC, Titusville, New Jersey; Ms. May is with the University of Alabama, Birmingham, Alabama; Ms Bruer is with the University of Alabama, Department of Psychiatry and Behavioral Neurobiology, Birmingham, Alabama; Dr. Sheehan is Distinguished University Health Professor Emeritus, University of South Florida College of Medicine, Tampa, Florida; and Dr. Alphs is with Janssen Medical Affairs, LLC, Titusville, New Jersey.
Innov Clin Neurosci. 2014;11(9–10):47–53
Funding: Janssen supported UAB for data collection and training associated with this project, but there was no funding to authors or anyone else for the writing of the manuscript.
Financial Disclosures: Dr. McCullumsmith has no conflicts of interest relevant to the content of this article; Dr. Williamson is an employee and stockholder in Johnson and Johnson, Janssen Scientific Affairs’s parent company; Ms. May has no conflicts of interest relevant to the content of this article; Ms. Bruer has no conflicts of interest relevant to the content of this article; Dr. Sheehan is the author and copyright holder of the Sheehan-Suicide Tracking Scale (S-STS), the Sheehan-Suicidality Tracking Scale Clinically Meaningful Change Measure Version (S-STS CMCM), the Pediatric versions of the S-STS, the Sheehan Disability Scale (SDS), and the Suicidality Modifiers Scale, is a co-author of the Suicide Plan Tracking Scale (SPTS), and owns stock in Medical Outcomes Systems, which has computerized the S-STS; Dr. Alphs is employed by Janssen Scientific Affairs, Titusville, New Jersey, and is a stockholder of Johnson & Johnson.
Key Words: Suicidality, assessment
Abstract: Objective: To explore the authors’ predictions 1) that hopelessness would positively correlate with suicidal ideation and that impulsivity (either transient urges to self-harm or impulsive acting out) would positively correlate with suicidal behavior, and 2) that the recent or long-standing nature of the traits will have corresponding effects on reported histories of suicidal ideation and behavior. Design: Questionnaire validation trial in which each subject received every measure in counterbalanced fashion. Setting: Inpatient and outpatient psychiatric settings associated with a medium-sized medical school in the southeastern United States. Participants: Forty-five subjects presenting with varying levels of suicidal ideation and behavior completed measures providing information about their histories of suicidal ideation and behavior, recent feelings of hopelessness, feelings of general hopelessness, recent feelings of difficulty controlling urges to self-harm, and feeling about general levels of impulsivity. Measurements: The InterSePT Scale for Suicidal Thinking–Plus, the Sheehan-Suicidality Tracking Scale, the Columbia–Suicide Severity Rating Scale, and six additional questions to assess hopelessness and impulsivity. Results: Recent and trait hopelessness correlated positively with suicidal ideation. Patients who reported any suicide attempt endorsed higher levels of general impulsivity than those who did not report a history of at least one suicide attempt. Those enrolled in the study secondary to a very recent suicide attempt reported more difficulties with recent suicidal impulses. Conclusion: Simple measures of hopelessness and impulsivity are associated with suicidal ideation and attempts and may add to determination of suicide risk.
Introduction
While death by suicide is now the 10th leading cause of death in the United States overall,[1] prediction of those most at risk for death by suicide or suicide attempts remains difficult. Existing scales to assess suicidal ideation or risk of suicide largely focus on quantifying and describing suicidal thoughts and intentions.[2–4] While suicidal ideation is very common in those with a history of suicide attempts, most patients with suicidal ideation never make a suicide attempt or die by suicide.[5–7] Prediction of future suicidal behavior among those individuals with suicidal ideation or among those who never report suicidal ideation may require the consideration of other risk factors, ideally ones that could be altered with therapy or medication.
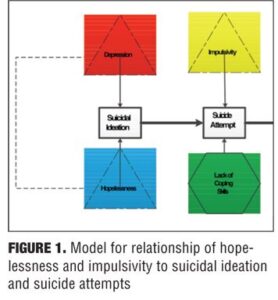
Two independent factors significantly associated with suicidal behavior are hopelessness and impulsivity.[8–29] Hopelessness has been independently and repeatedly associated with increased risk for suicidal ideation, suicide attempts, and death by suicide, both prospectively and retrospectively.[8–19] Impulsivity has been strongly associated with risk of suicide attempts and death by suicide, with few papers linking impulsivity to increased suicidal ideation.[20–29] From a review of this extensive literature, we have developed a simple model of progression from suicidal ideation to suicide attempt where hopelessness increases suicidal ideation, and impulsivity increases risk for suicide attempt (Figure 1).
However, some studies have not found association of hopelessness and/or impulsivity with suicide attempts or behavior.[4,18,30] A potential source of variability in these findings is the manner in which the constructs of hopelessness and impulsivity are measured. Different scales used to assess hopelessness and impulsivity may well be measuring entirely different dimensions or constructs. Longer scales like the Beck Hopelessness Scale10 or Barratt Impulsivity Scale31 may be more comprehensive, while shorter scales may address only a few or even one aspect of hopelessness or impulsivity. An additional important point of variance between existing scales is time frame: that is, does the scale attempt to measure recent and/or transient mood states (that may reflect attacks of impulsive suicidality) or more stable personality traits? Some preliminary studies suggest that the stability of hopelessness and impulsivity could be critical.[17,32–37] For instance, patients who are hopeless only while depressed are not as likely to harm themselves in the future as those who are hopeless when not depressed.[17] Similarly, while individuals who are prone to acting out impulsively in general are more likely to exhibit suicidal behavior generally, the addition of factors that transiently increase impulsivity (such as cocaine or alcohol) may add significant immediate risk.[32–37]
Combining our simple model of A) the relationship of hopelessness and impulsivity to suicidal behavior and B) our consideration of the differential effects of stable and recent (e.g., within the past 7 days) effects of hopelessness and impulsivity, we made a number of specific hypotheses with regard to the relationships of hopelessness and impulsivity to suicidal ideation and behavior (SIB), as follows:
1. Trait hopelessness will be positively associated with current suicidal ideation.
2. Recent hopelessness will be positively associated with current suicidal ideation.
3. Patients reporting a history of suicide attempts will have higher trait impulsivity than those who do not report suicide attempts.
4. Patients with recent suicidal behavior will report higher levels of recent impulsivity reflecting attacks of impulsive suicidality than those without recent suicidal behavior.
We examined these hypotheses within the context of an experimental sample assembled to assess correspondence between three previously validated scales of SIB. As part of this study, we included a smaller pilot questionnaire designed to assess the extent to which recent and trait hopelessness and impulsivity might influence the results of these scales. This paper focuses on how the hopelessness- and impulsivity-related questions from this pilot questionnaire were associated with patient history of SIB and current SIB.
Methods
Participants. A convenience sample of 45 subjects with varying severity of SIB were recruited from inpatient and outpatient psychiatric settings associated with the University of Alabama at Birmingham (UAB), a medium-sized medical school in the southeastern United States. We sought a minimum of five subjects from each of eight levels of SIB severity (described in “Measures” below). The Institutional Review Board of UAB approved the study, and each subject gave written informed consent.
Measures. This study was conducted within the context of a comparison of the InterSePT Scale for Suicidal Thinking–Plus (ISST–Plus),[38] the Sheehan-Suicidality Tracking Scale (S-STS),[39] and the Columbia–Suicide Severity Rating Scale (C–SSRS).[2] This comparison sought to determine the extent to which these scales could be used to map to the United States Food and Drug Administration’s (FDA) Classification Algorithm for Suicide Assessment (CASA).[40] A complete description of the methodology used for this comparison is being prepared in another report.[41] The data in this paper includes the computerized 11/11/11 versions of the S-STS, the Suicidality Modifiers (SM) scale (used in University of Alabama Birmingham S-STS validation study[42]), and the Alphs Dichotomous Impulsivity and Hopelessness (IH) (2 questions) from the ISST-Plus (used in the University of Alabama Birmingham ISST-Plus Validation Study). The S-STS is a well-validated instrument to assess SIB.[39,41,43] The S-STS obtains parallel scores from the patient as well as from the clinician, the latter based on structured clinical interview.
We were unable to collect S-STS patient ratings from subjects who presented with accidental injuries, as these all involved upper extremity injuries that precluded their ability to respond using the instrument’s computer interface. Consequently, we used the “Suicidal ideation” score from the clinician-rated S-STS as our metric for current suicidal ideation, as this provided us data across the entire range of suicidal ideation presenting in our sample. Higher scores indicated more intense suicidal ideation.
Patients also responded to questions regarding their feelings of hopelessness and impulsivity. “Stable” questions were framed in the context of “day-to-day life,” whereas “recent” were framed within the context of the past seven days. The questions were as follows:
1. Recent hopelessness (rated on a 5-point scale from “Not at all” [0] to “Extremely” [5]): 1) How much did you lose hope that your life would get better? and 2) How difficult was it for you to be hopeful that your life would get better?
2. Trait hopelessness (rated on a 7-point scale ranging from “Extremely hopeless” [0] to “Extremely hopeful” [7]): How hopeful/hopeless are you in your day-to-day life?
3. Recent impulsivity reflecting attacks of impulsive suicidality (same 5-point scale as the “Recent hopelessness” items): 1) How strong was the impulse (urgent need) to plan or to act in any suicidal way? and 2) How difficult was it for you to suppress or to restrain the impulse to plan or to act in any suicidal way?
4. Trait impulsivity (rated on a 7-point scale ranging from “Extremely cautious” [0] to “Extremely impulsive [7]): How impulsive/cautious are you in your day-to-day life?
As with the S-STS, responses to these questions were provided directly by patients via computer interface or to a clinician within an interview format. In the latter context, the clinician provided the rating felt to be the most accurate. For the “recent” items, we used the sum of the ratings for the two questions for each of the two domains (hopelessness and impulsivity).
Raters. Five raters were trained to administer all three scales and the pilot scale. Three of the five raters were master’s level counselors and two had Bachelor of Science degrees with extensive clinical research experience. Each was selected to administer a scale to a given subject on an “as available” basis. The raters participating in this study were qualified mental health professionals with experience working with suicidal patients. They were trained and certified using the training materials developed for each assessment scale. These included use of semi-structured interviews developed for each of the three SIB assessment instruments (C-SSRS, ISST-Plus, and S-STS). Similar standardized definitions of all critical SIB terms were used for all three scales. The authors of the respective instruments supervised the training the training for each scale.
Statistical analysis. All analyses were performed using Stata 13.1 (StataCorp, 2013 Stata: Release 13. Statistical Software. College Station, Texas: StataCorp LP). Baseline demographics and clinical characteristics were evaluated using descriptive statistics. Our first two hypotheses addressed the strength of the correlation between continuous variables: these were tested comparing the respective Spearman’s rhos using Hotelling’s t. Our second two hypotheses involved group differences: these were examined with traditional t-tests.
Results
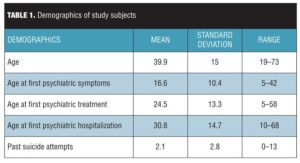
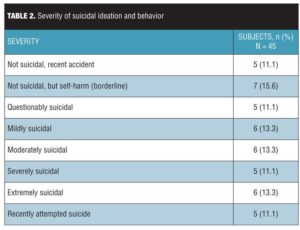
Study subjects. Demographics are summarized in Table 1. Most subjects were female (55.6%); 73.3 percent were white, 24.4 percent were black, and 2.2 percent were of mixed race. The number of subjects at each level of SIB severity is depicted in Table 2.
Although only five out of 45 of our subjects had recently attempted suicide, the majority of the patients with suicidal ideation had attempted suicide in the past. In fact, of the 34 subjects reporting suicidal ideation who had not made a recent attempt, 25 of these subjects (74%) had a history of at least one previous suicide attempt.
Primary hypotheses. Hopelessness. Results of analyses of the relationships between hopelessness and suicidal ideation were consistent with hypotheses. Trait hopelessness correlated positively with the S-STS suicidal ideation score (p=0.607, p<0.0001). Similarly, hopelessness over the past seven days correlated positively with the S-STS suicidal ideation score (p=0.751, p<0.0001).
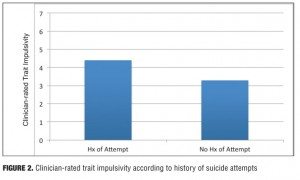
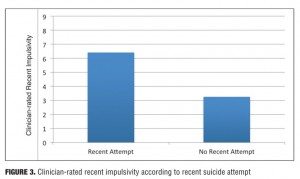
Impulsivity. Results of analyses of the relationships between impulsivity and suicidal behavior were also consistent with hypotheses. As predicted, patients who reported any historical suicide attempt were rated as reporting higher trait impulsivity than those who did not, as depicted in Figure 2 (mean [M]=4.400, standard deviation [SD]=1.694 vs. M=3.267, SD=1.033, respectively; t(43)= -2.372, p<0.05). Similarly, those who were enrolled in the study secondary to a very recent suicide attempt (M=6.400, SD=2.191) were rated as reporting higher levels of recent impulsivity than those who had not recently attempted suicide, as depicted in Figure 3 (M=3.250, SD=2.933, t(43)= -2.312, p<0.05).
Discussion
Our sample, chosen specifically to provide a range of suicidal ideation, allowed us to examine some of the relationships hypothesized in our model of SIB. Consistent with our model, we found that higher levels of both recent and trait hopelessness are linked to more severe suicidal ideation. Similarly, higher trait impulsivity is reported by those with any historical suicide attempt, whereas higher recent impulsivity is reported by those with a recent history of suicide attempt. It is striking that these effects were evident statistically even with our relatively limited numbers of subjects and items.
These findings corroborate evidence establishing strong associations between hopelessness and suicidal ideation and between impulsivity and suicidal behavior.[21,25,44] Moreover, our study suggests that simple questions to establish stable and recent hopelessness and impulsivity can demonstrate strong associations with SIB and may prove very useful in clinical settings where time and patient tolerance for extended interviews are limited.
This study suggests the importance of the delineation of recent feelings of hopelessness and impulsivity compared to chronic or state feelings of hopelessness and impulsivity in determining acute suicidal risk. Many studies of impulsivity have used the Barratt Impulsivity Scale, which is a measure of trait (stable) impulsivity. Few studies have measured recent impulsivity that may reflect attacks of impulsive suicidality in suicide attempts and death. However, increasing recent impulsivity factors have been considered as likely etiologies of the high correlation of alcohol substance use and suicide. One theory of the strong correlation of cocaine and alcohol use to suicide is via their ability to transiently increase impulsivity.[45–48] Others have examined the role of higher trait impulsivity in suicide, which may explain the link between Cluster B personality disorders and suicide as well as the strong hereditability of suicidal behavior.[19,21,28,49–55] However, no standard scales assess acute impulsivity and no scales delineate clearly between trait (stable) hopelessness and new-onset hopelessness.
A few limitations to our question wording warrant consideration. One might question the utility of the distinction between patient-reported “trait” vs. “recent” hopelessness and impulsivity, as numerous reports indicate that the recall of constructs is driven strongly by the congruence of what is being recalled with the mood of the patient at the time that he or she is asked.[56] While this point of view is reasonable, questions such as those examined in this study represent typical time frames often discussed by patients and clinicians in critical emergency department encounters. Consequently, although retrospective estimates of both “recent” and “typical” feelings are certainly colored by in-the-moment mood, it is important to examine the relationship of the responses to these types of questions to parameters that we know to be important in the clinician’s judgment of risk for future suicidal behavior (e.g., previous suicide attempts) to see if, in fact, the questions yield information that behaves identically or, in fact, diverges in ways that may be clinically important. Another aspect of these findings that merits further exploration is that the impulsivity items behaved as hypothesized, despite their disparate nature. Specifically, the “recent” items could be construed as asking more about attacks of impulsive suicidality, whereas the “trait” item was open enough to include the more act-without-thought type of impulsive personality trait. We look forward to a replication elaborating upon this work in which a two-by-two matrix can tease apart the extent to which time scale may play a relevant role in altering the relationship between suicidal behavior and different types of impulsive behavior described.
Limitations. A limitation of our study is the higher prevalence of SIB in our sample. We deliberately recruited our sample from clinical settings to represent a range of severity of suicidal ideation; consequently, the rate of suicidal ideation was quite high relative to the general population. However, our rate of reported suicidal behavior, (specifically suicide attempts) was quite high, particularly among those with current suicidal ideation (74%), The large proportion of individuals with prior attempts among those with current suicidal ideation may reflect the acuity of presentation and baseline risk for patients presenting to the emergency department with suicidal ideation overall. Similar findings of high rates of historical suicide attempts in those with current suicidal ideation have been reported in other high risk populations.[36,57–59]
Clearly more work remains to be done. Although the range of patients from across a broad, prospectively defined range of severity of suicidal ideation is a strength of the study, the absolute number of patients available to us that had recently attempted suicide was quite small: it will be important to replicate these findings in a larger sample of such patients. Likewise, this study was only able to examine a portion of the hypothesized model. Future efforts will be needed to assess the extent to which depression modifies the role that hopelessness plays in fostering suicidal ideation and the manner in which a lack of coping skills may interact with impulsivity in spurring suicidal behavior.
References
1. United States Centers for Disease Control and Prevention. Twenty Leading Causes of Death Among Persons Ages 10 Years and Older, United States, 2009. Web-based Injury Statistics Query and Reporting System (WISQARS). Leading Causes of Death Reports. Atlanta, GA: National Center for Injury Prevention and Control. http://www.cdc.gov/injury/wisqars/index.html. Accessed October 1, 2014.
2. Posner K, Brown GK, Stanley B,
et al. The Columbia–Suicide Severity Rating Scale: initial validity and internal consistency findings from three multisite studies with adolescents and adults. Am J Psychiatry. 2011;168:1266–1277.
3. Beck AT, Kovacs M, Weissman A. Assessment of suicidal intention: the Scale for Suicide Ideation. J Consult Clin Psychol. 1979;47:343–352.
4. Stefansson J, Nordström P, Jokinen J. Suicide Intent Scale in the prediction of suicide. J Affect Disord. 2012;136:167–171.
5. Borges G, Angst J, Nock MK,
et al. A risk index for 12-month suicide attempts in the National Comorbidity Survey Replication (NCS-R). Psychol Med. 2006;36:1747–1757.
6. Borges G, Angst J, Nock MK, et al. Risk factors for the incidence and persistence of suicide-related outcomes: a 10-year follow-up study using the National Comorbidity Surveys. J Affect Disord. 2008;105:25–33.
7. Kessler RC, Chiu WT, Demler O,
et al. Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry. 2005;62:617–627.
8. Weissman A, Beck A, Kovacs M. Drug abuse, hopelessness, and suicidal behavior. Int J Addict. 1979;14:451–464.
9. Emery G, Steer R, Beck A. Depression, hopelessness, and suicidal intent among heroin addicts. Int J Addict. 1981;16:425–429.
10. Beck AT, Steer RA, Kovacs M,
et al. Hopelessness and eventual suicide: a 10-year prospective study of patients hospitalized with suicidal ideation. Am J Psychiatry. 1985;142:559–563.
11. Chochinov HM, Wilson KG, Enns M, et al. Depression, Hopelessness, and suicidal ideation in the terminally ill. Psychosomatics. 1998;39:366–370.
12. Hewitt P, Norton G, Flett G, et al. Dimensions of perfectionism, hopelessness, and attempted suicide in a sample of alcoholics. Suicide Life Threat Behav. 1998;28:395–406.
13. Borges G, Saltijeral MT, Bimbela A, et al. Suicide attempts in a sample of patients from a general hospital. Arch Med Res. 2000;31:366–372.
14. Papakostas GI, Petersen T, Pava J, et al. Hopelessness and suicidal ideation in outpatients with treatment-resistant depression: prevalence and impact on treatment outcome. J Nerv Ment Dis. 2003;191:444–449.
15. Fawcett J, Scheftner WA, Fogg L, et al. Time-related predictors of suicide in major affective disorder. Am J Psychiatry. 1990;147:1189–1194.
16. Fawcett J, Scheftner W, Clark D,
et al. Clinical predictors of suicide in patients with major affective disorders: a controlled prospective study. Am J Psychiatry. 1987;144:35–40.
17. Young MA, Fogg LF, Scheftner W, et al. Stable trait components of hopelessness: baseline and sensitivity to depression. J Abnorm Psychol. 1996;105:155–165.
18. Samuelsson M, Jokinen J, Nordström AL, et al. CSF 5-HIAA, suicide intent and hopelessness in the prediction of early suicide in male high-risk suicide attempters. Acta Psychiatr Scand. 2006;113:44–47.
19. Brezo J, Paris J, Turecki G. Personality traits as correlates of suicidal ideation, suicide attempts, and suicide completions: a systematic review. Acta Psychiatr Scand. 2006;113:180–206.
20. Oquendo MA, Mann JJ. The biology of impulsivity and suicidality. Psychiatr Clin North Am. 2000;23:11–25.
21. Baca-Garcia E, Diaz-Sastre C, Garcia Resa E, et al. Suicide attempts and impulsivity. Eur Arch Psychiatry Clin Neurosci. 2005;255:152–156.
22. Braquehais MD, Oquendo MA, Baca-García E, et al. Is impulsivity a link between childhood abuse and suicide? Compr Psychiatry. 2010;51:121–129.
23. Brodsky B, Oquendo M, Ellis S,
et al. The relationship of childhood abuse to impulsivity and suicidal behavior in adults with major depression. Am J Psychiatry. 2001;158:1871–1877.
24. Carballo J, Oquendo M, Giner L, et al. Impulsive-aggressive traits and suicidal adolescents and young adults with alcoholism. Int J Adolesc Med Health. 2006;18:15–19.
25. Oquendo MA, Galfalvy H, Russo S, et al. Prospective study of clinical predictors of suicidal acts after a major depressive episode in patients with major depressive disorder or bipolar disorder. Am J Psychiatry. 2004;161:1433–1441.
26. Sher L, Oquendo MA, Galfalvy HC, et al. The relationship of aggression to suicidal behavior in depressed patients with a history of alcoholism. Addict Behav. 2005;30:1144–1153.
27. Kasen S, Cohen P, Chen H. Developmental course of impulsivity and capability from
age 10 to age 25 as related to trajectory of suicide attempt
in a community cohort. Suicide Life Threat Behav. 2011;41:180–192.
28. Dumais A, Lesage A, Alda M, et al. Risk factors for suicide completion in major depression: a case-control study of impulsive and aggressive behaviors in men. Am J Psychiatry. 2005;162:2116–2124.
29. Zouk H, Tousignant M, Seguin M, et al. Characterization of impulsivity in suicide completers: clinical, behavioral and psychosocial dimensions. J Affect Disord. 2006;92:195–204.
30. Gladstone GL, Mitchell PB,
Parker G, et al. Indicators of suicide over 10 years in a specialist mood disorders unit sample. J Clin Psychiatry. 2001;62:945–951.
31. Patton JH, Stanford MS, Barratt ES. Factor structure of the Barratt impulsiveness scale. J Clin Psychol. 1995;51:768–774.
32. Amore M, Innamorati M, Vittorio CD, et al. Suicide attempts in major depressed patients with personality disorder. Suicide Life Threat Behav. 2014 Apr;44(2):155–166.
33. Bernal M, Haro JM, Bernert S,
et al. Risk factors for suicidality in Europe: results from the ESEMED study. J Affect Disord. 2007;101:27–34.
34. Sublette EM, Carballo JJ, Moreno C, et al. Substance use disorders and suicide attempts in bipolar subtypes. J Psychiatr Res. 2009;43:230–238.
35. Garlow SJ, Purselle DC, Heninger M. Cocaine and alcohol use preceding suicide in African American and white adolescents. J Psychiatr
Res. 2007;41:530–536.
36. McCullumsmith CB, Clark CB, Perkins A, et al. Gender and racial differences for suicide attempters and ideators in a high-risk community corrections population. Crisis. 2013;34(1):50–62.
37. Oquendo MA, Currier D, Liu SM,
et al. Increased risk for suicidal behavior in comorbid bipolar disorder and alcohol use disorders: results from the National Epidemiologic Survey on Alcohol and Related Conditions (NESARC). J Clin Psychiatry. 2010;71:902–909,
38. Lindenmayer JP, Czobor P, Alphs L, et al. The InterSePT scale for suicidal thinking reliability and validity. Schizophr Res. 2003;63:161-70.
39. Coric V, Stock EG, Pultz J, et al. Sheehan-Suicidality Tracking Scale (S-STS): preliminary Results from a multicenter clinical trial in generalized anxiety disorder. Psychiatry (Edgmont). 2009;6:26–31.
40. Posner K, Oquendo MA, Gould M, et al. Columbia–Classification Algorithm of Suicide Assessment (C–CASA): classification of suicidal events in the FDA’s pediatric suicidal risk analysis of antidepressants. Am J Psychiatry. 2007;164:1035–1043.
41. Sheehan D, Giddens J, Sheehan I. Status Update on the Sheehan-Suicidality Tracking Scale (S-STS). Innov Clin Neurosci. 2014;11(9–10):93–140.
42. Sheehan DV, Alphs L, Giddens JM. Comparative validation of the ISST-Plus, the S-STS and the C-SSRS for assessing suicidal thinking and behavior. Poster presented at the 14th International Congress on Schizophrenia Research (ICOSR). Orlando, FL: April 21–25, 2013.
43. Preti A, Sheehan DV, Coric V,
et al. Sheehan-Suicidality Tracking Scale (S-STS): reliability, convergent and discriminative validity in young Italian adults. Compr Psychiatry. 2013;54(7):842–849.
44. Beck AT, Brown G, Steer RA. Prediction of eventual suicide in psychiatric inpatients by clinical ratings of hopelessness. J Consult Clin Psychol. 1989;57:309–310.
45. Roy A, Gonzalez B, Marcus A,
et al. Serum cholesterol, suicidal behavior and impulsivity in cocaine-dependent patients. Psychiatry Res. 2001;101:243–247.
46. Roy A. Relationship of childhood trauma to age of first suicide attempt and number of attempts in substance dependent patients. Acta Psychiatr Scand. 2004;109:121–125.
47. Sher L. Alcoholism and suicidal behavior: a clinical overview. Acta Psychiatr Scand. 2006;113:13–22.
48. Chachamovich E, Ding Y, Turecki G. Levels of aggressiveness are higher among alcohol-related suicides: results from a psychological autopsy study. Alcohol. 2012;46:529–536.
49. Abreu LN, Lafer B, Baca-Garcia E, et al. Suicidal ideation and suicide attempts in bipolar disorder type I: an update for the clinician. Rev Bras Psiquiatr. 2009;31:271–280,
50. Roy A. Family history of suicide and impulsivity. Arch Suicide Res. 2006;10:347–352.
51. McGirr A, Paris J, Lesage A, et al. Risk factors for suicide completion in borderline personality disorder: a case-control study of cluster B comorbidity and impulsive aggression. J Clin Psychiatry. 2007;68:721–729.
52. Peluso MAM, Hatch JP, Glahn DC, et al. Trait impulsivity in patients with mood disorders. J Affect Disord. 2007;100:227–231.
53. Swann A, Lijffijt M, Lane S, et al.: Increased trait-like impulsivity and course of illness in bipolar disorder. Bipolar Disord. 2009;11:280–288.
54. Doihara C, Kawanishi C, Ohyama N, et al. Trait impulsivity in suicide attempters: preliminary study. Psychiatry Clin Neurosci. 2012;66:529–532.
55. Westheide J, Quednow BB, Kuhn KU, et al. Executive performance of depressed suicide attempters: the role of suicidal ideation. Eur Arch Psychiatry Clin Neurosci. 20008;258:414–421.
56. Bremner JD, Shobe KK, Kihlstrom JF. False memories in women with self-reported childhood sexual abuse: an empirical study. Psychol Sci. 2000;11:333-337.
57. Ilgen MA, Zivin K, McCammon RJ, et al. Pain and suicidal thoughts, plans and attempts in the United States. Gen Hosp Psychiatry. 2008;30:521–527.
58. Ilgen MA, Burnette ML, Conner KR, et al. The association between violence and lifetime suicidal thoughts and behaviors in individuals treated for substance use disorders. Addict Behav.
2010;35(2):111–115.
59. Wojnar M, Ilgen M, Czyz E, et al. Impulsive and non-impulsive suicide attempts in patients treated for alcohol dependence. J Affect Disord. 2009;115:131–139.