 by Dharmendra Goyal, MD; Mashal Khan, MD; Bushra Qureshi, MD; Catherine Mier, MD; and Steven Lippmann, MD
by Dharmendra Goyal, MD; Mashal Khan, MD; Bushra Qureshi, MD; Catherine Mier, MD; and Steven Lippmann, MD
All from the University of Louisville School of Medicine, Department of Psychiatry, Louisville, Kentucky
Innov Clin Neurosci. 2014;11(1–2):26–28
Funding: There was no funding provided for the preparation of this manuscript.
Financial disclosures: The authors have no conflicts of interest relevant to the content of this manuscript
Key words: Fahr’s disease, idiopathic basal ganglia calcification, movement disorder, cognitive deficit, CT scan, cerebral calcification, dementia
Abstract
Idiopathic basal ganglia calcification or Fahr’s disease is a neurological condition with a prominent movement disorder. Diagnostically, brain imaging with computerized tomographic scanning reveals bilateral brain calcifications, usually of the basal ganglia. A positive family history is very common, along with a generational anticipatory effect, thus familial basal ganglia calcification is an alternative name. Cognitive deficits and psychiatric symptoms are often present. This progressive disease has no cure, but symptomatic treatment may be beneficial.
Introduction
Idiopathic basal ganglia calcification or Fahr’s disease is a genetic condition characterized by calcification of the brain.[1,2] Calcification is documented in the basal ganglia, especially the globus pallidus, and with occasional involvement of the internal capsule, thalamus, and cerebral white matter.[1,2] The onset is bimodal, occasionally in children, but more commonly in adults in their fourth to sixth decade.[3,4] Patients have a wide range of presentations with prominent extrapyramidal symptoms, pyramidal tract signs, cognitive impairment, behavioral dysfunction, and psychoses.[5] Computerized tomographic (CT) brain imaging evidences prominent, bilateral cerebral calcification.[4]
Clinical vignette
An 18-year-old woman was hospitalized for irritability and aggressive, dyscontrolled behavior. The past history documented that a neurological and cognitive dysfunction had been present for many years, but was getting worse in recent weeks with deteriorating school performance. The records revealed a progressive dementia diagnosed as Fahr’s Disease. The diagnosis was confirmed four years previously by CT scanning-evidence of symmetrical basal ganglia calcifications (Figure 1); cognitive impairment was present in several relatives. The past laboratory profile was unremarkable for hemogram, chemistry profile, sedimentation rate, rheumatoid factor, antinuclear antibodies, thyroid functions, and levels of pyruvate, lactate, and ceruloplasmin.
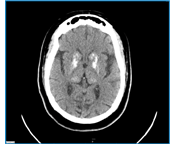
On the current physical examination, bilateral hand tremors were noted. The mental status testing evidenced a pattern consistent with dementia. A new comprehensive laboratory screening review was unremarkable and with normal parathyroid hormone and calcium levels. The present CT scanning (Figure 2) evidenced a progressive component to the calcification. The behavioral aspects improved somewhat once the patient was prescribed asenapine. Dementia remained static, but she required institutionalization due to continued dissocial behavior.
Discussion
Cerebral calcification is the hallmark of Fahr’s disease, characterized by bilateral basal ganglia involvement.[1,2,6] It is an inherited, usually autosomal dominant disorder, rarely observed in an autosomal recessive pattern.[7] The genetic heterogeneity evidences a generational, anticipatory effect, and is reflected in familial basal ganglia calcification as an alternate name. The causal genes remain unidentified, but there is a linkage to chromosome 14q (IBCG1) in some multigenerational families.[7] The CT scan is the most accurate diagnostic test, and it is better than magnetic resonance imaging at identifying calcification.[4,8] A Fahr’s disease diagnosis is confirmed when bilateral brain calcifications occur in cases with movement disorders. Psychiatric and cognitive complaints along with a positive family history are also often present. The cause of the brain calcification is not known, but it may be related to hyperphosphatemia.[9]
Other differential diagnoses to rule out would generally include hypoparathyroidism, toxoplasmosis, rubella, cytomegalovirus, cysticercosis, autoimmune deficient syndrome, Wilson’s disease, Cockayne syndrome, tuberous sclerosis, and rarely Down’s syndrome. Always consider idiopathic basal ganglia calcification in persons with cognitive and movement disorders and behavioral abnormalities, especially when there is a familial component.[1,2,6,7] CT scanning of the head would then be indicated diagnostically.[4,8]
Laboratory parameters in most patients reveal normal calcium, phosphorus, and parathyroid hormone (PTH) levels, but some individuals present with hypocalcemia and an inappropriately normal PTH, which warrants the exclusion of hypoparathyroidism. Considering that the disease has an idiopathic component, a careful investigation to rule out hypoparathyroidism is warranted since that endocrinopathy may produce similar neurological presentations. The diagnosis of primary hypoparathyroidism is usually confirmed by the concurrence of low parathyroid hormone and serum calcium concentrations. Secondary hypoparathyroidism is associated with low PTH and high calcium levels. Pseudohypoparathyroidism is a condition of bone and kidney disease, resulting in unresponsiveness of receptors to parathyroid hormone; findings include high PTH concentrations and low calcium assays.
There is no cure for Fahr’s disease; treatment is symptomatic. Neurological pathologies do not respond to conventional therapies, e.g., parkinsonianism fails to improve when levodopa is prescribed.[10] However, risperidone is documented to diminish psychotic symptoms.10 Calcium, vitamin D, and parathyroid hormone administration can be helpful at normalizing calcium levels in cases with concurrent hypoparathyroidism, and may improve the patient’s neurological status.9 One case report described an improvement with bisphosphonate administration.[11]
A recent literature review reveals a case report of Fahr’s disease presenting with dementia associated with cognitive, behavioral, and movement disorders. Calcifications were documented in basal ganglia and dentate nuclei of the cerebellum.[12] Some patients may present with fatigue, vertigo, dystonia, and clumsiness; muscular atrophy may appear as the disease progresses.
Conclusion
Idiopathic basal ganglia calcification or Fahr’s disease should be considered in the differential diagnosis of patients who present with movement disorders. This is especially true when there is a history of neurological illness, mental status changes, or behavioral issues in patients and/or their families. CT scanning would confirm the diagnosis if it reveals bilateral calcifications in the brain, especially the basal ganglia.
References
1. Malik R, Panday VK, Naik D. Fahr’s disease: a rare neurodegenerative disorder. Int J Radiol Image. 2004;14:383–384.
2. Baba Y, Broderick DF, Uitti RJ, et al. Heredofamilial brain calcinosis syndrome. Mayo Clinic Proc. 2005;80:251–256.
3. Manyam BV, Bhatt MH, Moore WD, et al. Bilateral striopalliododentate calcinosis: cerebrospinal fluid, imaging and elctrophysiological studies. Ann Neural. 1992;31:379–384.
4. Billard C, Dulac O, Boulouche J, et al. Encephalopathy with calcifications of basal ganglia in children: a reappraisal of Fahr’s disease with respect to 14 new cases. Neuropediatrics. 1989;20:12-19.
5. Shakbai SV, Johnson JP, Bourgeois JA. Paranoid delusions and cognitive impairment suggesting Fahr’s disease. Psychosomatics. 2005;46:569-572.
6. Kartin P, Zupevc M, Pogacnik T, et al. Calcification of basal ganglia, postoperative hypoparathyroidism and extrapyramidal, cerebellar, pyramidal motor manifestations. J Neurol. 1982;227:171–176.
7. Oliviera JR, Spiteri E, Sobrido MJ, et al. Genetic heterogeneity in familial idiopathic basal ganglia calcification (Fahr’s Disease). Neurology. 2004; 63:2165–2167.
8. Lippmann S. Emergency brain imaging: CT or MRI? Current Psychiatry. 2013;12(3):47.
9. Hossain M. Neurological and psychiatric manifestations in idiopathic hypoparathyroidism: response to treatment. J Neurol Neurosurg Psychiatry. 1970;33:153–157.
10. Sobrido MJ. Hopper S. Geschwind DH. Familial idiopathic basal ganglia calcification. GENE Reviews. 2007;1–15.
11. Loeb JA. Functional improvement in a patient with cerebral calcinosis using a bisphosphonate. Mov Disord. 1998;13(2):345–349.
12. Calabro RS, Spadaro L, Marra A, et al. Fahr’s disease presenting with dementia at onset: a case report and literature review. Behav Neurol. 2013 Sep 12. [Epub ahead of print].
