 by Allison Cowan, MD and Ali Ashai, MD
by Allison Cowan, MD and Ali Ashai, MD
Drs. Cowan and Ashai are with the Department of Psychiatry at the Boonshoft School of Medicine at Wright State University in Dayton, Ohio.
FUNDING: No funding was provided.
DISCLOSURES: The authors have no conflicts of interest relevant to the content of this article.
ABSTRACT: Sexual assault and abuse can result in severe physical and emotional trauma to the victim. Deploying targeted psychotherapeutic treatment that is individualized for the survivor is important to achieving optimal patient outcomes. There are several valid and evidence-based treatments available for posttraumatic stress disorder (PTSD) and interpersonal difficulties that can result from sexual abuse and assault. In this article, the authors discuss psychodynamic psychotherapy, trauma-focused cognitive behavioral therapy (TF-CBT), and eye movement desensitization and reprocessing therapy (EMDR) for the treatment of patients following sexual assault and abuse. The authors also provide practice points on common issues in the management of the treatment of sexual assault survivors, including transference, countertransference, and avoiding retraumatization. Composite case vignettes are used to illustrate treatment techniques.
KEYWORDS: Sexual abuse, sexual trauma, transference, countertransference, trauma
Department Editor. Julie P. Gentile, MD, is a professor with and chair of the Department of Psychiatry at Wright State University in Dayton, Ohio.
Editor’s Note. The patient cases presented in Psychotherapy Rounds are composite cases written to illustrate certain diagnostic characteristics and to instruct on treatment techniques. The composite cases are not real patients in treatment. Any resemblance to a real patient is purely coincidental.
Innov Clin Neurosci. 2020;17(22–26):
The intersection of sexual assault and psychotherapy is complicated. It was not until relatively recently that the treatment of survivors of sexual assault came to be under the purview of psychotherapeutic treatment.1 In their 1974 American Journal of Psychiatry article, Burgess and Holmstrom reported that there was little information on the physical and psychological effects of rape or how to manage the treatment of a survivor of sexual assault in the psychiatric literature.1 In the past, rape survivors were thought to need only counseling—that is, direct, problem-focused treatment—rather than broader, more in-depth treatment such as psychotherapy and, if the survivor did undergo psychotherapy, the major focus was on preexisting psychopathology.2 The United States Centers for Disease Control and Prevention (CDC) estimates that sexual violence affects one in three women and one in four men over the course of their lifetimes.3 The treatment of survivors of sexual assault gains benefits from several general and specialized types of psychotherapy including psychodynamic psychotherapy, trauma-focused cognitive–behavioral therapy (TF-CBT), and eye movement desensitization and reprocessing therapy (EMDR). In this article, we review these psychotherapeutic treatment methods in regard to managing this patient population and provide additional treatment suggestions to assist therapists in achieving optimal outcomes among survivors of sexual assault and abuse.
Psychodynamic Psychotherapy
Psychodynamic psychotherapy has been shown to be effective in treating patients with posttraumatic stress disorder (PTSD) that might have resulted from sexual assault.4,5 Gabbard previously described the distinctive features of psychodynamic psychotherapy (Table 1).6
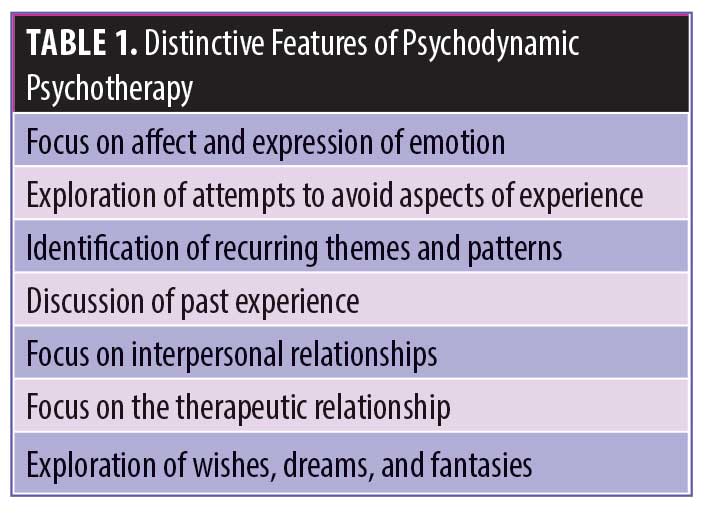
When treating a patient who has been sexually abused or assaulted, these distinctive features of psychodynamic psychotherapy remain the focus of the treatment. “Follow the red thread” is a phrasing used to encourage the therapist to focus on the feelings and emotions occurring in the therapy session rather than be pulled into discussing superficial issues. In order to do this, the therapist must create a safe space for talking with the patient by being empathic and nonjudgmental, attending to the patient’s physical comfort, and demonstrating understanding.7 Without these elements, a patient might feel retraumatized and unsafe.
Composite case vignette 1. Ms. A is a 28-year-old woman who has survived multiple instances of sexual abuse and sexual assault from men of authority in her life. She initiated therapy with the goal of improving her comfort in and ability to maintain an intimate relationship.
Dr. B—Last week, we talked about your date that you had planned for this past weekend. How did it go?
Ms. A—It went well! He was handsome and charming. We went to the boardwalk, played games, and he put his arm around me and kissed me.
Dr. B.—How did that feel?
Ms. A.—It felt good, I wanted him to… Also, we had sex.
Dr. B.—Oh, okay. How do you feel about that?
Ms. A.—Well, I know I said last week I wasn’t going to on the first date, but I wanted to. But, then, he was just a great guy, and guys always want to have sex. A date is always better with sex for them and, so, if we have sex, he’s going to like the date more.
Dr. B.—Would you have enjoyed the date more if you didn’t have sex?
Ms. A.—Hmm. I don’t know.
Dr. B.—Hmm.
Ms. A.—You think I only slept with him so that he’d like me.
Dr. B.—I’m sorry if my words or tone suggested judgment. That wasn’t my intention. I’m trying to understand what your feelings are. You’ve told me that you wanted to have sex with him and that you’d planned not to. So, I’m just trying to reconcile these ideas and better understand what your feelings are on this issue.
Ms. A.—Well, I guess, if I’m being honest, all men want sex. So…yeah, if you want a man to like you, give him sex. It’s what they want. Like, even my high school English teacher. I thought he wanted to help my writing, but no. What he wanted was sex.
Dr. B.—[allows for pause] That must have been difficult. How old were you then?
Ms. A.—Junior year…I was 16 when it happened, I guess.
Dr. B.—What happened?
Ms. A.—He had sex with me.
Dr. B.—[pauses]
Ms. A.—I was really into writing poetry, and I would sometimes stay after school to show him what I had written. I thought maybe he could help me get published somewhere. I would workshop with him. One day he decided to put his hand on my thigh and, I guess, see what would happen. I remember I just froze. [starts tearing up] I didn’t stop him, so I guess he thought that was a green light.
Dr. B.—How did you feel in that moment?
Ms. A.—Sad. [crying] Sad and just so angry.
Dr. B.—Tell me about the anger.
Ms. A.—Because, why does this always keep happening to me? Did I do something to make him think this was okay? I mean, clearly, I must be doing something for this to keep happening.
Dr. B.—Is that what you were thinking in that moment?
Ms. A.—Yeah, definitely. I still think about that sometimes though. Like, I know it’s not my fault, but still I just wonder why I froze instead of doing something.
Dr. B.—How are you feeling right now?
Ms. A.—Sad and mad.
Dr. B.—Yes, it seemed like it was difficult to share that information, but thank you for telling me. I hope that talking about it here will help you feel better.
This vignette also demonstrates exploration of recurring themes and patterns, sometimes of self-recrimination, betrayal, or anger, which can be drawn together to illustrate common patterns in a patient’s life in psychodynamic psychotherapy. The therapist in the vignette takes care to ask curious questions and make empathic statements that allow the patient to continue talking. Survivors can feel complicated mixes of emotions when discussing sexual assault. They might remember the feeling of having special, secret attention from someone in a powerful position. They might feel the horror and pain of the assault. They might recall the sting of betrayal because loved ones or caregivers were not able to protect them from harm. Survivors might feel guilt over what they think they should have or could have done differently. These powerful mixtures of emotions should not be shied away from but, rather, they should be held up for examination and consideration.
Practice points for psychodynamic psychotherapy.
- The feelings resulting from sexual abuse or sexual assault can be complicated, intense, and unclear.
- A nonjudgmental exploration of recurring themes and patterns can be helpful in clarifying feelings and actions.
- Discussion of past experience is a cornerstone not only of psychodynamic psychotherapy but of the treatment of sexual trauma.
Trauma-focused Cognitive–behavioral Therapy
TF-CBT is a brief, resilience-building model for trauma-impacted children or adolescents and their parents and caregivers that adapts the tenets of CBT for healing from trauma.8 The components are presented in Table 2.9
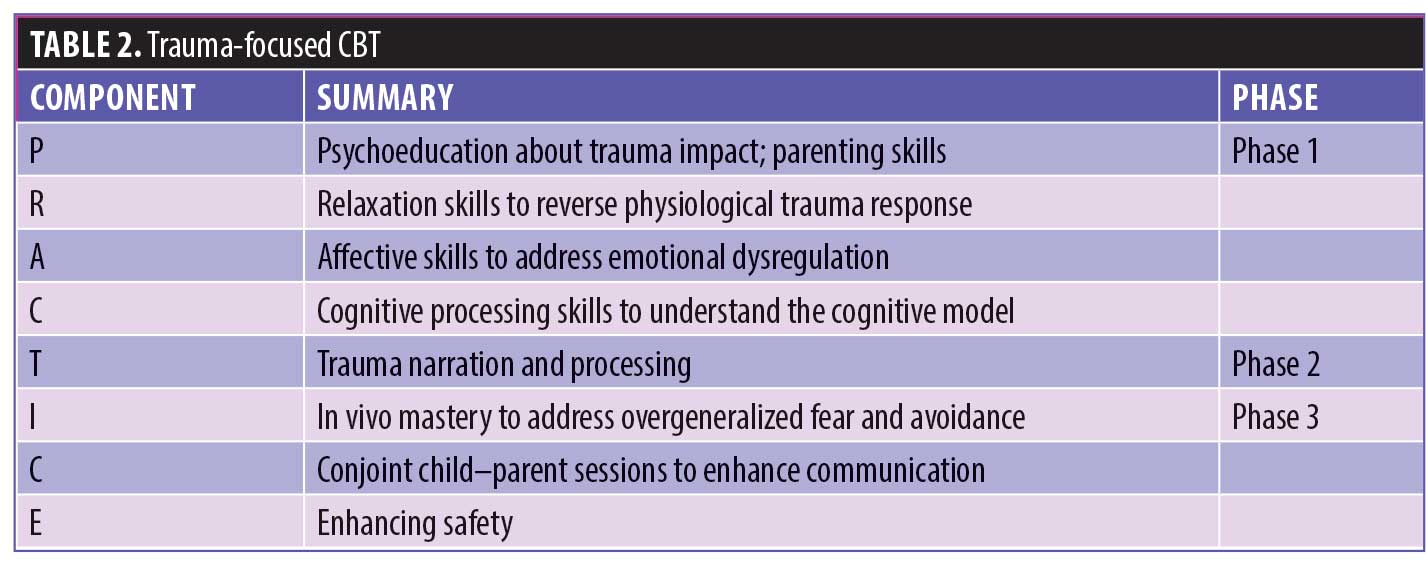

One of the main tasks of TF-CBT is collecting the trauma narrative. Over the course of several sessions, the child is encouraged to discuss in detail the events surrounding the traumatic event.
Composite case vignette 2. The patient is an 11-year-old boy who has survived repeated sexual abuse from his uncle who had also been his basketball coach. After a year of abuse, explicit photographs of several children, including the patient, were discovered on the abuser’s phone by his wife and the authorities were alerted. The patient’s parents were informed of the abuse, as were the parents of other children, which led to the patient coming to therapy. The patient has displayed sullen affect and has been increasingly withdrawn since his abuse was made known to his parents.
Dr. C.—Today, I would like us to talk about your coach.
E.—Which coach?
Dr. C.—The coach who is in jail.
E.—Do we have to talk about him?
Dr. C.—Do you feel uncomfortable talking about him?
E.—Yeah, I don’t like talking about him.
Dr. C.—Why is that?
E.—It just makes me think of bad memories.
Dr. C.—What kind of bad memories?
E.—Just about what happened.
Dr. C.—I think it would be helpful if we could talk about what happened. Can you tell me what he did?
E.—He took pictures of me and the other guys when we had our clothes off.
Dr. C.—Where did this happen?
E.—In the locker room.
Dr. C.—How are you feeling right now?
E.—Sad…like I did something wrong. Freaking out, like I can’t breathe.
Dr. C.—Remember your breathing exercise? Do you think need to do that now?
E.—I think I’m okay.
Dr. C.—Okay. If you feel like you need to, you can. Did you also feel that way when he was taking pictures?
E.—Yeah, when it happened, it wasn’t just sad it was also…I felt scared because I didn’t really know what was happening, and I knew it was wrong.
Dr. C.—Are you feeling scared now?
E.—No, not as much.
Dr. C.—Do you feel safe?
E.—Yeah, kind of. I just don’t like talking about it.
Dr. C.—I see that this is tough for you, but I’m glad to hear that you feel safe. You are in a safe place. The feelings you’re having now are because of something that already happened. It’s okay to feel that way, and it’s okay talk about it. I’m here to help you feel less bad.
This vignette demonstrates the task of eliciting a trauma narrative. It might take one or two sessions to obtain the full narrative and, while a well-meaning therapist will want to address cognitive distortions and challenge negative automatic thoughts, the true task lies in gathering the telling of the trauma. Unhelpful thoughts can be processed afterward. Of note, this is the only component of Phase 2. Before eliciting the trauma narrative, it is important to teach the patient and parents/guardians about the impact of trauma, parenting skills, and relaxation skills that can replace the trauma response. Here, Dr. C. does this by offering space for the patient to do the breathing exercise. Reminding a patient that this is an option can be enough of a reminder that the patient has control, but Dr. C. also could have taken time to practice solidifying this skill as a useful method of managing overwhelming feelings. The Vanderbilt University’s workbook for eliciting a trauma narrative outlines the goals and process, with an emphasis placed on the gradual and repetitive nature of the psychotherapy.10
After collecting the trauma narrative, Dr. C. will work with E. on processing the trauma by examining and testing the validity of cognitive distortions surrounding the trauma. As with psychodynamic psychotherapy, inspecting thoughts as well as putting words to feelings and fears is an important part of TF-CBT.
Practice points for TF-CBT.
- Gathering a traumatic narrative in TF-CBT allows the therapist and patient to later evaluate automatic thoughts and cognitive distortions.
- The therapeutic alliance allows for the painful work of processing trauma to be conducted.
- Guilt can be a major impediment to discussing trauma, and working through reluctance with patience, kindness, and optimism is an
important part of TF-CBT.
Eye Movement Desensitization and Reprocessing
EMDR is a psychotherapy designed to alleviate distress associated with traumatic memories.11 During therapy, the therapist will move his or her fingers back and forth in front of the patient’s face so that the patient follows with his or her eyes. Some therapists will use other rhythmic techniques such as deploying a metronome or tapping his or her foot or hand. While the patient follows the rhythmic movement with his or her eyes, the therapist will ask the patient to recall a traumatizing event. The therapist then asks the patient to gradually shift negative thoughts to more pleasant ones. While the hallmark of EMDR is the regular back and forth of lateral eye movements—called bilateral stimulation—while focusing on the disturbing memory, there are eight phases, as described in Table 3.12

Composite case vignette 3. This vignette demonstrates the portion of treatment where the therapist and patient collaboratively choose a ‘target’ or trauma that will be the focus of treatment. Only certain portions of EMDR use eye movement, and determining the target is a portion that does not use eye movement.
Dr. A.—We talked last week about your problems with sleep—that the memories and thoughts pop into your head. We planned that we would be finding targets this week.
Ms. B.—I am not looking forward to this.
Dr. A.—Oh, I get it. It is difficult. I also think you’d feel better after we work though some of the things that have happened to you.
Ms. B.—I guess.
Dr. A.—Where did you want to start?
Ms. B.—Probably with my abusive ex-husband. I was reminded of something when I headed over to your office today. Whenever I smell someone wearing his cologne, I lose it. I was on an elevator once and when a guy got on smelling like that, I pushed all the buttons to get the elevator doors open. They must have thought I was nuts.
Dr. A.—It sounds frustrating to feel like you’re at the mercy of these reactions.
Ms. B.—Yeah, it would.
Dr. A.—You mentioned wanting to work on something that happened a little more recently.
Ms. B.—I don’t think I’m ready for that one yet. I just don’t want to talk about it today.
Dr. A.—That’s fine. I want to keep it on our radar to work on in the future. Of course, when you feel ready.
This vignette demonstrates that, again, as with psychodynamic psychotherapy and TF-CBT, the therapist encourages a strong therapeutic alliance and empathy to lay the groundwork for trust and the discussion of difficult topics. The therapist allows the patient to choose what the topic will be. Some patients prefer to start with less traumatic events, while others immediately want to tackle the most distressing target. EMDR differs from other treatments in that bilateral stimulation—the back-and-forth of, e.g., a metronome, two fingers, or of an oscillating light bar—is used during processing of targets.12 The therapist would then continue with the patient to process the target using eye movements to desensitize the patient to their distressing memories while practicing self-regulation skills. Though some evidence suggests that eye movements are not necessary to evoke the improvements seen in EMDR,13 this technique, as a whole, has been found to be effective as a treatment for PTSD.14
Practice points for EMDR.
- The source of the bilateral stimulation in EMDR is not as important as the back-and-forth motion.
- Reprocessing targets serves to desensitize the patient to the distress previously evoked by the traumatic memories.
- Continuing to build up self-soothing skills also promotes confidence and a sense of mastery and agency in the survivor of sexual abuse and assault.
General Guidelines for Treatment
There are several suggested ways14,15 to work with patients in any psychotherapeutic modality, including normalizing and validating feelings, being nonjudgmental, and showing compassion (Table 4).

Manage transference and countertransference. The therapeutic alliance is categorized by a warm emotional bond. It is not unusual in treatment for patients to have feelings for their therapists. On occasion, a patient who is a sexual assault and/or abuse survivor will use sexualization as a defense mechanism. When patients with abuse histories are decompensated, they might feel that their sexuality is their only valuable part. Attempting to engage with the therapist on a sexual level could be an attempt by the patient to please or placate the therapist or to distract them from painful topics. The most important goal of the therapist in these situations is to maintain appropriate, safe boundaries. A patient might act-in, using defenses in session to replay or re-enact certain feelings or behaviors, and these can be of a sexual nature. A patient, e.g., might want to tell explicit sexual stories or dress provocatively. Again, the role of the therapist is to maintain appropriate, healthy boundaries. This can be done by gently noting when a patient might be acting in a sexualized manner, e.g., “it seems like you are wanting something from me that I can’t and won’t do.” Putting words to feelings rather than acting on them is one of the key components in psychotherapy.
Create a safe place. Creating a welcoming, safe space in the session allows patients to discuss difficult topics. However, even a well-meaning therapist can feel compelled to ask for details that are not in the service of the patient’s well-being and growth. The use of supervision with an experienced therapist-supervisor can be helpful if a therapist struggles between helping a patient and wanting to know details to address their own curiosity, e.g., “was your attacker attractive?” or “what did you wear to the party?” Awareness of common rape myths—that somehow drinking alcohol makes the individual who was sexually assaulted responsible for letting things get out of control or that rape must be perpetrated with violence—can be helpful in navigating treatment with survivors of sexual assault.16 Ensuring that the questions being asked are appropriate and helpful to the patient is the minimum acceptable.
Therapists are typically used to hearing difficult stories, but the interpersonal betrayal of sexual abuse and assault can be particularly difficult to bear. One of the axioms of psychoanalysis is “don’t just do something; sit there!” This is particularly useful information when working with survivors of sexual assault. The therapist might feel compelled to act—to intervene, on behalf of a patient, with the patient’s spouse, supervisors, or landlord—but sitting with a patient and bearing witness to the patient’s account is often the most helpful approach. Pain, frustration, and despair are not unusual feelings for a therapist to have but so, too, are hope and joy.
Composite case vignette 4.Ms. B, from case vignette 1, has been seeing Dr. A for treatment for several months. They have been working on Ms. B’s feelings about her sexual abuse.
Dr. A.—You were telling me about that day.
Ms. B.— I am enraged. Furious. I worry that I’ll be engulfed and eaten alive by it.
Dr. A.—That your stepdad abused you?
Ms. B.—Yes, that it happened and that I didn’t protect my sister; that it was somehow my fault like my mom said; that my mom was there and didn’t do anything; and, even now, she says that it didn’t happen or, if it did happen, it was my fault and that my family believes him over me, still, even though they’re MY family!
Dr. A.—[starting to feel overwhelmed] – Wow. That is a lot.
Ms. B.—I KNOW. Do you think I don’t know?! And this makes it even worse. I’m too much for everyone. They can’t stand to be near me, and I’m left alone, damaged, and with nothing.
Dr. A.—[deep breath, remembers Ms. B. is not mad at Dr. A.]—I know your family isn’t in your life any longer and that sometimes you feel completely alone. I know you’ve made a life for yourself.
Ms. B [laughs bitterly]—Well, it’s cold comfort to know that he was never punished and that I’m the one who has to be punished.
Dr. A.—I agree. It isn’t fair. But you held this secret all by yourself for so many years.
Ms. B.—Ugh, fine. I guess I’ve felt better since I started coming here, but I feel worse, too. It is so hard to drag myself in here every week to go over this. I feel like I’m falling apart.
Dr. A.—Are you, though? Falling apart?
Ms. B.—I guess not. I feel pretty strong today.
This vignette demonstrates how intense emotions can emerge in session, but, here, Dr. A. creates an environment where Ms. B. can talk about her rage and disappointment. Because Dr. A. is not actually overwhelmed or hurt by listening to Ms. B., Ms. B. begins the process of examining her feelings and reactions. This allows a more nuanced introspection that can bring solace and understanding. If Ms. B. had become too upset or became inappropriate, Dr. A. could have redirected her with a statement like, “I can’t hear what you’re saying when you’re yelling at me” or “time out; I think it’s getting too hot. Let’s do our five senses mindfulness grounding exercise, and then we can come back to that.”
Further reading. Every patient deserves individualized care that is compassionate and helpful. There are some specific resources for sexual assault survivors. The Sexual Trauma Workbook for Teen Girls is a guide for recovery from sexual assault and abuse.17 Additionally, Opening the Door focuses on therapy for male survivors of sexual abuse.18 Finally, the Rape, Abuse & Incest National Network is an American nonprofit anti–sexual assault organization and has many local and national resources that survivors and family can reference.19
Conclusion
The CDC estimates that sexual violence affects one in three women and one in four men over the course of their lifetimes. Survivors of sexual assault can benefit from several types of psychotherapy including psychodynamic psychotherapy, TF-CBT, and EMDR. Processing abuse and trauma is a helpful and necessary step to recovery and is the main focus in these treatment modalities. General considerations for working with survivors of sexual abuse and assault are awareness of common pitfalls, managing transference and countertransference, and avoiding retraumatization.
References
- Burgess AW, Holmstrom LL. Rape trauma syndrome. Am J Psychiatry. 1974;131(9):981–986.
- Rose DS. “Worse than death”: psychodynamics of rape victims and the need for psychotherapy. Am J Psychiatry. 1986;143(7):817–824.
- Smith SG, Zhang X, Basile KC, et al. The national intimate partner and sexual violence survey: 2018 data brief—updated release. Available at: https://www.cdc.gov/violenceprevention/pdf/2015data-brief508.pdf. Accessed February 6, 2020.
- Levi O, Bar‐Haim Y, Kreiss Y, Fruchter E. Cognitive–behavioural therapy and psychodynamic psychotherapy in the treatment of combat‐related post‐traumatic stress disorder: s comparative effectiveness study. Clin Psychol Psychother. 2016;23(4):298–307.
- Paintain E, Cassidy S. First‐line therapy for post‐traumatic stress disorder: a systematic review of cognitive behavioural therapy and psychodynamic approaches. Couns Psychother Res. 2018;18(3):237–250.
- Gabbard GO. Long-term Psychodynamic Psychotherapy: A Basic Text. Washington DC: American Psychiatric Publishing; 2017: 3–4.
- Cohen JA, Mannarino AP, Perel JM, Staron V. A pilot randomized controlled trial of combined trauma-focused CBT and sertraline for childhood PTSD symptoms. J Am Acad Child Adolesc Psychiatry. 2007;46(7):811–819.
- Cabaniss DL. Psychodynamic Psychotherapy: A Clinical Manual. West Sussex, UK: John Wiley & Sons; 2016.
- Cohen JA, Deblinger E, Mannarino AP. Trauma-focused cognitive behavioral therapy for children and families. Psychother Res. 2018;28(1):47–57.
- Vanderbilt University. Trauma narrative. Available at: https://www.mc.vanderbilt.edu/coe/tfcbt/workbook/Trauma%20Narrative/Trauma%20Narrative%20Goals%20and%20Process.pdf. Accessed: January 19, 2020.
- Shapiro F, Snyker E, Maxfield L. EMDR: eye movement desensitization and reprocessing. In: Kaslow FW, Patterson T (eds). Comprehensive Handbook of Psychotherapy, Cognitive-Behavioral Approaches. West Sussex, UK: John Wiley & Sons. 2004; 248–254.
- Shapiro R, Brown LS. Eye movement desensitization and reprocessing therapy and related treatments for trauma: an innovative, integrative trauma treatment. Practice Innovations. 2019;4(3):139.
- Davidson PR, Parker KC. Eye movement desensitization and reprocessing (EMDR): a meta-analysis. J Consult Clin Psychol. 2001;69(2):305–316.
- Cusack K, Jonas DE, Forneris CA, et al. Psychological treatments for adults with posttraumatic stress disorder: a systematic review and meta-analysis. Clin Psychol Rev. 2016;43:128–141.
- Women’s Health: Treating Survivors of Sexual Assault. (August 2019). Women’s Health. DOI 10.2310/7800.13087. Decker Psychiatry.
- Hockett JM, Saucier DA, Badke C. Rape myths, rape scripts, and common rape experiences of college women: Differences in perceptions of women who have been raped. Violence Against Women. 2016;22(3):307–323.
- Lohmann RC, Raja S. The Sexual Trauma Workbook for Teen Girls: A Guide to Recovery from Sexual Assault and Abuse. Oakland, CA: Instant Help; 2016.
- Crowder A. Opening the Door: A Treatment Model for Therapy with Male Survivors of Sexual Abuse. Oxfordshire, UK: Routledge; 2014: 1–226.
- Rape, Abuse & Incest National Network. Materials. Available at: https://www.rainn.org/materials. Accessed January 30, 2020.
