
by Samara White, PharmD; Tammie Lee Demler, BS, PharmD, MBA, BCGP, BCPP; Eileen Trigoboff, PMHCNS-BC, DNS, DABFN; Lucy Keers, PharmD; and Chloe Matecki, PharmD
All authors are with Department of Pharmacy Practice, State University of New York at Buffalo, School of Pharmacy and Pharmaceutical Sciences in Buffalo, New York. Drs. Demler and White are additionally with Department of Pharmacy, New York State Office of Mental Health in Buffalo, New York. Drs. Demler and Trigoboff are additionally with the Department of Psychiatry, State University of New York at Buffalo, Jacobs School of Medicine and Biomedical Sciences in Buffalo, New York.
Funding: No funding was provided for this article.
Disclosures: The authors have no conflicts of interest relevant to the contents of this article.
Innov Clin Neurosci. 2023;20(10–12):18–22.
Abstract
Purpose: The perceptions and responses to acute states of emergency may vary for people experiencing serious mental illness (SMI). Therefore, studying the mental health toll of the COVID-19 pandemic on psychiatric inpatients can inform psychiatric care in the event of future global crises. The objective of this study was to determine if there was a difference in the incidence of mental health manifestations in an adult inpatient state psychiatric facility during the COVID-19 pandemic, compared to the immediately preceding year.
Methods: Medication administration history for patients who utilized an as needed (PRN) medication for anxiety, agitation, or psychosis between March 1, 2020, and February 28, 2021, were analyzed. Secondary data on the incidence of restraints and seclusions were also examined.
Results: The total number of PRN medications was higher during the pre-COVID-19 time frame than during the pandemic (8,139 vs. 7,630), but this was not statistically significant. The following assessments were statistically significant: predominance of psychosis as a psychiatric symptom during the COVID-19 time frame (557 vs. 389), and the difference in PRN medication administration times between time frames as categorized by day (3,741 vs. 2,623), evening (3,844 vs. 4,239), and night (554 vs. 768).
Conclusion: During the height of the COVID-19 pandemic, the use of PRN medications for psychosis increased and the use of PRN medications for anxiety and agitation decreased among inpatients at a state psychiatric hospital. These results suggest that experiencing a worldwide pandemic in a psychiatric inpatient facility may be protective in some respects but may exacerbate symptoms of psychosis.
Keywords: COVID-19, psychiatric inpatients, mental health
The worldwide crisis caused by the severity of illness, rapid transmission, and lack of pharmacologic interventions for the novel severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) escalated rapidly, and the World Health Organization (WHO) elevated the resulting coronavirus disease 2019 (COVID-19) designation from a public health emergency to full pandemic status on March 11, 2020.1–3 Subsequently, the mandated, government-imposed restrictions and quarantine orders that were issued for public health protection resulted in significant emotional distress, social isolation, financial strain, poor physical health, and decreased quality of life for the global population.2–6 Compounding these stressors were the reduced access to healthcare and social services, disruption in routines, and the fear, uncertainty, and grief associated with COVID-19 that also contributed to the increase in new onset and exacerbation of pre-existing mental health conditions for many people.1,4–7 According to the United States (US) Centers for Disease Control and Prevention (CDC), the prevalence of anxiety disorder symptoms increased three-fold (25.5% vs. 8.1%) and symptoms of major depressive disorder increased approximately four-fold (24.3% vs. 6.5%) in the US during the first year of the pandemic, compared to the year preceding the pandemic.8 According to a collection of surveys from Mental Health America, 76 percent of Americans experienced moderate-to-severe symptoms of any mental health condition, which translated to a two-percent increase from 2019 to 2021.9 Other results from these surveys comparing data from 2019 and 2021 demonstrated a 422-percent increased incidence of anxiety, 188-percent increased incidence of psychosis, and eight-percent increased risk of suicidal ideation.9
In the US, the residual mental health effects that arose from the COVID-19 pandemic have persisted well past the height of the pandemic and even well after restrictions and quarantine orders eased. Notable common mental health manifestations and symptoms during the COVID-19 pandemic included increased incidence of depression, anxiety, fear, anger, irritability, psychological distress, substance use, suicidal ideation, and poor sleep quality, which have been well-documented and studied in the general population.1,3–7,9,10 However, the mental health impacts of the pandemic have not been as well explored in psychiatric inpatients, a population that is considered to be more vulnerable to stressors, restrictions, medication shortages, and disruption in healthcare services, and have a higher risk of relapse and severe negative mental health outcomes.1,4,7,10–13
Many factors complicate care for people with psychiatric disorders. Of note, the perceptions and responses to what is typically considered an acute state of emergency may vary for people experiencing serious mental illness (SMI), compared to the general population.11,14,15 Depending on the severity of illness, people with mental health conditions may not fully comprehend the severity or global impacts of a pandemic, but they endure more severe and prolonged emotional distress from pandemic-imposed stressors and stay-at-home orders, compared to healthy controls.11–14,16 The stressors that the pandemic imposed on the general population that psychiatric inpatients typically do not experience include, but are not limited to, employment concerns, financial strain, and decreased access to both essential resources and discretionary luxuries. However, the impacts of the common stressors that were experienced both in the community and within the inpatient psychiatric population, such as the fear of infection, restriction of voluntary activities and/or hobbies, boredom, frustration, grief, lack of social connection, and stigma of COVID-19 infection, may have exceeded the coping capacity of psychiatric inpatients, resulting in exacerbation of mental health conditions.1,5,11–15,17,18 Additionally, the stressors that uniquely affected psychiatric inpatients, such as hospital staffing challenges, facility environment concerns, and lack of intrapersonal agency with infection control policies, may have further added to the existing mental health toll within this population.11
There are irrefutable benefits to studying the clinical and pharmacologic impacts of COVID-19 in people experiencing SMI specifically due to the pharmacokinetic consequences of infection-related organ dysfunction, which may particularly interfere with psychotropics with narrow therapeutic indexes.19–22 However, it is equally important to study the emotional and mental health impacts of COVID-19 in psychiatric inpatients due to the ability to improve patients’ mental healthcare and inform providers how care can optimally be delivered to this population during a global state of emergency.1,6,14,23 The objective of this study was to determine if there was a difference in the incidence of mental health manifestations in an adult inpatient state psychiatric facility during the first year of the COVID-19 pandemic, compared to the immediately preceding year.
Methods
This study was a retrospective analysis evaluating the mental health impact of the COVID-19 pandemic on patients at a state adult inpatient psychiatric facility in Buffalo, New York, USA. The primary data for this study, which included the frequency and indication for use of administered as needed (PRN) psychiatric medications, was extracted from the facility’s electronic medical record (EMR) system. These data were grouped into two time frames: March 1, 2019, to February 28, 2020, (designated as the pre-COVID-19 period) and March 1, 2020, to February 28, 2021 (designated as the COVID-19 period). Supporting secondary data from the use of restraint and seclusion behavioral de-escalation tactics were also extracted from the institution’s EMR to provide a fuller understanding of the frequency, timing, and magnitude of behavioral exacerbations.
The inclusion criteria for this study included all patients in a state adult inpatient psychiatric institution who used a psychiatric PRN medication for the following indications: agitation, anxiety, irritation, nervousness, and psychosis. The exclusion criteria were patients with a state-defined status of criminal procedure law (CPL) designation. The study questions that were examined are as follows:
- Did the COVID-19 pandemic change the use of psychiatric PRN medications for psychiatric inpatients?
- Were the three categories of psychiatric symptoms (as represented by PRN medication use) different from before the COVID-19 pandemic to during the COVID-19 pandemic?
- Was there a psychiatric symptom (as represented by PRN use) with a predominant difference between the two time frames?
- Was the mode of timing for the administration of PRN psychiatric medications different between the two time frames?
Data analysis. PRN medication use was analyzed using a Chi-squared test, and PRN frequencies were categorized by indication. Continuous data were analyzed using a t-test with a significance threshold of 0.05. Descriptive statistics were used to summarize restraint and seclusion data.
Results
A total of 142 patients in the pre-COVID-19 time frame and 135 patients in the COVID-19 time frame were included in this study. A comparison of pre-COVID-19 and COVID-19 data can be found in Table 1. The data showed that 8,139 PRN medications were used in the pre-COVID-19 time frame, and 7,630 PRN medications were used during the COVID-19 time frame; however, this difference was not statistically significant (p=0.34). The PRN medications per indication were as follows during the pre-COVID-19 and COVID-19 time frames, respectively: agitation, 3,915 versus 3,590; anxiety, 3,829 versus 3,477; and psychosis, 395 versus 563, of which only the results for psychosis were statistically significant (p=0.001). There were 66 participants that utilized a psychiatric PRN medication in both time frames; however, none of the dependent variables were found to have a statistically significant difference within this subset of patients, as p-values ranged from 0.09 to 0.47 for the three indications.
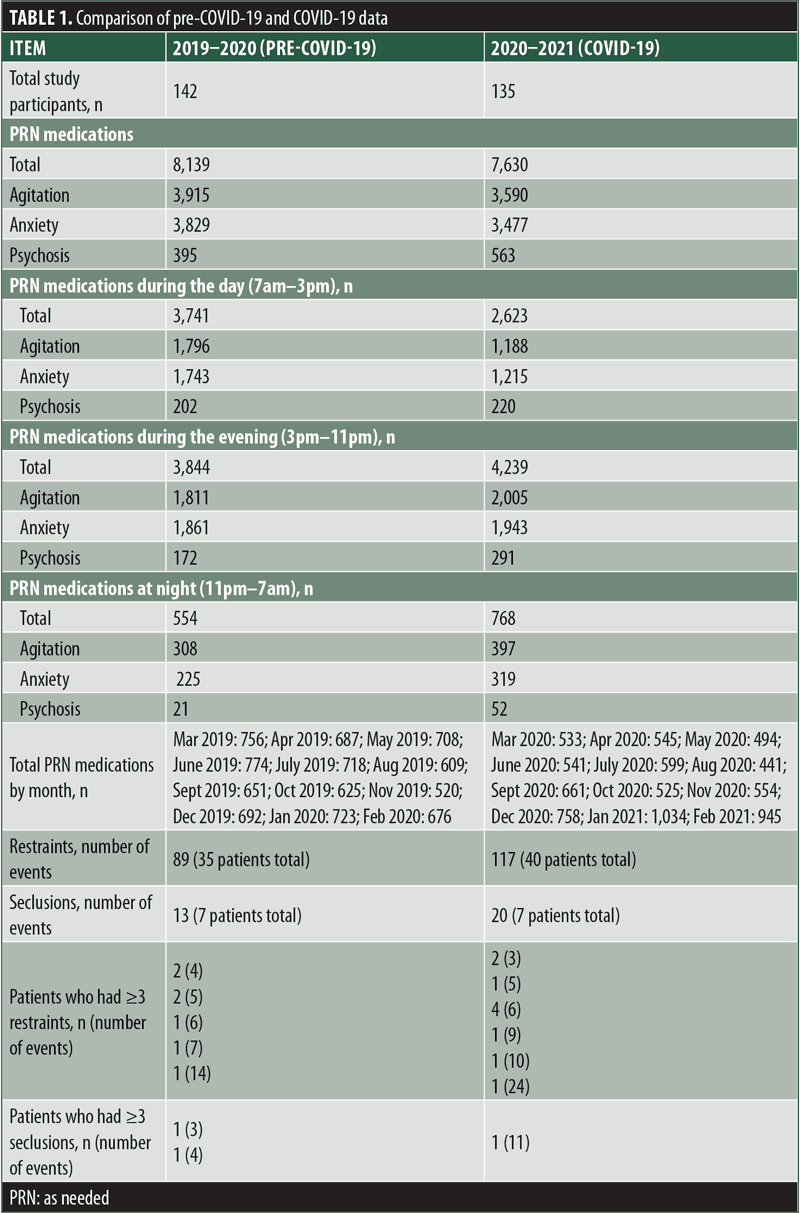
The use of PRN medications by mode of timing were categorized as day (7am–3pm), evening (3pm–11pm), and night (11pm–7am). The difference in PRN medication mode of timing was found to be statistically significant to the 0.001 level for pre-COVID-19 and COVID-19 time frames, respectively: day, 3,741 versus 2,623; evening, 3,844 vs. 4,239; and night, 554 versus 768.
There were a total of 89 and 117 restraints (35 vs. 40 patients) and 13 and 20 seclusions (7 patients both years) in the pre-COVID-19 and COVID-19 time frames, respectively. Seven and 10 participants had three or more restraints, and two and one participants had three or more seclusions in the pre-COVID-19 and COVID-19 time frames, respectively. There were three participants who had three or more restraints in both time frames, and no participants that had three or more seclusions in both time frames.
Discussion
In this retrospective study analyzing the use of PRN medications at a psychiatric inpatient facility, we found that there was no significant difference in the overall number of administered PRN medications, but that there were significantly more PRN medications used for psychosis. Additionally, we found that there was a significant increase in the use of PRN medications during evening and night time frames.
It may seem counterintuitive that psychiatric inpatients would need fewer PRN medications for agitation and anxiety during a global pandemic, especially since people with SMI may react with more severe traumatic responses to stressors.11–14,16 Considerations to explain this are as follows: 1) staff protected patients from major stressors that occurred in the community; 2) suspension of visitations may have decreased exposure to family conflicts, extreme fear experienced in the community, and risk of infection; 3) restrictions within the units and the discontinuation of usual hospital programming may have been protective due to decreased exposure to peers’ disruptive behaviors; and 4) inpatients may have been less preoccupied with issues concerning access to healthcare and overall financial strains, compared to the general population, especially since hospital discharges were paused.
Patients’ inability to perceive facial expressions due to hospital masking policies may have contributed to the increase in PRN medications for psychosis. Psychiatric patients have difficulties interpreting emotions from facial expressions, and face masks have made this even more challenging since a significant portion of the face is concealed.24,25 Another possible explanation is that neuropsychiatric sequalae from COVID-19 contributed to symptoms of psychosis. Additionally, there is a historical correlation between pandemics and psychosis; however, these studies are limited by possible misdiagnoses of psychosis that would be better described as delirium, given the large overlap of symptoms, and therefore, these findings warrant further investigation.26,27
A possible explanation for the higher frequency of PRN medications given during evenings and nights could be that patients suffered from increased boredom, loneliness, or residual effects from poor sleep quality that are experienced in the later hours of the days. Considerable professional literature supports that poor sleep quality and duration predicts increases in psychosis symptoms, negative affect, and cognitive symptoms.28
The data from restraints and seclusions suggest that behavioral exacerbations were more frequent during the pandemic than the data from our analysis of PRN medications could capture. The raw data show a 31-percent increase in the number of restraints (89 vs. 117) and a 54-percent increase in the number of seclusions (13 vs. 20). This is an important aspect that warrants further examination with a more thorough analysis.
Limitations. Analyzed data were limited to three indications of prescribed psychiatric PRN medications, namely agitation, psychosis, and anxiety, in addition to data from the incidence of restraint and seclusion tactics. Therefore, these data may not represent all psychiatric symptoms that were experienced, potentially missing symptoms including, but not limited to, insomnia, depression, and suicidal ideation. Another factor that may have been useful in providing a more robust understanding of the data would have been use of patient progress notes. This study also did not track the incidence of COVID-19 infections, which may have contributed to distinguishing delirium from psychosis.
Other limitations of this study were factors that are intrinsic to these subjects. The patient population at this institution consists of some of the most complex psychiatric cases in a four-county range; therefore, their responses may have varied from the typical psychiatric inpatient population. The magnitude of the change of psychiatric symptoms may have been minimized by the concomitant use of psychiatric medications, making it difficult to determine the true incidence of behavioral exacerbations. Psychiatric patients may have demonstrated malingering behaviors by requesting PRN medications, a common practice in this setting;29 contrary to this, it is also a possibility that patients refrained from requesting PRN medications, which would also skew data.
As the COVID-19 pandemic stressed the healthcare system with burnout, exhaustion, and traumatic experiences, some extrinsic limiting factors may potentially have affected this study.30 Inadequate staffing may have limited nurses’ capacity to administer PRN medications. Staff might have attempted to decrease the amount of time that they spent with patients as a protective measure, which might negatively affect communication between patients and staff. Nurses might have exercised their personal discretion in withholding PRN medications. There may have been a potential contribution of staff burnout as a subjective factor in the use of restraints and seclusions.
Conclusion
This study suggests that experiencing a worldwide pandemic in a psychiatric inpatient facility may be protective in some respects, specifically for symptoms of anxiety and aggression. Some of these protective factors may include evading the extreme panic that was largely experienced in the community and psychiatric inpatients’ limited contact with their peers’ disruptive behaviors. However, more data are needed to make definitive conclusions, especially as they relate to COVID-19-induced psychosis, as there are confounding factors that may make it difficult to distinguish delirium from psychosis. The increased incidence of psychosis, as found in our study, may have been precipitated by patients’ inability to perceive facial expressions due to hospital masking policies or may simply be neuropsychiatric sequelae from COVID-19 infection.
The extreme mental health toll experienced in the general population most likely stemmed from the negative social and financial constraints imposed by COVID-19; psychiatric inpatients do not share these stressors, and this may explain the difference in reactions to a global health pandemic. Therefore, it follows that the relationship of negative psychological outcomes related to the pandemic and stay-at-home orders were pronounced for people who experienced a greater change in their daily lives, as opposed to psychiatric inpatients, whose lives remained relatively unaffected, at least as it applies to lack of concern for employment unreliability, financial security, and maintaining shelter. Although psychiatric inpatients undoubtedly experience stressors and, in fact, experience more intense and prolonged distress than the general population, since psychiatric inpatients have limited autonomy at baseline, the reactions to these stressors are likely intrapsychic and do not vary much during an acute worldwide pandemic.
Since our study was limited to describing mental health exacerbations via administered PRN medications for anxiety, agitation, and psychosis, these data may not represent all psychiatric symptoms that psychiatric inpatients experienced as a result of the pandemic. In order to fully understand the impact of global health crises on patients’ mental health and ensure the capacity for adequate care, future studies should employ different mechanisms for documenting behavioral exacerbations and investigate if different types of mental health conditions have varying responses.
References
- Dalkner N, Ratzenhofer M, Fleischmann E, et al. Psychological and behavioral response on the COVID-19 pandemic in individuals with bipolar disorder: a multicenter study. Psychiatry Res. 2022;310:114451.
- AJMC Staff. A timeline of COVID-19 developments in 2020. Am J Manag Care. Updated 21 Jan 2021. https://www.ajmc.com/view/a-timeline-of-covid19-developments-in-2020. Accessed 27 Dec 2022.
- Goldenberg MN, Parwani V. Psychiatric emergency department volume during Covid-19 pandemic. Am J Emerg Med. 2021;41:233–234.
- Tull MT, Edmonds KA, Scamaldo KM, et al. Psychological outcomes associated with stay-at-home orders and the perceived impact of COVID-19 on daily life. Psychiatry Res. 2020;289:113098.
- Pfefferbaum B, North CS. Mental health and the Covid-19 pandemic. N Engl J Med. 2020;383(6):510–512.
- Poudel AN, Zhu S, Cooper N, et al. Impact of Covid-19 on health-related quality of life of patients: a structured review. PLoS One. 2021;16(10):e0259164.
- Nam SH, Nam JH, Kwon CY. Comparison of the mental health impact of COVID-19 on vulnerable and non-vulnerable groups: a systematic review and meta-analysis of observational studies. Int J Environ Res Public Health. 2021;18(20):10830.
- Czeisler MA, Lane RI, Petrosky E, et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic – United States, June 24-30, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(32):1049–1057.
- Mental Health America. Mental health and COVID-19 2021 Data. Updated Apr 2022. https://mhanational.org/mental-health-and-covid-19-two-years-after-pandemic. Accessed December 28, 2022.
- Brooks SK, Webster RK, Smith LE, et al. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. Lancet. 2020;395(10227):912–920.
- Yocum AK, Zhai Y, McInnis MG, et al. Covid-19 pandemic and lockdown impacts: a description in a longitudinal study of bipolar disorder. J Affect Disord. 2021;282:1226–1233. 10.1016/j.jad.2021.01.028.
- Chatterjee SS, Barikar CM, Mukherjee A. Impact of COVID-19 pandemic on pre-existing mental health problems. Asian J Psychiatr. 2020;51:102071.
- Druss BG. Addressing the COVID-19 pandemic in populations with serious mental illness. JAMA Psychiatry. 2020;77(9):891–892.
- Asmundson GJG, Paluszek MM, Landry CA, et al. Do pre-existing anxiety-related and mood disorders differentially impact COVID-19 stress responses and coping? J Anxiety Disord. 2020;74:102271.
- Han L, Zhan Y, Li W, et al. Associations between the perceived severity of the COVID-19 pandemic, cyberchondria, depression, anxiety, stress, and lockdown experience: cross-sectional survey study. JMIR Public Health Surveill. 2021;7(9):e31052.
- Demler TL. Addressing mental and physical health in vulnerable patients during the COVID-19 pandemic. US Pharm. 2021;46:47–57.
- Stein MB. COVID-19: psychiatric illness. UpToDate. Updated 30 Aug 2023. https://www.uptodate.com/contents/covid-19-psychiatric-illness/. Accessed 28 Dec 2022.
- Yang H, Rigsby M, Zhu X, et al. COVID-19 in long-term care facilities: a rapid review of infection correlates and impacts on mental health and behaviors. HERD. 2022;15(3):277–294.
- Rojas-Velasquez D, Lifland B, Caro MA. Supratherapeutic lithium levels in COVID-19 infection. Bipolar Disord. 2022;24(4):447–450.
- Bojdani E. Pharmacokinetic implications leading to marked valproic acid level-drop during COVID-19 treatment. Psychiatry Res. 2021;296:113701.
- Bilbul M, Paparone P, Kim AM, et al. Psychopharmacology of COVID-19. psychosomatics. 2020;61(5):411–427.
- Javelot H, Straczek C, Meyer G, et al. Psychotropics and COVID-19: an analysis of safety and prophylaxis. Encephale. 2021;47(6):564–588.
- Schou TM, Joca S, Wegener G, Bay-Richter C. Psychiatric and neuropsychiatric sequelae of COVID-19 – a systematic review. Brain Behav Immun. 2021;97:328–348.
- Escelsior A, Amadeo MB, Esposito D, et al. COVID-19 and psychiatric disorders: the impact of face masks in emotion recognition face masks and emotion recognition in psychiatry. Front Psychiatry. 2022;13:932791.
- Rinck M, Primbs MA, Verpaalen IAM, Bijlstra G. Face masks impair facial emotion recognition and induce specific emotion confusions. Cogn Res Princ Implic. 2022;7(1):83.
- Smith CM, Gilbert EB, Riordan PA, et al. COVID-19-associated psychosis: a systematic review of case reports. Gen Hosp Psychiatry. 2021;73:84–100.
- Moccia L, Kotzalidis GD, Bartolucci G, et al. COVID-19 and new-onset psychosis: a comprehensive review. J Pers Med. 2023;13(1):104.
- Meyer N, Joyce DW, Karr C, et al. The temporal dynamics of sleep disturbance and psychopathology in psychosis: a digital sampling study. Psychol Med. 2022;52(13):2741–2750.
- Bellman V, Chinthalapally A, Johnston E, et al. Malingering of psychotic symptoms in psychiatric settings: theoretical aspects and clinical considerations. Psychiatry J. 2022;2022:3884317.
- Office of the Assistant Secretary for Planning and Evaluation. Impact of the COVID-19 pandemic on the hospital and outpatient clinician workforce: challenges and policy responses. 3 May 2022. https://aspe.hhs.gov/reports/covid-19-health-care-workforce. Accessed 29 Sep 2023.
