
by Maria Fe Garcia-Rada, MPS, and Robert E. Litman, MD
Ms. Garcia-Rada and Dr. Litman are with CenExel CBH Health in Gaithersburg, Maryland. Dr. Litman is with Georgetown University Medical School in Washington, DC.
Funding: Funding was provided by CenExel Clinical Research.
Disclosures: Dr. Litman is a member of the Speaker’s Bureau for Janssen, AbbVie, and Terran Biosciences. Ms. Garcia-Rada has no conflicts of interest relevant to the contents of this article.
Innov Clin Neurosci. 2022;19(10–12):24–28.
Abstract
Introduction: Recent research on the COVID-19 pandemic suggests that individuals who suffer from serious mental illness (SMI) are at heightened risk of infection and have increased mortality due to their illness and/or lack of access to healthcare. Consequently, progress in developing new treatments for SMIs has been disrupted, with many interruptions to clinical trials in psychiatry due to concerns regarding the pandemic and its risks to patients with SMI.
Objective: This study aimed to examine the impact of the COVID-19 pandemic on patients with SMI, specifically relating to psychiatric morbidity, pandemic-induced stress, and ability to cope with pandemic-related precautionary measures, restrictions, and disruptions to daily life.
Design: A cross-sectional survey study of 94 clinical trial patients diagnosed with bipolar disorder, major depressive disorder (MDD), or schizophrenia was conducted in three geographically distinct clinical trial sites between June and September 2020. Prevalence rates were calculated for sample characteristics and demographics, and low versus high stress groups were compared on survey variables using Pearson’s Chi-squared test of independence.
Results: The results from the surveys indicated that COVID-19 knowledge, awareness, and the use of precautionary safety measures (e.g., handwashing, personal protective equipment [PPE], and social distancing) were robust and mirrored the general population. While the majority of patients reported experiencing moderate or extreme levels of distress (61.5%, n=56), high levels of stress were correlated with positive coping skills.
Conclusion: These findings suggest that clinical trial patients with SMI can safely participate in clinical trials despite the increase safety risks posed by the COVID-19 pandemic.
Keywords: Clinical trials, psychiatry, COVID-19, pandemic
Increasing evidence shows that severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), known as coronavirus disease 2019 (COVID-19) and the ensuing pandemic are associated with symptoms of psychiatric illness and psychological stress. Evidence suggests that previously healthy individuals infected with COVID-19 can present with diverse neuropsychiatric symptoms, including delirium, encephalopathy, and affective distress, including depression, anxiety, and psychosis, both acutely and chronically.1–5 In addition, psychiatric symptoms related to psychological stress caused by the pandemic, including increases in symptoms of depression and anxiety, have been documented in healthcare workers, first responders, and the general population.6–10 These are likely a result of pandemic-associated disruption of daily life routines, social isolation, job loss, restrictions imposed to reduce virus transmission, and fear of exposure to infection, among other psychosocial stressors.11–13
While many studies have investigated the psychological impact of the COVID-19 pandemic on the general population, much less is known regarding the effects the pandemic might have on patients with premorbid psychiatric illnesses, especially those with a serious mental illness (SMI). Almost from the start of the pandemic, clinical concerns were raised regarding the potential for adverse effects of the pandemic on patients with SMI, who are considered to be an especially vulnerable patient population.14 For instance, schizophrenia and bipolar disorder are often associated with cognitive deficits and comorbid medical conditions, placing this population at an increased risk for infection and adverse outcomes from COVID-19.15 Structural barriers (e.g., unstable housing) can also place individuals with SMI at a greater risk for exposure.16 Another risk factor for patients with SMI includes changes in the delivery or frequency of mental healthcare services, especially outpatient care. While in-person services can increase the risk of transmission, the lack of these types of services can contribute to service disengagement, medication nonadherence, distress, and ultimately, exacerbation of symptoms.15 Finally, consistent with these concerns, recent evidence suggests that increased mortality is associated with premorbid psychiatric illness, particularly schizophrenia-spectrum diagnoses.17,18
There is also evidence of heightened levels of psychological distress and reduced coping skills among psychiatric patients during the initial lockdown phase of the COVID-19 pandemic. Existing data from surveys of patient cohorts in countries such as Spain and China showed higher levels of anxiety, depression, insomnia, acute stress, and suicidal ideation among those with a pre-existing mental illness, compared to healthy controls.6,19–22 Additionally, some studies support a disproportionate impact of the pandemic on those with affective disorders, compared to those with psychotic disorders.23,24 One study found that individuals with affective disorders scored higher on measures of psychological distress, compared to individuals with psychotic disorders.24 Individuals with affective disorders were also more likely to report engaging in the use of protective measures, such as compliance with stay-at-home orders and the use of face masks.
Given the increased risks posed by the pandemic toward patients with premorbid psychiatric illness, we investigated the experience of patients with SMI who were current or past participants in pharmaceutical industry-sponsored clinical trials (unrelated to COVID-19) for schizophrenia, bipolar disorder, or major depressive disorder (MDD) at three clinical trials sites in the United States (US). The impetus for the survey was in part due to safety concerns, which pharmaceutical sponsors expressed regarding the advisability of continuing ongoing clinical trials or initiating new trials during the pandemic. In this study, we examined psychiatric diagnosis, psychiatric clinical status, and coping skills related to the pandemic, which we defined as patient knowledge, risk perception, and behavioral measures participants took to protect themselves and others from viral transmission (e.g., using precautionary measures, laboratory testing, and healthcare services). Psychological stress was measured using Kessler’s Psychological Distress Scale (K10).25 Based on previous research of pandemics on the mentally ill population,6,19–22 it was predicted that patients with SMI would have high levels of pandemic-related psychological distress and low levels of coping behavior.
Methods
Participants. Adults with a diagnosis of MDD, bipolar disorder, or schizophrenia (n=94) were selected for participation in the survey from three different clinical trial sites in distinct geographic areas in the US (Montgomery County, Maryland; Fulton County, Georgia; and Broward County, Florida) based on having participated in one or more psychiatry clinical trials in the previous two years and their willingness and ability to complete a survey.
Assessments. A cross-sectional structured questionnaire was derived from literature related to the impact of COVID-19 and previous pandemics (e.g., influenza) in the general population and mental health patients.26,27 The final questionnaire consisted of information on seven different categories, including demographic information, COVID-19 health and health service utilization, history of exposure to SARS-CoV-2 virus, COVID-19 knowledge, concerns regarding COVID-19 disease, risk perception, and use of precautionary measures.
In addition, psychological stress as a result of the pandemic was assessed using K10,25 a 10-item self-report scale with well-established reliability and validity that measures anxiety and depressive symptoms present within the past 30 days and yields a global measure of psychological distress.28 Responses for each question are scored on a 5-point Likert scale ranging from 1 (“none of the time”) to 5 (“all of the time”). The responses to each item are then summed and a total score is derived.
Procedures. Patients were identified through current or previous participation in a clinical trial for the treatment of schizophrenia, bipolar disorder, or MDD. Patients who were currently enrolled in a clinical trial were approached in-person by a trained interviewer during a study visit. Patients who were previously enrolled in a clinical trial were identified through a patient database and approached by a trained interviewer via telephone. All patients who were identified and interested in participating were provided with the rationale and overview of the study and, after informed consent was obtained, were invited to answer a set of questions about the impact of the COVID-19 pandemic. The interviewer administered the questionnaire in-person or over the telephone, recording all participant responses on a pen and paper survey. Data collection took place from June to September 2020.
Statistical analysis. Descriptive statistics, including prevalence rates, were calculated for sociodemographic variables and sample characteristics. A dichotomization method was used to group participant responses on the K10 into “no stress” versus “stressed” groups. This dichotomization was created by taking the median (3, or moderately distressed) of this distribution as the cut-off point. All values below 3 were grouped into the no stress category, while values of 3 or above were grouped into the stressed group. An unpaired samples t-test was then used to measure the difference between the two groups. Pearson’s Chi-squared test of independence was used to examine the differences of sample characteristics and demographic variables between no/low and high stress groups. R/R-Studio was used for all statistical analyses.
Results
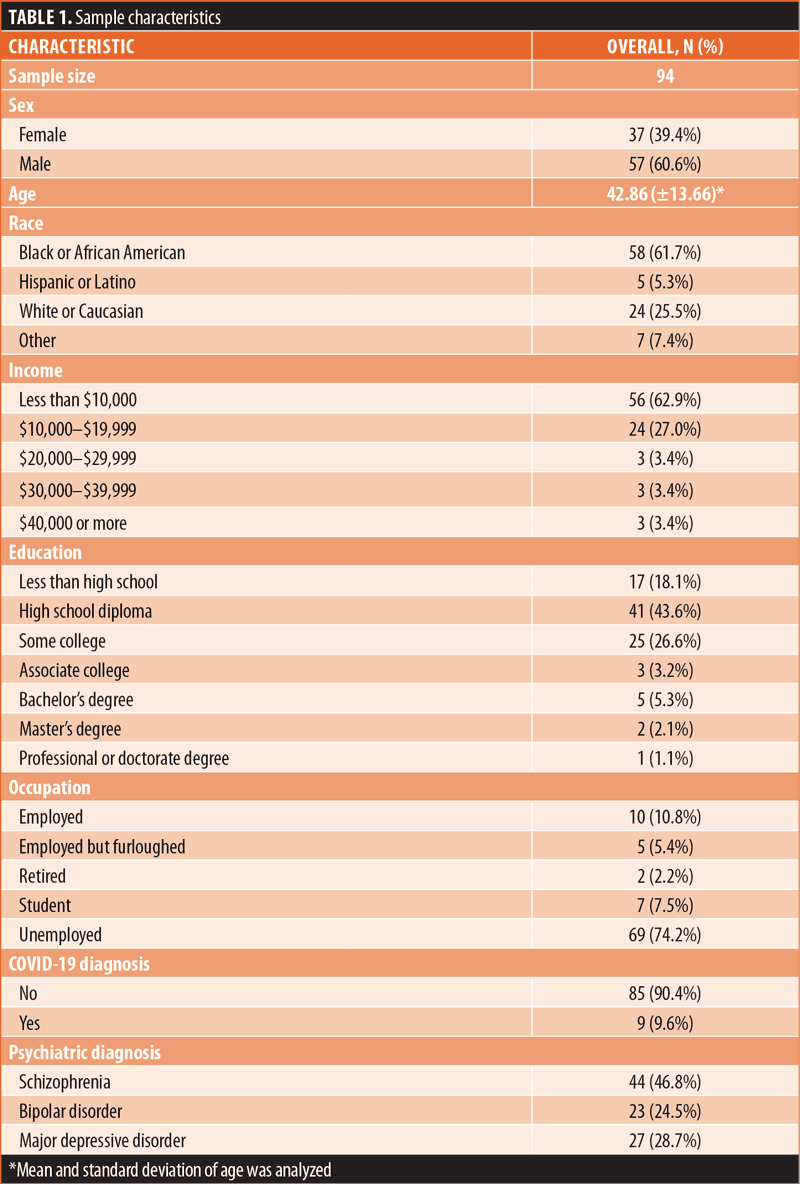
Sample characteristics (Table 1). The sample consisted of mostly male (60.6%) respondents with mean age of 42.7 years (standard deviation [SD]: 13.7). There was a higher proportion of African American/Black respondents (61.7%), followed by Caucasian/White (25.5%) and Hispanic/Latino (5.3%). The majority of the sample was of a lower socioeconomic status (79.8%), received a high school degree or equivalent (43.6%), and were unemployed at the time of the survey (74.2%). All psychiatric patients had lifetime diagnoses of schizophrenia (46.8%), bipolar disorder (24.5%), or MDD (28.7%). Nine of the patients (9.6%) had a diagnosis of COVID-19 infection at some point in their lifetime.
Knowledge about COVID-19. Forty-nine percent of patients were able to identify the common symptoms of COVID-19 disease (e.g., fever, cough, difficulty breathing) according to the US Centers for Disease Control and Prevention (CDC).29 Eighty-two percent of patients were able to correctly characterize the slope of the incidence rate of COVID-19 in the US at the time they were surveyed, and 61 percent of patients correctly identified the number of infected individuals in the US. More than half of the patients (57%) correctly identified all three methods of transmission, and 81 percent of patients identified that it is an airborne transmitted virus. The majority of patients reported that they received most of their COVID-19 information from TV sources (68%), followed by internet sources (25.6%) and family members (2.4%).
Use of precautionary measures and risk perception. Approximately two-thirds of patients reported using face masks and practicing physical distancing always or most of the time. Moreover, use of precautionary measures in this sample population mirrored trends in the general population.30 More than two-thirds of patients indicated that the use of face masks and practicing social distancing decreased risk of infection, while 69.6 percent of patients indicated washing their hands frequently decreased risk. Interestingly, patients who reported wearing personal protective equipment (PPE) were 64 percent more likely to say that they would survive a COVID-19 infection when compared to those who did not wear PPE; however, this difference was not significant (odds ratio [OR]: 1.636, 95% confidence interval [CI]: 0.71–3.80).
Healthcare and utilization of services. Eight patients (8.5%) reported being in close contact with an individual with a confirmed COVID-19 infection. Twelve patients (13%) experienced three or more symptoms of COVID-19 (e.g. fever, headache, cough, loss of taste or smell). Less than half of patients (43.6%) sought at least one medical service related to COVID-19. Among the 41 patients that had sought at least one medical service, it was found that 22 (53.7%) had undergone COVID-19 testing in the previous two weeks, 15 (36.6%) sought consultation with a physician, five (12.2%) were hospitalized, and four (9.8%) were quarantined.
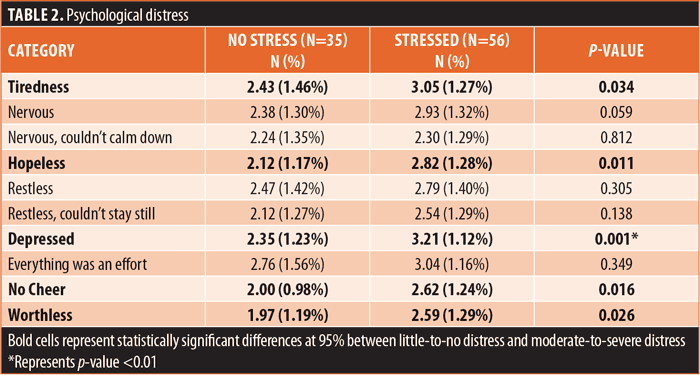
Psychiatric symptoms and psychological distress (K10) (Table 2). Forty-eight of 94 surveyed patients (51%) reported experiencing a worsening of psychiatric symptoms at the time of the survey. Similarly, dichotomization of K10 scores from the patient sample (n=91; 3 patients were missing from this sample due to missing data on K10 scores that did not allow us to dichotomize those 3 subjects into moderate/severe vs. little/no distress.) showed moderate-to-severe distress in 56 patients (61.5%) versus 35 patients (38.5%) with little-to-no distress. Patients diagnosed with MDD were three times more likely to report having higher levels of distress (i.e., moderate/extreme), compared to patients with schizophrenia or bipolar disorder (p<0.05). Compared to patients who reported little-to-no stress, patients reporting moderate-to-severe stress also reported increases in depression (p<0.01), tiredness, hopelessness, no cheer, and worthlessness (p<0.05) on the K10. Results for the K10 scale and sub-items are presented in Table 2.
Patients reporting higher levels of stress (i.e., moderate/extreme) indicated increased levels of perceived likelihood of contracting COVID-19 (p<0.05) and general concern regarding COVID-19 (p<0.01), compared to patients reporting lower levels of stress. While higher numbers of patients reporting moderate-to-severe distress consulted with a doctor or received a COVID-19 test, compared to patients reporting little-to-no distress, these differences were not significant. No other differences were found between moderate-to-severe versus little-to-no stress groups regarding COVID-19 disease knowledge, risk perception, use of precautionary measures, or healthcare utilization. A higher percentage of psychiatric patients living in Florida (86.5%) reported a worsening of psychiatric symptoms, compared to patients living in Maryland and Georgia (p<0.05), although overall psychological distress did not significantly differ between geographic locations.
Discussion
Results from our survey of 94 clinical trial subjects with SMI suggest that a significant majority of these patients are knowledgeable regarding COVID-19 disease, demonstrate awareness regarding the risk of infection, and use precautionary measures to mitigate infection risk, even while reporting increased symptoms and moderate-to-severe levels of psychological stress. In fact, patients with higher levels of psychological stress reported higher levels of concern regarding infection, were more likely to use precautionary measures and seek medical help, and were more likely to have a diagnosis of major depression. These findings are consistent with other reports of the experiences of patients with psychiatric illness during the COVID-19 pandemic.21,23,24,31
While a significant majority of patients with SMI surveyed used precautionary measures to protect against COVID-19, far fewer (<30%) used medical services or laboratory testing. While reasons for this are unclear based on our data, the findings are consistent with other reports of pandemic-associated exacerbation of medical healthcare disparities affecting the mentally ill6,15,16 and might account for the high rate of COVID-19 infection in our sample (10%). Other studies assessing the effect of the COVID-19 pandemic on individuals with a pre-existing mental illness consistently report symptom exacerbation, including higher scores of anxiety, depression, stress, and insomnia on rating scales,6,19–22 which is consistent with our findings. Possible contributing factors to this worsening of symptoms may be fear or concerns regarding contracting COVID-19, social isolation related to lockdown restrictions in place at the time of the survey, lack of access or reduction in access to healthcare services, or difficulty obtaining or adhering to psychiatric medications.6,32
The findings that a majority of patients were knowledgeable about the common symptoms and transmission of COVID-19, used precautionary measures, and understood risk mitigation using protective measures were encouraging and are consistent with two other studies of PPE use in patients with SMI conducted during the COVID-19 pandemic, which found that patients with SMI did not differ from healthy controls in the use of preventive measures.33
Limitations. The significance of these findings is limited by the cross-sectional design and lack of a control group for comparison. Other limitations include a small study sample derived by convenience sampling, thus lacking power and representability to draw extensive conclusions. Response bias might have been present, given that the survey was interviewer-administered and sensitive information was being collected. Lastly, due to differences in frequency of outpatient care and resources, our findings in clinical trial participants with SMI might not be generalizable to the majority of patients with SMI who do not participate in clinical trials.
Conclusion
Despite these limitations, our survey results provide additional evidence for robust coping abilities in patients with SMI during the COVID-19 pandemic, including knowledge of disease risk and use of precautionary measures to prevent infection; our findings also suggest that this patient population can safely participate in clinical trials and generally in the community, despite the health dangers posed by the pandemic. It is important to note that this survey was conducted during the first wave of the COVID-19 pandemic (i.e., June–September 2020), when testing for COVID-19 was relatively limited and vaccines were not publicly available. In addition to vaccination rollout, efforts have since been made for more widespread testing. Additional investigations that are longitudinal in approach, utilize appropriate control groups for comparison and valid ratings for measurement of symptoms and pandemic-related stress, and include data on laboratory testing and vaccination are warranted, as these might better distinguish between pandemic- and illness-related factors and therefore provide better therapeutic interventions to help medically and psychiatrically vulnerable patients with SMI cope during a pandemic.
References
- Beach SR, Praschan NC, Hogan C, et al. Delirium in COVID-19: a case series and exploration of potential mechanisms for central nervous system involvement. Gen Hosp Psychiatry. 2020;65:47–53.
- Chen G, Wu D, Guo W, et al. Clinical and immunological features of severe and moderate coronavirus disease 2019. J Clin Invest. 2020;130(5):2620–2629.
- Debnath M, Berk M, Maes M. Changing dynamics of psychoneuroimmunology during the COVID-19 pandemic. Brain Behav Immun Health. 2020;5:100096.
- Mao L, Wang M, Chen S, et al. Neurological manifestations of hospitalized patients with COVID-19 in Wuhan, China: a retrospective case series study. JAMA Neurol. 2020;77(6):683–690.
- Yang L, Wu W, Hou Y, et al. Analysis of psychological state and clinical psychological intervention model of patients with COVID-19. medRxiv. 2020.
- Hao F, Tan W, Jiang L, et al. Do psychiatric patients experience more psychiatric symptoms during COVID-19 pandemic and lockdown? A case-control study with service and research implications for immunopsychiatry. Brain Behav Immun. 2020;87:100–106.
- Holman A, Thompson R, Garfin D, Silver R. The unfolding COVID-19 pandemic: a probability-based, nationally representative study of mental health in the United States. Sci Adv. 2020;6(42):eabd5390
- McCracken LM, Badinlou F, Buhrman M, Brocki KC. Psychological impact of COVID-19 in the Swedish population: depression, anxiety, and insomnia and their associations to risk and vulnerability factors. Eur Psychiatry. 2020;63(1):e81.
- Muller AE, Hafstad EV, Himmels JPW, et al. The mental health impact of the COVID-19 pandemic on healthcare workers, and interventions to help them: a rapid systematic review. Psychiatry Res. 2020;293:113441.
- Vindegaard N, Benros ME. COVID-19 pandemic and mental health consequences: systematic review of the current evidence. Brain Behav Immun. 2020;89:531–542.
- Brooks SK, Webster RK, Smith LE, et al. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. Lancet. 2020;395(10227):912–920.
- Holmes EA, O’Connor RC, Perry VH, et al. Multidisciplinary research priorities for the COVID-19 pandemic: a call for action for mental health science. Lancet Psychiatry. 2020;7(6):547–560.
- Tsang HW, Scudds RJ, Chan EY. Psychosocial impact of SARS. Emerg Infect Dis. 2004;10(7):1326–1327.
- Druss BG. Addressing the COVID-19 pandemic in populations with serious mental illness. JAMA Psychiatry. 2020;77(9):891–892.
- Kozloff N, Mulsant B, Stergiopoulos V, Voineskos A. The COVID-19 global pandemic: implications for people with schizophrenia and related disorders. Schizphr Bull. 2020;46(4):752–757.
- Shinn AK, Viron M. Perspectives on the COVID-19 pandemic and individuals with serious mental illness. J Clin Psychiatry. 2020;81(3):20com13412.
- Li L, Li F, Fortunati F, Krystal JH. Association of a prior psychiatric diagnosis with mortality among hospitalized patients with coronavirus disease 2019 (COVID-19) infection. JAMA Netw Open. 2020;3(9):e2023282.
- Nemani K, Li C, Olfson M, et al. Association of psychiatric disorders with mortality among patients with COVID-19. JAMA Psychiatry. 2021;78(4):380–386.
- García-Fernández L, Romero-Ferreiro V, Padilla S, et al. The impact on mental health patients of COVID-19 outbreak in Spain. J Psychiatr Res. 2021;136:127–131.
- Neelam K, Duddu V, Anyim N, et al. Pandemics and pre-existing mental illness: a systematic review and meta-analysis. Brain Behav Immun Health. 2021;10:100177.
- Solé B, Verdolini N, Amoretti S, et al. Effects of the COVID-19 pandemic and lockdown in Spain: comparison between community controls and patients with a psychiatric disorder. Preliminary results from the BRIS-MHC STUDY. J Affect Disord. 2021 15;281:13–23.
- Sun Q, Qin Q, Basta M, et al. Psychological reactions and insomnia in adults with mental health disorders during the COVID-19 outbreak. BMC Psychiatry. 2021;21:19.
- Hölzle P, Aly L, Frank W, et al. COVID-19 distresses the depressed while schizophrenic patients are unimpressed: a study on psychiatric inpatients. Psychiatry Res. 2020;291:113175.
- Vissink CE, Van Hell HH, Galenkamp N, van Rossum IW. The effects of the COVID-19 outbreak and measures in patients with a pre-existing psychiatric diagnosis: a cross-sectional study. J Affect Disord Rep. 2021;4:100102.
- Kessler RC, Andrews G, Colpe LJ, et al. Short screening scales to monitor population prevalences and trends in non-specific psychological distress. Psychol Med. 2002;32(6):959–976.
- Maguire PA, Reay RE, Looi JC. A sense of dread: affect and risk perception in people with schizophrenia during an influenza pandemic. Australas Psychiatry. 2019;27(5):450–455.
- Wang C, Pan R, Wan X, et al. Immediate psychological responses and associated factors during the initial stage of the 2019 coronavirus disease (COVID-19) epidemic among the general population in China. Int J Environ Res Public Health. 2020;17(5):1729.
- Andrews G, Slade T. Interpreting scores on the kessler psychological distress scale (K10). Aust N Z J Public Health. 2001;25(6):494–497.
- Centers for Disease Control and Prevention. Symptoms of COVID-19. Updated 22 Feb 2021. https://www.cdc.gov/coronavirus/2019-ncov/symptoms-testing/symptoms.html. Accessed 28 Oct 2021.
- Crane MA, Shermock KM, Omer SB, Romley JA. Change in reported adherence to nonpharmaceutical interventions during the COVID-19 pandemic, April-November 2020. JAMA. 2021;325(9):883–885.
- Maneepongpermpoon P, Pitanupong J. Knowledge, risk perception, precautionary behavior and level of worry towards the 2019 coronavirus disease (COVID-19) among psychiatric outpatients. Siriraj Med J. 2020;73(1):1–9.
- Khanra S, Sahoo RR, Bose S, et al. Impact of lockdown and health anxiety during COVID 19 pandemic among inpatients of a psychiatric hospital: an observational study. Asian J Psychiatr. 2020;293:113429.
- Pinkham AE, Ackerman RA, Depp CA, et al. COVID-19-related psychological distress and engagement in preventative behaviors among individuals with severe mental illnesses. NPJ Schizophr. 2020;7:7.
