
by Nita Bhatt MD, MPH; Jesse Cannella, MSIII; and Julie P. Gentile, MD, MBA
Dr. Bhatt is Associate Director of Medical Student Education and Associate Professor in the Department of Psychiatry at Wright State University in Dayton, Ohio. Mr. Cannella is a medical student at Wright State University Boonshoft School of Medicine in Dayton, Ohio. Dr. Gentile is Professor and Chair of the Department of Psychiatry at Wright State University in Dayton, Ohio.
Funding: No funding was provided for this study.
Disclosures: The authors have no conflicts of interest relevant to the content of this article.
Innov Clin Neurosci. 2022;19(4–6):23–32.
Department Editor
Julie P. Gentile, MD, is Professor and Chair of the Department of Psychiatry at Wright State University in Dayton, Ohio.
Editor’s Note
The patient cases presented in Psychotherapy Rounds are composite cases written to illustrate certain diagnostic characteristics and to instruct on treatment techniques. The composite cases are not real patients in treatment. Any resemblance to a real patient is purely coincidental.
Abstract
Lesbian, gay, bisexual, transgender, queer/questioning, intersex, asexual, plus (LGBTQIA+ or LGBTQ+) individuals face a wide array of health disparities both within and separate from the healthcare system. Transgender patients are subject to microaggressions, misgendering, and harassment from providers, medical staff, and fellow patients. These patients experience drastic disparities in suicidality, depression, anxiety, substance use, malignancy, sexually transmitted disease (STD), and victimization of violence. Providers have the opportunity to intervene and positively impact patient experiences through gender-affirming care, but they first require an adequate knowledge base and understanding of the importance of sensitive and inclusive care. Seemingly small interventions, such as listing one’s own pronouns, using gender-neutral language, validating and affirming patients, and utilizing appropriate mental and physical health screenings, can lead to significant impacts on the patient experience, health outcomes, and quality of life. This article will discuss some of the most common disparities and obstacles faced by transgender patients and will argue the paramount role of the provider in establishing gender-affirming care and some high-impact avenues that the provider, regardless of specialty, may pursue when caring for these patients.
Keywords: Transgender, trans, gender minority, gender-affirming, gender-affirming care, LGBTQ+, health disparities, inclusive care
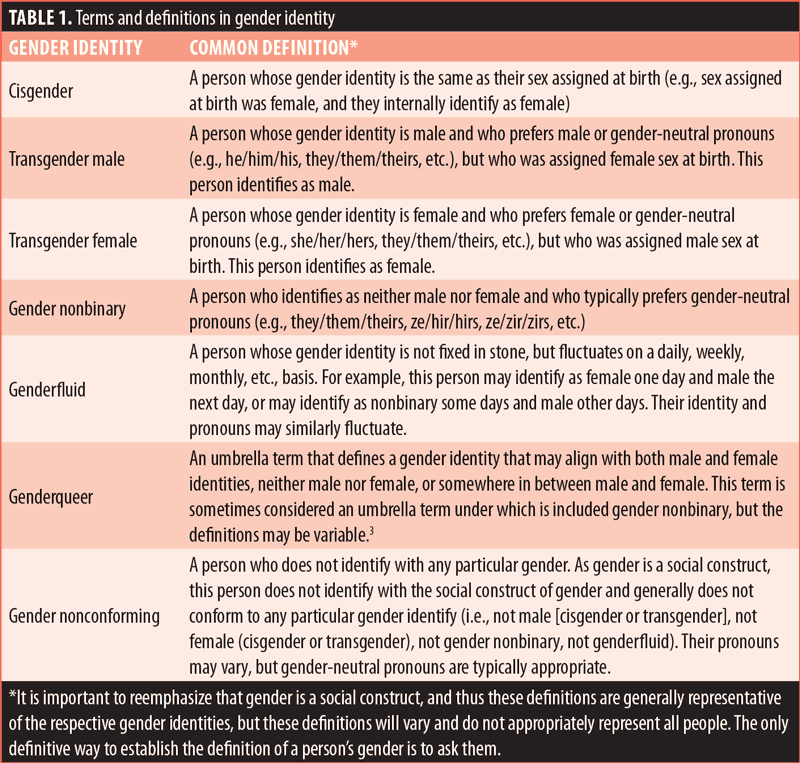
It has been well established that gender is a social construct, not an inborn reality of biology, nor is it binary. This is contrasted with sex, which is generally defined as the biological characteristics (i.e., reproductive, chromosomal, hormonal) of a person established at birth, and is in fact also nonbinary, although it is most often characterized as male or female. Even after “checking under the diaper” and with karyotyping, the sex defined at birth may be established as male or female, but it also may be established as intersex or be within other nonbinary variations.1 Gender, however, is a social construct that may be cisgender male or female, but individuals may alternatively be identified as nonbinary, genderfluid, genderqueer, or transgender male or female, among other identities (Table 1). Indeed, the binary construct of gender is one of Western context and is not absolute.2
Fundamentally, it must be emphasized that the gender of a person cannot be externally read or assumed. Gender identity is an internal self-identity and may or may not correspond to how a person dresses, how a person grooms their hair or facial hair, what a person calls themselves, or how they speak. How a person externally represents themselves, such as through apparel, hair style, voice, or behavior, is known as their gender expression.4 For various reasons, including but not limited to comfort, safety, self-realization, laws, institutional guidelines, and conformity to social norms, the gender expression of a person may not necessarily correlate to their gender identity. For this reason, the only way to know the gender of a person is by asking them, and even when asked, gender and gender identity is subject to change and is not necessarily a permanent quality.
This article discusses some of the most significant health disparities faced by transgender patients, common challenges they experience, and how providers, regardless of specialty, can positively intervene to better provide an inclusive environment with gender-affirming care.
Health Disparities in LGBTQ+ Patients
Lesbian, gay, bisexual, transgender, queer/questioning, intersex, asexual, plus (LGBTQIA+ or LGBTQ+) patients experience dramatic disparities in healthcare and health outcomes, even experiencing greater incidence of cancer.5 Specifically, transgender individuals face even greater challenges and disparities due to confounding factors of societal norms, institutionalized discrimination, individual prejudice, violence, abuse, and transphobia. Transphobia can be explained as the belief that gender and sex are binary, and thus that the transgender identity is a medical pathology. When assessing provider knowledge of transgender healthcare, a multivariable linear regression study found that transphobia was the only variable predicting knowledge level regarding transgender care. Even increased learning time spent on transgender healthcare was not shown to increase a provider’s competence when transphobia was first evident.6 Indeed, studies show that up to 70 percent of gender minority adults, in addition to 56 percent of sexual minority adults, self-report a history of discrimination from health providers. Furthermore, approximately eight percent of sexual minorities and 25 percent of transgender people report a history of being denied healthcare services from providers.7
Social services are likewise lacking for these patients. A 2015 survey showed that 24 percent of transgender Americans reported transgender-related housing discrimination within the prior year, and 30 percent reported transgender-related employment discrimination. Rates were greater still among transgender people of color.8 A cross-sectional data analysis found positive correlations among transgender women in Chicago and Los Angeles between two variables, intimate partner violence (IPV) and polysubstance use, with two outcomes, human immunodeficiency virus (HIV) positivity and condomless anal intercourse, as well as correlations with sex work and incarceration.8 These variables are potentially preventable with public health efforts, however, and thus outcomes of HIV incidence, sex work, and incarceration are as well. Wesp et al8 suggest that public health should focus on prioritizing housing access for this community, along with adequate education and employment opportunities, with a focus on upstream medicine. Indeed, multiple studies support that transgender women with adequate health insurance and stable housing have lower-risk behaviors with improved health outcomes.9 However, the 2016 National Transgender Discrimination Survey found that 19 percent of transgender individuals did not have health insurance, more than the general American population. Providers and social workers should thus prioritize these issues.10
Fictional Case Vignette 1
Alex C. was an 18-year-old transgender male patient who presented to his family doctor for his annual physical and to receive his meningitis vaccine for college. Alex missed his past three physicals and had not seen a medical provider since the age of 14 years. Alex had a past medical history of asthma, eczema, and generalized anxiety disorder, which were all currently untreated. Alex was not currently on any medications except for a daily men’s vitamin. Alex reported no complaints or medical concerns at presentation and only desired the completion of his physical form for school, as well as his vaccine.
Based on the physical exam, Alex was a healthy-appearing adolescent male, pleasant, and cooperative. Oral exam was significant for obvious decay of his left incisor with apparent gum necrosis, extremely tender to palpation. Genital exam was deferred.
Alex was given vaccines for meningitis A (MenA), meningitis B (MenB), and human papillomavirus (HPV) and was prescribed acetaminophen for dental pain, with a recommendation for close follow-up with a dentist. A follow-up physical was scheduled for one year.
Alex never presented to his dentist and did not return for his one-year follow-up.
Practice Point: Addressing Appropriate Screening and Preventative Healthcare in Transgender Patients
Appropriate screening and preventative healthcare are frequently missed in transgender patients due to oversight or ignorance in the position of the provider, discomfort or avoidance in the position of the patient, insurance denial, institutionalized and systemic discrimination, or a combination thereof. The literature shows increasingly evident reductions in the use of primary care services for transgender patients. Standardized preventative care, such as HIV screenings, are recommended annually for high-risk groups per United States (US) Centers for Disease Control and Prevention (CDC) guidelines, yet a Massachusetts survey from 2007 to 2009 found that only 16.8 percent of transgender respondents reported an HIV test within the prior year.10,11 Likewise, the American Heart Association (AHA) recommends that all adults age 20 years or older receive at least biannual cholesterol screening; a 2014 chart review study showed that transgender women receiving hormone therapy were found to have higher triglyceride levels than their cisgender peers, emphasizing the importance to at least maintain these biannual evaluations, yet these patients often did not meet recommended guidelines for screening.10 Any transgender female patient, regardless of hormone therapy or gender-affirming surgery in the absence of complete prostatectomy, should continue to receive prostate exams corresponding to the recommended guidelines for cisgender male patients, according to both the World Professional Association for Transgender Health and the Endocrine Society. Caution should be made when evaluating prostate-specific antigen (PSA) levels, however, as a level of 1ng/mL may be an accurate proxy for the upper limit of normal.12 Likewise, any transgender male patient, regardless of hormone therapy or gender-affirming surgery, in the absence of a complete mastectomy removing all breast tissue, should continue to receive age-appropriate breast exams and mammograms; any patient with a cervix should similarly continue to receive age-appropriate pap smears and pelvic exams. A New England study, however, found that only 31 percent of transgender men who have sex with cisgender men had received a pap smear within the past year.10 That being said, it is essential to emphasize the sensitivity required when inquiring about and performing these screenings and encounters. These are often uncomfortable and undesirable exams, even for cisgender patients, and these feelings of discomfort are only heightened in transgender and nonbinary patients, who may be required to advocate on their own behalf and educate their providers, may be subject to misgendering and discrimination, and have most likely already experienced negative encounters with healthcare providers. Less invasive options, such as self-swab pilot studies, have shown similar efficacy to pap smears for transgender men, while minimizing trauma and gender dysphoria.5
It is important to note that due to both behavioral and socioeconomic factors, sexual health differs for LGBTQ+ patients, and appropriate screenings should thus respectively differ. Lesbian and bisexual women experience higher rates of bacterial vaginosis. Men who have sex with men (MSM) and transgender women have higher rates of sexually transmitted diseases (STDs), including HIV, hepatitis C, gonorrhea, and syphilis. When screening or testing for these diseases, the individual’s sexual behaviors should be considered, and swabs, when appropriate, should be used in respective anal, urethral, and/or vaginal orifices, as applicable; vaginal-penile sex should never be assumed.5 In fact, worldwide, transgender women experience a higher prevalence of HIV than any other group. Rates in the US are higher still among Black transgender women.8 High-quality, easily accessible, and LGBTQ+-sensitive and -relevant sexual education and information is quintessential. Due to inconsistencies in provider expertise and sensitive care, all providers thus hold the responsibility of ensuring appropriate education for these patients. Furthermore, preventative medicine and risk reduction measures have been shown to benefit MSM, transgender men, and transgender women by offering HPV vaccination, pre- and postexposure HIV prophylaxis, and regular assessments for hepatitis A and B.5
While differences in sexual behaviors are obvious in this population, health disparities exist across a vast continuum. Although pharmacokinetic effects of hormone therapy compound this statistic, when compared with cisgender women, transgender women experience higher incidences of venous thromboembolisms, cerebrovascular accidents, myocardial infarction, and overall cardiovascular mortality.7 Indeed, even cancer rates are increased among LGBTQ+ adults.5
Furthermore, increased rates of IPV and physical and sexual abuse in this population may additionally trigger posttraumatic stress disorder (PTSD) or secondary trauma.13 Tragically, mortality from violence is significant among this population, particularly in further intersectionalities. Some studies estimate that up to 93 percent of transgender homicide victims in the US are Black or Latinx transgender women. Their homicide rates are even higher than cisgender Black and Latina women, even though they represent a smaller population.8 Trauma-informed care and sensitive exams should thus be a pillar of treatment for all patients, but especially for this population. A provider should always ask the patient’s consent before placing hands on the patient or before beginning a physical exam; the reasons for the exam should similarly be established and explained. The sensitive affect and demeanor of the provider is likewise essential in establishing comfort and mitigating stigma; a provider who is judgmental, uncomfortable, or uncertain how to proceed with an exam or interview will only make the patient more uncomfortable and inhibit rapport.14
Fictional Case Vignette 2
Xi M. was a 22-year-old transgender female patient who used they/them/their pronouns and presented to their outpatient psychiatrist for “feeling down” for the past six weeks. They reported feeling sad and hopeless, with decreased sleep and weight loss of 12 pounds over the past two months. They reported feeling “like there’s nothing to live for.”
Xi admitted to a history of cutting their wrists and one prior suicide attempt (SA) two years prior (attempting to jump off a bridge) that was stopped by police. They recently purchased a pistol and “have been thinking about using it, so that I can get away from everything” and “just be free.”
On further interview, it was revealed that Xi was recently evicted from their apartment because of a new landlord who “didn’t want people like me living there.” They worked part-time at a gas station; they previously worked at a bakery for six years but were fired the previous year when they came out to the owner as transgender. Upon presentation, Xi indicated they were uninsured but were applying for Medicaid, and that they were currently “crashing on a friend’s couch.” Prior to their last apartment, they lived with their parents, but were “kicked out” on their 18th birthday.
Xi admitted to nine years of tobacco use (current use one pack per day) and moderate alcohol use of 2 to 3 drinks per night. They also admitted to daily marijuana use and occasional cocaine use for the past three years. Xi reported that their closest friend died of a heroin overdose two months previously, “but I would never do that stuff.”
Xi had no medical history besides gender dysphoria and reported that they “tried to start hormone therapy, but my doctor said it would give me blood clots and breast cancer.” Xi still desired hormone therapy but was scared of these effects. Xi had never undergone gender-affirmation surgery but reported that “my [primary care] doctor still tells me that I should be seeing an OB/GYN for this stuff though.”
Xi was pink-slipped and admitted to inpatient psychiatry with suicide precautions. After two weeks of inpatient rehabilitation, Xi was started on outpatient fluoxetine and hormone therapy and referred to an outpatient therapist. At one-month psychiatry follow-up, Xi reported a “better mood” and still transient but greatly reduced suicidal ideation (SI). They reported “feeling better about myself and about how I look,” continuing to attend weekly therapy with bimonthly psychiatry follow-up and having joined an LGBTQ+ support group.
Three years later, Xi continued to attend therapy, but discontinued the fluoxetine, saying that they felt “a lot better;” “I finally feel like I look on the outside like who I am on the inside.” Xi also reported that they “started seeing someone” and that it was “going very well.”
Practice Point: Addressing Mental Health Issues in Transgender Patients
Not only do transgender patients experience greater rates of preventable disease, communicable disease, and discrimination and discomfort in public health and healthcare, but it is also well documented that transgender patients experience radically increased rates of substance use disorders, tobacco use, major depression, suicidality, and other psychiatric diseases.5 The literature likewise shows that American transgender people experience higher rates of suicide attempts (SAs) and substance use than cisgender people, higher still among transgender people of color or those with disabilities.8
While gender dysphoria is a diagnosis under the Diagnostic and Statistical Manual of Mental Disorders-5 (DSM-5), briefly defined as incongruence in gender identity and assigned sex causing significant impairment and distress, it is important to note that gender dysphoria is not synonymous with being transgender.4 Not all transgender patients actively experience gender dysphoria, and not all patients with gender dysphoria identify as transgender. Unfortunately, however, many treatment options, such as gender-affirming surgery and hormone therapy, are sometimes only accessible for patients if they have this DSM-5 diagnosis.8
Substance use disorders originate from biopsychosocial etiologies and often begin as coping mechanisms or self-treatment for abuse or psychiatric illness.13 Transphobia and homophobia lead to chronic stressors and stigma playing into the minority stress model; this frequently progresses to coping mechanisms becoming increasingly maladaptive, often resulting in high-risk substance use and sexual behavior.5 Indeed, a 2009 study of transgender women in New York City found that one out of two participants reported present tobacco use, while a 2015 San Francisco study found that 83 percent of transgender women reported cigarette use within the last 31 days. Similarly, a Virginia study of 350 transgender participants found that 64 percent self-reported using tobacco during their life, with 23 percent reporting a lifetime tobacco use problem.10 However, motivational interviewing, substance use counseling, and treatment of comorbidities have the potential to combat these disparities.
Disparities throughout the spectrum of mental health have been found in transgender patients. Transgender men have been found to have increased prevalence of depression, anxiety, somatic symptom disorder, and suicide completion.12 High rates of real or threatened IPV; physical, emotional, and sexual abuse from family members; and homelessness; high population prevalence of suicide, homicide, and accidental overdose; and the lifelong influences of the minority stress model all play into PTSD, prevalent in the transgender population.13,14 Research suggests that trauma-informed care, with a focus on empowerment and emotional regulation, has been shown to reduce social withdrawal for trauma survivors. Furthermore, a trusting and effective provider-patient relationship, formal or informal psychotherapy and cognitive-behavioral therapy (CBT), and affirmative care are effective in reducing symptoms of anxiety, depression, and hypervigilance and further foster patient agency with improved long-term physical and mental health.14
The literature shows that the COVID-19 pandemic has further exaggerated mental health symptoms for many individuals, in particular for transgender people. The LGBT Foundation reported that 38 percent of transgender people aged 50 years or older were currently living alone in 2020, with 29 percent desiring decreased isolation.15 In the same year, a Columbia University survey of 6,200 individuals found that 86 percent of people reported increased anxiety, 75 percent reported vicarious trauma, 74 percent reported a sense of helplessness, and 29 percent reported dark and negative thoughts as a result of the COVID-19 pandemic. Twenty-seven percent of those people reported experiencing anxiety for the first time, and 20 percent reported depression for the first time during this period. The pandemic may thus have increased isolation and corresponded with increased symptoms of cognitive and emotional disorders and worsening mental health symptoms.15 In times of medical pandemics, mental and psychiatric issues should not be overlooked, but rather should be given extra care and consideration.
The most feared health outcome of psychiatric illness is SI or SA. Unfortunately, both SI and SA are associated with greater risk stratification in the transgender community. Indeed, a study of 6,450 transgender and gender-nonconforming people found that 41 percent self-reported a history of SA, a statistic 27 times that of the general public.12 A study by Zwickl et al16 in Australia similarly showed that over 40 percent of transgender Australian adults self-reported a history of SA, which was 10 times that of the general public, despite nationwide antidiscrimination laws. While these statistics are disheartening and tragic, they are preventable. Increased odds of SA were positively associated with comorbid depression, victimization of physical assault, unemployment, a desire for gender-affirmation surgery, and institutionalized cis-sexism. Unemployment alone was shown to confer a 55-percent greater odds of SA in transgender individuals; self-reported depression represented a 300-percent greater odds of SA. Zwickl et al16 thus concluded that addressing factors of gender-affirming treatment access, discrimination, and assault be paramount priorities of transgender healthcare. The authors suggest that resilience-focused, strength-based approaches and positive psychotherapy are necessary shifts in healthcare for these patients to best minimize SI and SA and promote the best health outcomes.16
Fictional Case Vignette 3
Jamie H. was a 54-year-old transgender male patient who presented to a Women’s Health Clinic for pain when urinating. Upon arrival at the clinic, Jamie spoke to the nurse at registration to say that he was there for his appointment. The nurse was unable to find Jamie’s information in the system and asked to look up his phone number. When looking up the given phone number, the nurse only found the name “Katelyn L.” Jamie uncomfortably reassured the nurse that they are the same person, but that he preferred the name Jamie. The nurse asked for Jamie’s license for verification. His license had the name Jamie H. instead of Katelyn L., and the nurse was unsure how to proceed since the identification did not meet the clinic records. The nurse asked for Jamie’s real license, which Jamie insisted that this was. After discussing with the nursing supervisor, the nurse ultimately accepted this identification but did not make any notes or addendums in the patient record.
Jamie filled out his intake form. Demographic options only included “race: White; African American; Latino/Latina” and “sex: M/F.” Jamie listed “White,” “M.” The intake forms for the Women’s Health Clinic consistently used female pronouns, much to Jamie’s discomfort. Jamie returned his paperwork to the nurse and waited in the waiting room.
Jamie’s name was called by a different nurse, and Jamie walked over to the nurse.
Nurse C: Is your wife in the bathroom?
Jamie: No… I’m here alone.
Nurse C: But this is the women’s health clinic.
Jamie: Yes…I know.
Nurse C looked confused but walked Jamie into the back and took Jamie’s vitals. Nurse C then walked Jamie to Room 3 and asked Jamie why he was there.
Jamie: It’s been burning when I go to the bathroom.
After a few more questions, Nurse C walked Jamie to the restroom to get a urine sample.
Jamie: This is the women’s restroom. Is there another restroom I can use?
Nurse C: Well, this is the women’s health clinic. This is the only restroom where we have the window for urine samples. If you wanted to come to the women’s health clinic, you can use the women’s bathroom.
Jamie uncomfortably went into the women’s restroom and got a urine sample. Jamie walked back to Room 3, and sometime later, Dr. J arrived. Dr. J did not introduce herself and quickly took a history of present illness (HPI). Dr. J did not ask for a menstrual history or sexual history. Dr. J listened to Jamie’s heart and lungs but did not offer to do a genital exam or speculum exam. The patient had not received a pap smear in the past six years and was not offered one. The patient had never undergone a mammogram and was not offered one.
Jamie was prescribed three days of sulfamethoxazole/trimethoprim 160mg by mouth and told to return to the clinic if symptoms worsened. Five days later, Jamie continued to have dysuria and dyspareunia, but did not return to clinic, hoping that it would “solve itself.”
Three weeks later, Jamie got a bill from the clinic for the entire cost of the visit. His visit was apparently not authenticated by insurance because the name records at the clinic did not match his insurance records.
Practice Point: Providing Gender-affirming Care
From the second that a transgender patient calls to schedule an appointment with their healthcare provider, they are subject to potentially receiving noninclusive care and revisiting trauma.
Providing gender-affirming care begins with the first encounter of a patient with a provider’s waiting room, phoneline, or website. Cisnormativity, the assumption that being cisgender is the norm and expectation, whereas being transgender is “abnormal,” leads to erasure and invisibility of the transgender experience and transgender identity. A 2016 systematic review, however, found that the prevalence of self-reported transgender identity is actually as high as 0.1 to 0.7 percent.17 Far too often, registration and intake forms or medical interviewing provides only gender-binary options. Worse still, these forms frequently mistake sex for gender, prepopulate or assume these qualities, and include no mention or opportunity to list pronouns. Inclusive and gender-affirming care necessitates gender-inclusive and gender-neutral options on intake forms and in registration. Along with “name,” these forms should include options for “preferred name.” Similarly, gender should be included on these forms, and if “sex assigned at birth” is an additional box, it should not replace gender, but should be included in addition. Options for gender should either be a fill-in-the blank response or should include options outside of the binary, optimally including transgender male, transgender female, gender nonbinary, gender fluid, and other.17 Furthermore, gender-neutral terms should be utilized whenever available; for example, many individuals prefer the term “Latinx” to “Latino” or “Latina,” as it is a gender-neutral variation of the word. Intake forms that ask about ethnic demographics can specify “Hispanic and Latinx” or “Hispanic and Latina/Latino/Latinx” in place of the more standard and more binary “Latino/Latina” option.18
Countertransference is an important aspect of minority and gender-affirming care. In short, countertransference refers to a provider’s conscious and unconscious reactions to a patient and can lead to significant obstacles in the therapeutic relationship. A provider who is uncomfortable with their patient will only make their patient more uncomfortable. Self-awareness can be a powerful tool in combatting the potentially problematic effects of countertransference.19 Providers are not expected to have a complete understanding of every identity or minority but should feel comfortable learning more about these identities and should not allow their incomplete understanding to impede them in providing high-quality care. Mistakes and incorrect language are inevitable but should be followed with an apology, rather than avoidance or greater discomfort, and should then be followed by moving on with a continued encounter. These subjects should not be avoided or ignored but also should not prevent the provider from building rapport or properly caring for a patient.
An inclusive and gender-affirming healthcare atmosphere necessitates appropriate and inclusive education for all staff and employees, not only for healthcare providers or physicians. Gender-neutral language should be encouraged and printed, and gender-neutral restrooms should be clearly available and easily accessible. Diversity and inclusion statements or nondiscrimination statements should be clearly posted in the lobby or waiting room, and inclusive or minority logos, such as the pride flag or transgender flag or colors, can further encourage comfort and establish inclusive care. The literature supports that gender-neutral language should also be utilized whenever possible. Seemingly minor adjustments, such as changing the names of women’s health centers to obstetrics and gynecology or mother and child units to labor and delivery, can create more inclusive environments, as people who are not women receive gynecological evaluations and people who are not mothers go through labor and delivery. Sensitive techniques, such as the use of pediatric speculums in transgender women and when examining neovaginas, likewise help to make exams more comfortable.17
Physicians and providers should feel comfortable stating their own pronouns and should directly state them when introducing themselves to patients, as well as directly ask patients to share theirs, for example, saying, “Hello, my name is Dr. Smith. I use she/her/hers pronouns. How may I help you today?” Pronouns should similarly be included on intake forms. This helps create an inclusive environment and encourages patients to share their own pronouns, especially in scenarios where patients are less comfortable with their pronouns or may have previously felt uncomfortable or unsafe sharing them. Providers can also nonverbally establish this comfort and rapport by wearing badges or lapel pins with their pronouns or with the pride flag or transgender flag. Healthcare professionals should also be encouraged to list their pronouns in their email signatures and in professional or casual communication with patients or other medical personnel.20
Fictional Case Vignette 4
Lily M. was a 14-year-old transgender female patient who presented to the children’s hospital for insufficient weight gain, with a past medical history of major depression and gender dysphoria and past surgical history of right-sided myringotomy. Lily’s parents were concerned because they felt that Lily was “extremely underweight.” Lily believed that she was not underweight and, in fact, believed that she was “still too fat.” Lily was diagnosed with severe malnutrition and anorexia nervosa. Lily was admitted as an inpatient and placed on nightly nasal-gastric feeds. An inpatient gastroenterologist was consulted.
Dr. R, a third-year resident, was careful to use Lily’s correct pronouns and was insistent that Dr. R’s intern and medical student did as well. The patient care assistant, however, smiled at Lily and called her “a very pretty boy,” consistently using male pronouns and refusing to use Lily’s name.
The hospital electronic medical record did not allow for name or gender changes, so Lily’s chart continued to be under the name of “Andrew M.” and listed Lily as a male, with all templates auto-populating to “Andrew M, a 14 y.o. boy….” Although there was a separate tab for sexual orientation, gender identity, and gender expression (SOGIE) information, it was not readily accessible.
Dr. R made a point to include a note in Lily’s electronic chart stating her preferred name and pronouns. Dr. R manually changed all of the auto-populated information in her notes to use Lily’s correct name and gender.
Upon full history and physical exam, Lily also admitted to continuous SI, with a history of four SAs, all by overdose. Lily denied current SI or plan but admitted to “sometimes thinking about doing it.” Lily denied access to firearms or lethal means and reported feeling safe at home. Lily reported that her parents were supportive of her gender identity and used her preferred name, but that her teachers and school administration did not, and that she had “no friends.” Lily was prescribed sertraline hydrochloride 25mg daily, and inpatient psychiatry was consulted. Lily was placed on suicide precautions.
After visiting Lily, Dr. R and her team then made their rounds to their 11 other patients. When running the list after rounds, Dr. R unintentionally said “Andrew M.” when referring to Lily, because that was the name printed on her patient list.
Practice Point: Transgender Patients in Pediatrics
Pediatric and adolescent transgender patients are subject to additional and unique challenges. Caring for these patients requires added considerations. Does the patient understand the terminology which they themself or the provider uses? Does the patient understand the spectrum of gender identity? Is this the patient’s first experience ever discussing or considering these subjects? Does the patient feel safe or comfortable with these identities in light of their families, education, or social environment?
Gender identity is not necessarily a fixed quality but rather is subject to fluctuation. Gender exploration is thus a normal facet of social development. This does not, however, suggest that a child or adolescent who identifies as a specific gender is merely exploring these identities, but rather, that they may have already begun to establish their identity. Nearly all cisgender children will begin to identify with their assigned sex by three years of age, with corresponding gender expression based on their playmates, toys, and clothing.21 Research supports that development of gender identity in most individuals, whether cisgender or transgender, becomes noticeable and stable between the ages of three and eight years old.22 The question of when gender identification becomes permanent and when hormone therapy or gender-affirming surgery should begin remains controversial, however. Research tends to support beginning hormone therapy or puberty blockers in transgender youth if the child or adolescent themself desires it. Ethicist Florence Ashley suggests that gender exploration does not necessarily precede gender transition or identification, but rather that the processes are inevitably intertwined and concurrent. Ashley concludes that the provider’s role should be one of support, and that hormone therapy and puberty blockers thus should not be withheld, even in younger individuals, if they themselves desire such therapy.23
While normal development corresponds with gender exploration and establishing a gender identity, abnormal psychosocial development also consists of an interplay with these issues. Recent research finds that gender dysphoria may have a relationship with autism spectrum disorder (ASD). An Amsterdam study of 204 pediatric patients found an ASD prevalence of 10 percent among transgender female patients and a four percent prevalence among transgender male patients, greater than the one percent prevalence among the general public.22 The basis for this prevalence and its relevance is unclear, although it has been hypothesized that this may represent the role of gender identity as a social construct. Individuals with autism may more readily express their gender identity as a gender minority due to weaker constraints of social norms and sociocultural gender roles. Alternatively, gender dissatisfaction among individuals with autism may be further highlighted in this group due to differing coping mechanisms and comorbid stressors. Regardless, the literature suggests that the best role of the provider for this group continues to be one of support and validation.24
A 2018 cohort study by Becerra-Culqui et al22 found increased prevalence of anxiety, depression, and attention-deficit hyperactivity disorder (ADHD) among gender minority children under the age of nine years. A study in Los Angeles found that 35 percent of transgender youth had depressive symptoms and that greater than one in two experienced SI. The research indicates, however, that transgender and gender minority children who receive meaningful gender identity support may not be prone to the increased prevalence of anxiety and depression.22 Meta-analyses suggest that, compared to their peers, LGBTQ+ youth have 123- to 623-percent greater odds of using substances during their lifetime, 82- to 317-percent greater odds of experiencing mental health diseases, and 20- to 280-percent greater odds of being victim to violence. Meanwhile, gender minority youth, specifically, compared to cisgender youth, have 42- to 80-percent greater odds of using substances during their lifetime, 90- to 350-percent greater odds of being victim to violence, and a significant 470- to 1,130-percent greater odds of experiencing symptoms of depression and suicidality. Bullying likewise remains a major challenge for transgender youth. Antibullying laws have been positively associated with reduced rates of bullying victimization.25
Delaying puberty in transgender-identifying patients has been hypothesized to minimize symptoms of gender dysphoria by impeding the distress related to the phenotypic changes associated with secondary sexual development. Many providers will thus prescribe hormone blockers at the onset of puberty (i.e., the development of Tanner Stage 2 characteristics). Although age cutoffs are not defined, hormone blocker monotherapy is often stopped after the age of 14 years due to concerns about bone density. Many transgender adolescents even undergo gender-affirming surgery, such as mastectomy, prior to the age of 18 years; outcomes were likewise positive, with median findings at a two-year follow-up with scores for gender dysphoria commensurate to their cisgender peer controls. Gender-affirming surgery is irreversible and should not be casually pursued, but research suggests that it is appropriate for adolescents when they and their families are fully informed of risks and benefits and desire such treatment.26 Indeed, a 2018 survey study of postsurgical transgender male minors who had undergone chest reconstruction surgery found extremely low self-reported rates of regret and minimal adverse effects.27
It is a great travesty that rates of SI and SAs are heightened in this population. One of the greatest protective factors, however, is a gender-affirming support system. While parents and family are ideally part of this affirming support system, that is not always the case. Healthcare providers and healthcare staff often offer the opportunity to provide this support in proxy. Indeed, even a single positive encounter with a healthcare provider while discussing gender identity has the potential to act as a source of support otherwise inaccessible to many patients. Positive interventions exist across a number of dimensions and range from individual interactions to institutional policies, but should include peer support, defining coping strategies, affirmative school environments and curriculum, and inclusive policymaking.25 Indeed, the literature suggests that one of the greatest opportunities for provider intervention in rural areas or places with limited resources is in the role of advocacy, to better ensure affirmative school environments with access to gender-neutral restrooms and locker rooms, usage of preferred names, and usage of preferred pronouns.28 Internet-based resources and online support groups can further extend accessibility to these highly vulnerable individuals.25
Interventions and Treatment Options in Transgender Patients
While not all providers of all specialties will provide hormone therapy or gender-affirming surgery during their careers, all providers should be aware of these treatment options. Providers should also be aware that not all transgender patients actually undergo hormone therapy and very few actually undergo full gender-affirming surgery. As previously mentioned, gender identity does not necessarily correlate to gender expression or outward appearance, and thus not all transgender individuals dress in correspondence to their respective gender identity, let alone undergo medical treatment or surgery that corresponds to their gender identity. For reasons similar to those affecting gender expression, this may be related to a wide variety of reasons, including but not limited to cost, insurance, access to medical treatment, medical literacy, societal or institutional requirements or guidelines, feelings of safety or comfort, or simply because they do not want this treatment.4
Hormone therapy describes the use of either steroid agonists, steroid antagonists, and/or gonadotropin therapy to “masculinize” or “feminize” a patient (i.e., agonize or antagonize the effects of androgens or estrogens). Hormone therapy has been used since the 1930s and is approved both pre- and post-puberty. Adverse effects are variable, based on the specific medication, but include varying expenses, metabolic effects, electrolyte effects, renal effects, and effects on bone density, with possible cardiac effects.29 Structural inequities, refusal by providers, economic barriers, and nonaccess to hormone therapy has led many transgender individuals to pursue treatments through the internet or black market, as well as by nonmedical means, such as cement glue, automobile fluid, and industrial silicone. The dangers and adverse effects of this misuse and nonmedical or non-provider-mediated therapies are vast and include anaphylaxis, thrombosis, pulmonary hemorrhage, amputation, pneumonitis, and even death. Misuse of hormone therapy is further associated with increased rates of sex work as a means of financing treatment.9 One study in the United Kingdom found that 50 percent of gender identity clinic users had previously received hormone therapy through internet services and 28 percent received this therapy without medical evaluation or advice.30 Interventions for these high-risk transgender patients with lower socioeconomic status should thus focus on access to services, appropriate health education, and insurance and financial services.9
Gender-affirmation surgery generally describes urologic, gynecologic, or plastic surgery intended to change a person’s anatomy to better match their gender identity and to improve patient quality of life or reduce symptoms of gender dysphoria. Patients often refer to these surgeries as top surgery (e.g., mastectomy, breast reductions, breast implants) or bottom surgery (e.g., hysterectomy, vaginoplasty, phalloplasty). Gender-affirmation surgery has been performed since 1931 and is shown to increase quality of life in transgender patients, with 91 percent of transgender female patients reporting improved quality of life after vaginoplasty. These surgeries have likewise been correlated with reduced rates of gender dysphoria and reduced rates of depression and suicidality. As many as 67 percent of transgender women who first undergo hormone therapy ultimately undergo surgical breast augmentation (i.e., top surgery) via implants or fat grafting. Complications have been shown to have no significant difference, compared to cisgender controls, and benefits have been associated with satisfaction, psychological wellbeing, and sexual wellbeing. Male-to-female bottom surgery is generally performed via penile-inversion vaginoplasty, or, less commonly, via intestinal vaginoplasty, creating a neovagina. Patient satisfaction is as high as 80 percent with penile-inversion vaginoplasty, but complications may include sexual dysfunction, colon injury, fistulation, or stenosis. The most common risk of female-to-male top surgery (i.e., mastectomy or chest masculinization) is hematoma; unplanned repeat operations carry a rate of 3.2 percent. Female-to-male bottom surgery is far less common and is undergone by fewer than five percent of transgender men. Metoidioplasty and phalloplasty use existing genital tissue and peripheral tissue, respectively, to construct a phallus. Reported satisfaction averages at 77 percent and 85 percent, respectively, with up to 100 percent achieving successful micturition. Complications are most commonly urologic and include strictures, fistulation, flap loss, and aesthetic revision. Additional options exist, such as facial feminization or masculinization surgery, but outcomes have not been as well studied in the literature.31 Overall, regret due to bottom surgery is reported in the literature between 0.0 and 2.2 percent. Despite the well-documented benefits of gender-affirming care and guidelines by the World Professional Association for Transgender Health (WPATH), a 2020 cross-sectional analysis found that only about 10 percent of insurance providers offer favorable coverage for bottom surgery, defined as establishing policies covering gender-affirming surgery that adhere to WPATH guidelines (i.e., coverage of reconstructive surgeries matching WPATH guidelines, coverage for the age of majority [generally 18 years of age, but varies by state], diagnositc criteria for gender dysphoria, eligibility for hormone therapy, duration of only 12 months living in the congruent gender role, referral from one to two mental health providers not requiring doctoral designations, no requirement for legal name change, and options for fertility preservation). Excessive insurance criteria often include legal name changes and diagnosis of gender dysphoria, complicating accessibility even in plans which otherwise cover gender-affirmation surgery.32 Provider advocacy and knowledge again become paramount in providing treatment.
Nonaccess to gender-affirming surgery has been shown to confer 73-percent greater odds of SAs in transgender patients.16 Indeed, the literature suggests that one of the most significant interventions by which providers may assist patients is letter writing. Both hormone therapy and gender-affirming surgery are often difficult for patients to access or obtain, frequently due to legal red tape or insurance requirements. These barriers can be addressed and reduced with letter writing by physicians, showing support and emphasizing the appropriateness and necessity of the medical treatment, even if said physician is not the person who is providing the treatment. Furthermore, some insurance campaigns specifically require these letters and evaluations from two or more providers. Access to gender-affirmation surgery thus extends beyond the sole reach of the surgeon and into the domains of cross-specialty providers, highlighting the importance of interdisciplinary knowledge and gender-affirming care.33
Advocacy and involvement in policymaking are likewise important means of provider support and intervention. One study found that statewide marriage equality laws correlated significantly with lower rates of SAs in transgender and sexual minority youth.25 Even the rare provider who will never see a transgender patient is still able to effect change as an ally through their voice and power of advocacy.
Transgender Care in Medical and Continuing Education
In 2018, a survey found that 80 percent of medical students across 10 different medical schools did not feel competent treating transgender patients.7 A separate study of 150 medical schools across Canada and the US found that the median time dedicated to LGBTQ+ curriculum was five hours, with presumably far less pertaining to transgender or gender-affirming care.20 In order to provide gender-affirming care, it is essential that providers and medical staff first be educated on this issue. The provider who is currently reading this article is taking one step in that effort. To systemically improve inclusive and gender-affirming care, this must be taught and emphasized in medical and nursing schools, resident and medical assistant education and training, continuing education programs, and other educational services. While many medical schools are beginning to include inclusive care and LGBTQ+ education, many programs still do not do so, and most undergraduate and postgraduate medical education programs are lacking in this regard. Further still, absence of gender identity terminology and definitions in medical education limit the accuracy and representativity of research and epidemiology; many demographic delineations of research studies are broken into the gender binary, incorrectly representing or entirely ignoring gender minorities, such as transgender and nonbinary individuals.2 Education among the allied health professions should likewise include inclusive and gender-affirming healthcare education, yet a 2020 integrative review by Lightfoot et al17 found this to also be lacking in undergraduate curriculum, nursing curriculum, and clinical research.
The literature shows that providers identify insufficient formal training on transgender health in residency and medical school as a significant barrier to appropriate care for these patients.12 It should be encouraged and standardized that gender-affirming care, hormone therapy, gender-affirming surgery, and trauma-informed care are included across medical education longitudinally, rather than in one individual endocrinology lesson or public health session. These subjects should be included and normalized in medical education, licensing exams, and everyday discussion to better normalize these issues and reduce stigma and disparities for this vulnerable population.
Clinical Pearls
- The only way to know the gender of a person is by asking them.
- Gender identity extends along a spectrum and is nonbinary, including but not limited to cisgender male, cisgender female, transgender male, transgender female, gender nonbinary, genderfluid, genderqueer, and gender nonconforming.
- Gender is subject to change and may not be a permanent quality.
- Trauma-informed care should be a pillar of treatment for all patients, but especially for transgender and LGBTQ+ patients.
- Transgender patients experience disparities across the spectrum of psychiatric illness, including SI and SA; however, this is preventable with intervention and gender-affirming care.
- Providing gender-affirming care begins with the first encounter of a patient in the provider’s waiting room, phoneline, or website.
- Inclusive environments may be established by clearly posting nondiscrimination statements, providing easily accessible gender-neutral restrooms, using gender-neutral language, stating one’s pronouns, and effectively educating all staff.
- Positive health outcomes are consistently correlated with gender-affirming and gender-supportive providers and support systems.
- Letter writing is a powerful tool for providers to extend access to gender-affirmation surgery.
- Graduate medical education, postgraduate medical education, and continuing education should adequately include issues of gender-affirming care, hormone therapy, gender-affirming surgery, and trauma-informed care.
Conclusion
Gender is a social construct, yet it continues to be a daily and ongoing stressor and point of discrimination for transgender and gender-minority individuals. Transgender patients experience disproportionate disparities in mental health, physical health, homelessness, and violence. These disparities are not inevitable, however. Gender-affirming care has consistently been shown to improve quality of life, improve health outcomes, and reduce rates of SI and SAs. Healthcare providers and medical staff, regardless of field or specialty, have the opportunity and responsibility to provide sensitive and gender-affirming care and hold the power to positively influence patient quality of life and even life expectancy. Gender-neutral language, explicit use of personal pronouns, and sensitive physical exams can all have dramatic effects on the patient experience and ability to establish rapport. Providers also hold significant power of advocacy and can help patients from both an individual and systemic level. Gender-affirming care starts the moment that the patient schedules or considers scheduling an appointment, but must continue through every interaction, great or small, thereafter.
References
- Roen K. Intersex or diverse sex development: critical review of psychosocial health care research and indications for practice. J Sex Res. 2019;56(4–5):511–528.
- Rushton A, Gray L, Canty J, Blanchard K. Beyond binary: (re)defining “gender” for 21st century disaster risk reduction research, policy, and practice. Int J Environ Res Public Health. 2019;16(20):3984.
- Catalpa JM, McGuire JK, Fish JN, et al. Predictive validity of the genderqueer identity scale (GQI): differences between genderqueer, transgender and cisgender sexual minority individuals. Int J Transgenderism. 2019;20(2–3):305–314.
- Bloom TM, Nguyen TP, Lami F, et al. Measurement tools for gender identity, gender expression, and gender dysphoria in transgender and gender-diverse children and adolescents: a systematic review. Lancet Child Adolesc Heal. 2021;5(8):582–588.
- Mizock L, Kenner C, DiStefano A, et al. LGBTQ community needs and assets assessment of a sexual health clinic: a brief report. Sex Cult. 2021;25(5):1673–1689.
- Stroumsa D, Shires DA, Richardson CR, et al. Transphobia rather than education predicts provider knowledge of transgender health care. Med Educ. 2019;53(4):398–407.
- Caceres BA, Streed CG, Corliss HL, et al. Assessing and addressing cardiovascular health in LGBTQ adults: a scientific statement from the American Heart Association. Circulation. 2020;142(19):e321–e332.
- Wesp LM, Malcoe LH, Elliott A, Poteat T. Intersectionality research for transgender health justice: a theory-driven conceptual framework for structural analysis of transgender health inequities. Transgend Health. 2019;4(1):287–296.
- Clark K, Fletcher JB, Holloway IW, Reback CJ. Structural inequities and social networks impact hormone use and misuse among transgender women in Los Angeles county. Arch Sex Behav. 2018;47(4):953–962.
- Edmiston EK, Donald CA, Sattler AR, et al. Opportunities and gaps in primary care preventative health services for transgender patients: a systematic review. Transgend Health. 2016;1(1):216–230.
- DiNenno EA, Prejean J, Irwin K, et al. Recommendations for HIV screening of gay, bisexual, and other men who have sex with men—United States, 2017. MMWR Morb Mortal Wkly Rep. 2017;66(31):830–832.
- Ingham MD, Lee RJ, MacDermed D, Olumi AF. Prostate cancer in transgender women. Urol Oncol Semin Orig Investig. 2018;36(12):518–525.
- Peitzmeier SM, Malik M, Kattari SK, et al. Intimate partner violence in transgender populations: systematic review and meta-analysis of prevalence and correlates. Am J Public Health. 2020;110(9):E1–E14.
- Antebi-Gruszka N, Scheer JR. Associations between trauma-informed care components and multiple health and psychosocial risks among LGBTQ survivors of intimate partner violence. J Ment Heal Couns. 2021;43(2):139–156.
- Ljungholm DP, Olah ML. COVID-19-related health inequities and biopsychosocial stressors experienced by LGBTQ+ people. 2021;11(1):101–111.
- Zwickl S, Wong AFQ, Dowers E, et al. Factors associated with suicide attempts among Australian transgender adults. BMC Psychiatry. 2021;21(1):1–10.
- Lightfoot S, Kia H, Vincent A, et al. Trans-affirming care: an integrative review and concept analysis. Int J Nurs Stud. 2021;123:104047.
- María Del Río-González A. To Latinx or not to Latinx: a question of gender inclusivity versus gender neutrality. Am J Public Health. 2021;111(6):1018–1021.
- Rocco D, De Bei F, Negri A, Filipponi L. The relationship between self-observed and other-observed countertransference and session outcome. Psychotherapy (Chic). 2021;58(2):301–309.
- Eisenberg ME, McMorris BJ, Rider GN, et al. “It’s kind of hard to go to the doctor’s office if you’re hated there.” A call for gender-affirming care from transgender and gender diverse adolescents in the United States. Health Soc Care Community. 2020;28(3):1082–1089.
- Gülgöz S, Glazier JJ, Enright EA, et al. Similarity in transgender and cisgender children’s gender development. Proc Natl Acad Sci U S A. 2019;116(49):24480–24485.
- Becerra-Culqui TA, Liu Y, Nash R, et al. Mental health of transgender and gender nonconforming youth compared with their peers. Pediatrics. 2018;141(5):e20173845.
- Ashley F. Thinking an ethics of gender exploration: against delaying transition for transgender and gender creative youth. Clin Child Psychol Psychiatry. 2019;24(2):223–236.
- George R, Stokes MA. Gender identity and sexual orientation in autism spectrum disorder. Autism. 2018;22(8):970–982.
- Coulter RWS, Egan JE, Kinsky S, et al. Mental health, drug, and violence interventions for sexual/gender minorities: a systematic review. Pediatrics. 2019;144(3):e20183367.
- Handler T, Hojilla JC, Varghese R, et al. Trends in referrals to a pediatric transgender clinic. Pediatrics. 2019;144(5):e20191368.
- Olson-Kennedy J, Warus J, Okonta V, et al. Chest reconstruction and chest dysphoria in transmasculine minors and young adults’ comparisons of nonsurgical and postsurgical cohorts. JAMA Pediatr. 2018;172(5):431–436.
- Poquiz J, Moser CN, Grimstad F, et al. Gender-affirming care in the midwest: reaching rural populations. J Rural Ment Health. 2021;45(2):121–128.
- Martinez C, Rikhi R, Haque T, et al. Gender identity, hormone therapy, and cardiovascular disease risk. Curr Probl Cardiol. 2020;45(5):100396.
- Willis P, Dobbs C, Evans E, et al. Reluctant educators and self-advocates: older trans adults’ experiences of health-care services and practitioners in seeking gender-affirming services. Health Expect. 2020;23(5):1231–1240.
- Akhavan AA, Sandhu S, Ndem I, Ogunleye AA. A review of gender affirmation surgery: what we know, and what we need to know. Surgery. 2021;170(1):336–340.
- Ngaage LM, Knighton BJ, Benzel CA, et al. A review of insurance coverage of gender-affirming genital surgery. Plast Reconstr Surg. 2020;145(3):803–812.
- Budge SL. Psychotherapists as gatekeepers: an evidence-based case study highlighting the role and process of letter writing for transgender clients. Psychotherapy. 2015;52(3):287–297.
